🧠 Core concept - Plaque Problem Primer
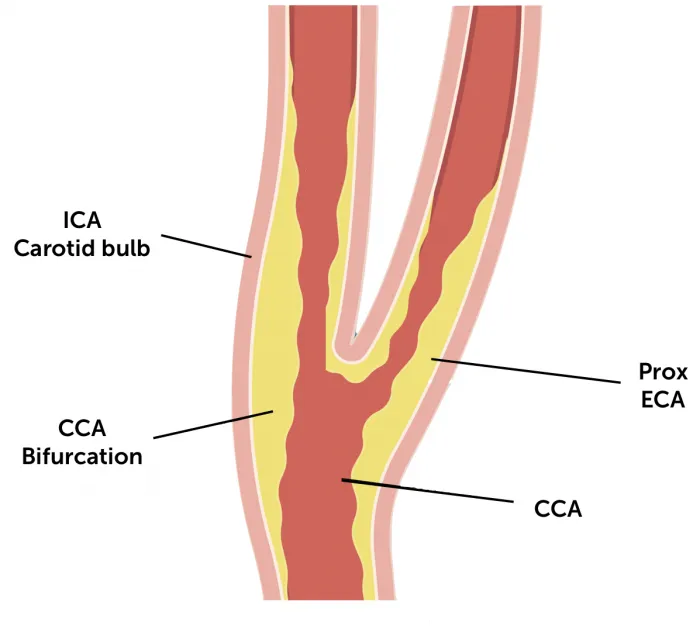
- Pathology: Atherosclerosis forms plaques, primarily at the carotid bifurcation, the origin of the Internal Carotid Artery (ICA).
- Mechanism of Ischemia:
- Embolism (most common): Unstable plaque ruptures, sending thromboembolic debris to the brain → TIA/stroke.
- Hemodynamic: Severe stenosis causes low flow, especially with systemic hypotension.
- Plaque Risk: Ulcerated, soft, lipid-rich plaques are more prone to rupture and embolization than calcified, stable plaques.
⭐ The most common site for carotid atherosclerosis is the posterior wall of the carotid bulb at the origin of the internal carotid artery.
🧠 Clinical Manifestations - Stroke Signals
Symptoms reflect cerebral ischemia, typically from embolism off an atherosclerotic plaque or severe hypoperfusion.
- Transient Ischemic Attack (TIA): Focal neurologic deficits that resolve completely within 24 hours.
- Amaurosis Fugax: Transient, painless monocular blindness, often described as a "curtain falling down."
- Contralateral hemiparesis or hemisensory loss.
- Aphasia (if the dominant hemisphere is affected).
- Stroke (CVA): Neurologic deficits that persist for > 24 hours.
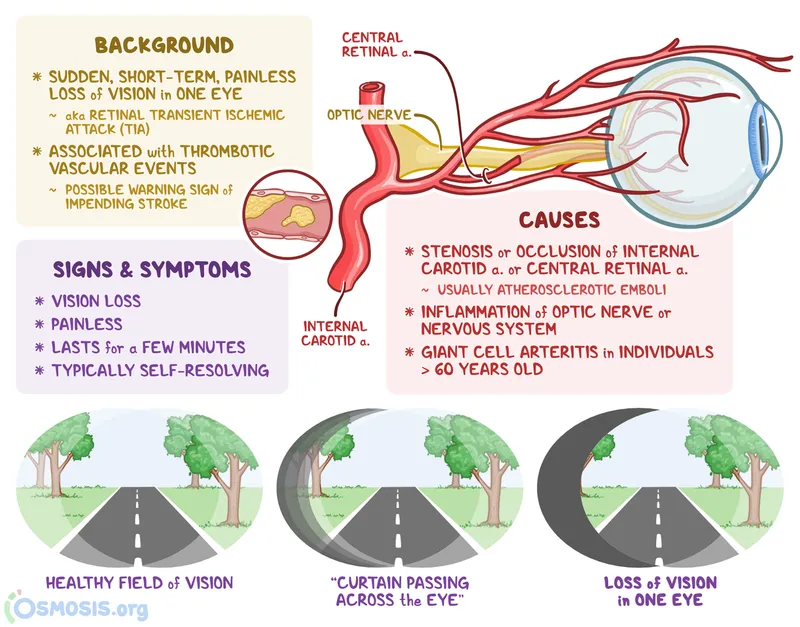
⭐ Amaurosis fugax is a classic sign of ipsilateral internal carotid artery disease, caused by emboli lodging in the retinal artery.
🩺 Diagnosis - Finding the Fault
- Initial Test: Carotid Duplex Ultrasound. Non-invasive, uses ↑ peak systolic velocity (PSV) and end-diastolic velocity (EDV) to estimate stenosis severity.
- Confirmatory Imaging: CT Angiography (CTA) or MR Angiography (MRA). Provides detailed anatomy of the aortic arch, carotid bifurcation, and intracranial circulation for pre-operative planning.
- Gold Standard: Digital Subtraction Angiography (DSA). Most accurate but invasive (0.5-1% stroke risk), reserved for discrepancies.
