🚧 Clogged Pipes 101
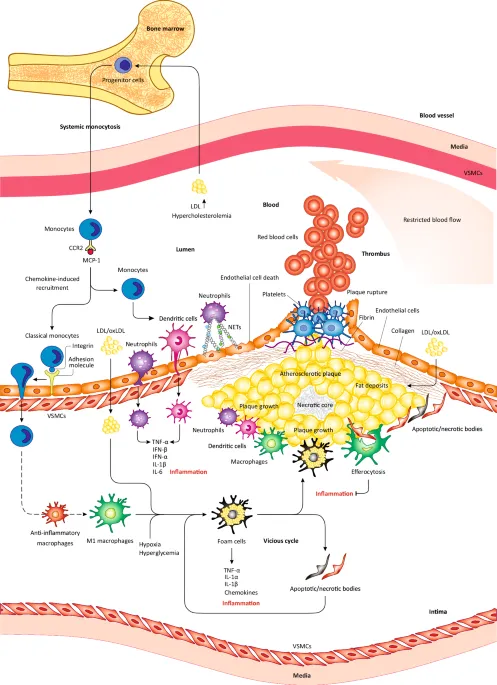
Primarily driven by atherosclerosis, a systemic inflammatory process. Risk factors (smoking, DM, HTN, HLD) cause endothelial injury, leading to lipid deposition and chronic inflammation within the vessel wall.
⭐ Most common site: Superficial femoral artery (SFA) in the adductor (Hunter's) canal.
🦵 Clinical Manifestations - Signs of the Struggle
-
Chronic Ischemia (Gradual Occlusion):
- Skin: Cool, shiny, thin, atrophic with hair loss (alopecia).
- Color: Pallor on elevation; dependent rubor (Buerger's sign) when lowered.
- Pulses: Diminished or absent distal pulses (dorsalis pedis, posterior tibial).
- Ulcers: Painful, "punched-out" ulcers with a pale base, typically on toes or pressure points.
- Nails: Thickened, brittle; muscle atrophy.
-
⚠️ Acute Limb Ischemia (Sudden Occlusion):
- 📌 The 6 P's: Pain, Pallor, Pulselessness, Paresthesia, Paralysis, Poikilothermia (coolness).
⭐ Leriche Syndrome (aortoiliac occlusion): Triad of 1) bilateral hip/thigh/buttock claudication, 2) absent/diminished femoral pulses, and 3) impotence.
🩺 Diagnosis - Catching the Culprit
-
History & Physical: Classic symptoms are intermittent claudication and rest pain. Signs include diminished pulses, pallor on elevation, dependent rubor, shiny atrophic skin, and non-healing ulcers (typically on toes/foot).
-
Ankle-Brachial Index (ABI): Best initial test.
- Formula: $ABI = \frac{\text{Highest Ankle Systolic Pressure}}{\text{Highest Brachial Systolic Pressure}}$
- ABI Values & Interpretation:
- > 1.4: Non-compressible/calcified vessels (DM, CKD).
- 0.91 - 1.4: Normal.
- 0.41 - 0.90: Mild to moderate PAD.
- ≤ 0.40: Severe PAD / Critical Limb Ischemia (CLI).
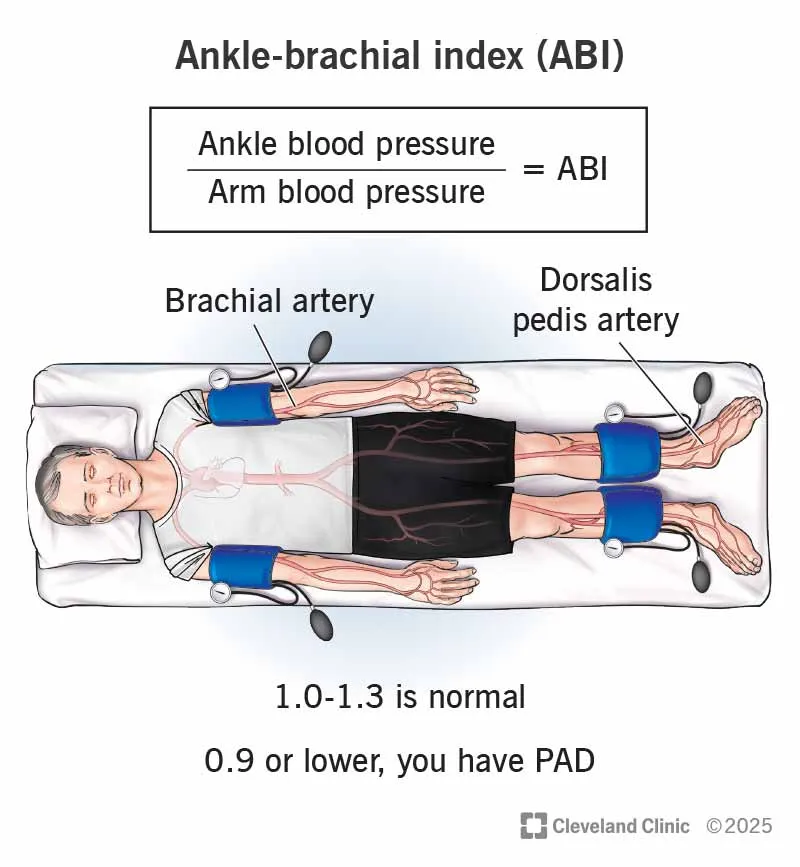
⭐ If ABI is > 1.4, it's unreliable. A Toe-Brachial Index (TBI) is the next step, as digital arteries are less prone to calcification. A TBI < 0.7 is diagnostic for PAD.
- Imaging for Intervention:
- Arterial Duplex Ultrasound: First-line imaging to localize stenosis and assess flow.
- CTA/MRA: Gold standard for detailed anatomical mapping before surgery/endovascular procedures.
🌊 Management - Opening the Floodgates
-
Cornerstone (All Patients):
- Risk Factor Modification:
- Smoking Cessation: Single most important intervention.
- BP & Glycemic Control: Target BP <130/80, HbA1c <7%. ACEi/ARBs are preferred.
- Medical Therapy:
- Antiplatelet: Aspirin (81mg) or Clopidogrel.
- Statin: High-intensity (e.g., Atorvastatin 40-80mg) for all; PAD is an ASCVD equivalent.
- Risk Factor Modification:
-
Symptomatic Claudication:
- Supervised Exercise Program: First-line. Walk until near-maximal pain, rest, repeat.
- Cilostazol: PDE-3 inhibitor for refractory symptoms. ⚠️ Contraindicated in heart failure.
⭐ A structured, supervised exercise program is as effective as angioplasty for improving walking distance in patients with claudication.
- Critical Limb Ischemia (CLI) / Refractory Disease:
- Revascularization: Restore blood flow.
- Endovascular: Angioplasty ± Stenting.
- Surgical: Bypass graft (e.g., fem-pop), endarterectomy.
- Revascularization: Restore blood flow.
⚡ High-Yield Points - Biggest Takeaways
- Ankle-Brachial Index (ABI) < 0.9 is the best initial diagnostic test.
- Intermittent claudication (exertional leg pain relieved by rest) is the hallmark symptom.
- Smoking is the most significant modifiable risk factor.
- Initial management: risk factor modification (statins, BP control) and a supervised exercise program.
- Cilostazol for symptomatic relief; aspirin or clopidogrel for secondary prevention.
- Acute limb ischemia (the "6 P's") is a surgical emergency requiring immediate revascularization.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