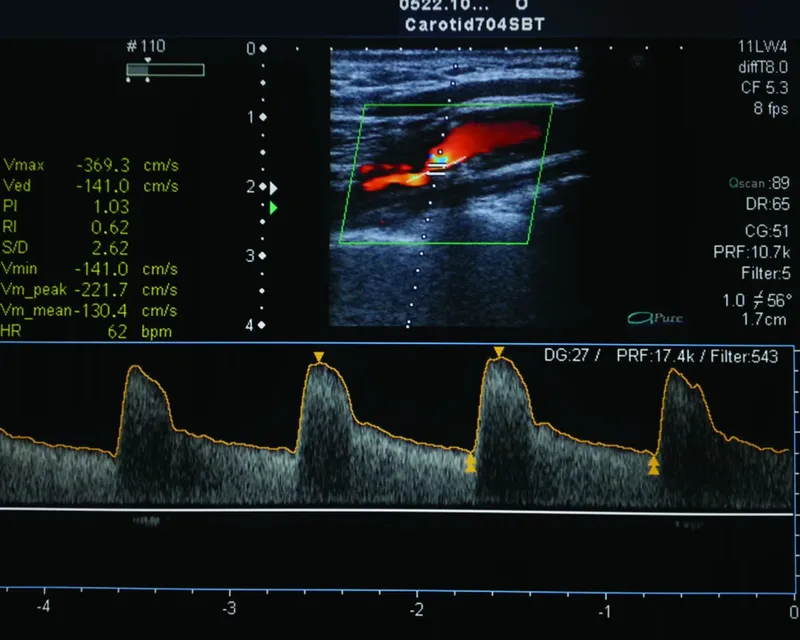
⭐ NASCET Criteria: The standard for measuring stenosis. % Stenosis = (1 - [Diameter of stenosis / Diameter of normal distal ICA]) x 100. This method is crucial for trial-based indications.
🔪 Management - The Scalpel Solution
- Indications for Carotid Endarterectomy (CEA):
- Symptomatic: Recent TIA or non-disabling stroke.
- Stenosis >70%: Clear benefit.
- Stenosis 50-69%: Benefit for select patients (e.g., male, recent stroke).
- Asymptomatic:
- Stenosis >60% in patients with >5-year life expectancy and low perioperative risk (<3%).
- Symptomatic: Recent TIA or non-disabling stroke.
⭐ Most common cranial nerve injury during CEA is the hypoglossal (CN XII), causing tongue deviation towards the lesion upon protrusion.
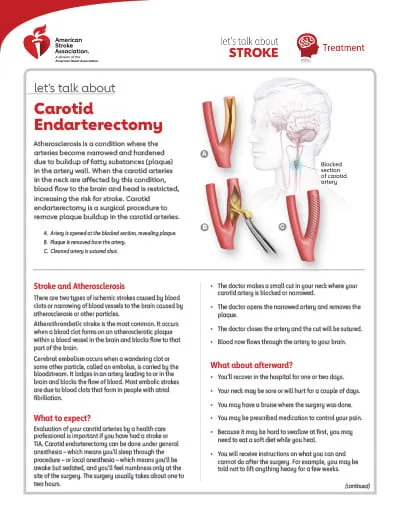
⚠️ Complications - Post-Op Pitfalls
- Stroke/TIA: Most feared. Immediate post-op suggests thrombosis (return to OR); later suggests embolism.
- Cranial Nerve Injury:
- CN XII (Hypoglossal): Tongue deviates to ipsilateral side.
- CN X (Vagus): Hoarseness.
- CN VII (Marginal Mandibular): Asymmetric smile.
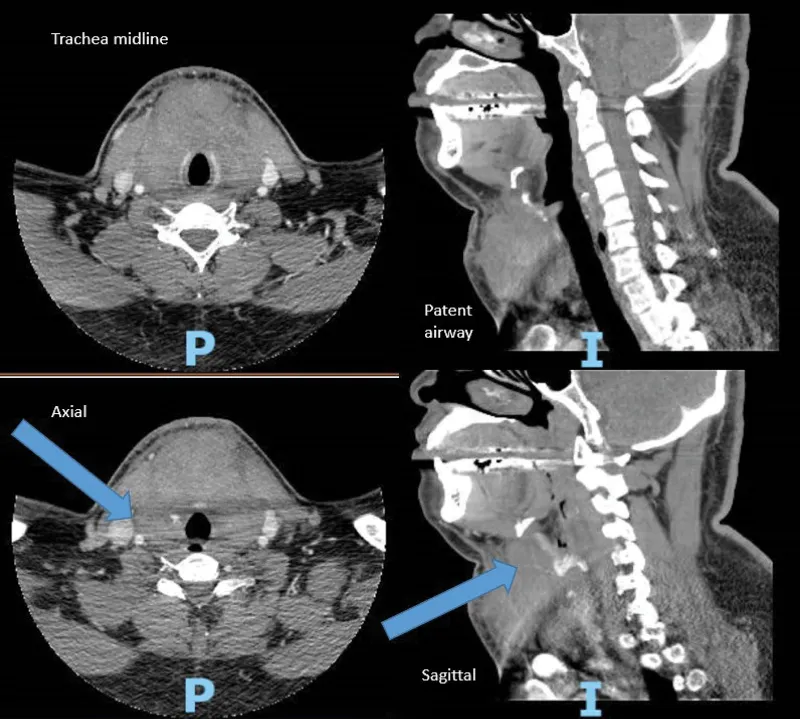
- Neck Hematoma: ⚠️ Can cause airway compromise. Requires urgent re-exploration.
- Carotid Sinus Instability: Labile BP.
⭐ Hyperperfusion Syndrome: Rare but severe. Presents with ipsilateral headache, seizures, and focal neurological deficits days after reperfusion.
⚡ High-Yield Points - Biggest Takeaways
- Symptomatic patients (TIA/stroke): CEA is indicated for stenosis >70%. Consider for 50-69%, especially in men.
- Asymptomatic patients: CEA for stenosis >80% only if life expectancy is >5 years and perioperative risk is low.
- Most feared complication is perioperative stroke from embolism or thrombosis.
- Cranial nerve injuries: Hypoglossal (CN XII) → tongue deviation; Vagus (CN X) → hoarseness.
- Post-op hyperperfusion syndrome: severe headache, seizures, focal deficits.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

