🗺️ The Rerouting Plan
Bypass grafting reroutes blood flow around an arterial blockage using a conduit. Anastomosis connects the graft proximally and distally to the healthy artery.
- Graft Types & Hierarchy:
- Autologous (Vein/Artery): Best choice. ↑Patency, ↓infection risk.
- Great Saphenous Vein (GSV): Gold standard for leg bypass (reversed or in-situ).
- Other: Arm veins (cephalic), IMA (for CABG).
- Prosthetic (Synthetic): Used if no autologous conduit is available.
- PTFE: Common for above-knee fem-pop bypass.
- Dacron: For large vessels (e.g., aortofemoral).
- Autologous (Vein/Artery): Best choice. ↑Patency, ↓infection risk.
⭐ For below-the-knee bypasses, autologous vein grafts (especially GSV) have significantly higher long-term patency rates than prosthetic grafts.
🧬 Anatomy - Pipes & Tubes
-
Principle: Create a new path for blood flow around an occluded or stenotic arterial segment. Choice of conduit is critical for success.
-
Graft Material Comparison:
| Graft Type | Material | Best Use Case | Patency | Infection Risk |
|---|---|---|---|---|
| Autologous | Great Saphenous Vein (GSV) | Infra-inguinal (below knee) | Highest | Lowest |
| Internal Mammary Artery | Coronary Artery Bypass (CABG) | Excellent | Low | |
| Prosthetic | PTFE (e.g., Gore-Tex®) | Supra-inguinal (above knee), AV access | Good (high flow) | Moderate |
| Dacron | Aortoiliac, thoracic aorta | Good (large caliber) | High |
- **Reversed:** Vein is excised, flipped 180° so valves don't impede flow.
- **In-situ:** Vein left in its native bed; valves are destroyed with a valvulotome.
⭐ For infra-inguinal bypasses (e.g., femoropopliteal), autologous great saphenous vein is the conduit of choice, offering superior long-term patency and resistance to infection compared to prosthetic grafts.
🕵️♂️ Management - Post-Op Patrol
-
Immediate Care: Vigilant monitoring for hemorrhage, hematoma, compartment syndrome, and acute graft thrombosis. Perform hourly neurovascular checks (pulses, motor, sensory).
-
Long-Term Surveillance: A structured protocol is essential for maintaining long-term graft patency. This involves regular clinical evaluation and non-invasive imaging to detect failing grafts before occlusion.
-
Key Metrics:
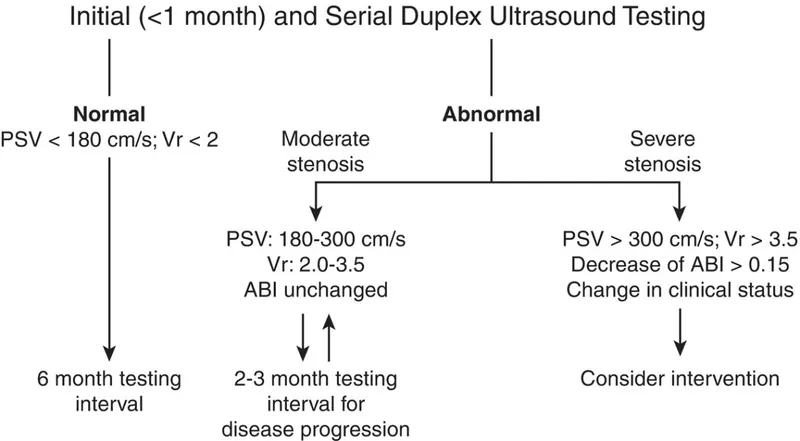
- Ankle-Brachial Index (ABI): A sustained drop of >0.15 from post-op baseline suggests impending graft failure.
- Duplex Ultrasound: Primary tool. Peak Systolic Velocity (PSV) ratio >2.5 indicates >50% stenosis.
⭐ Early graft failure (<30 days) is often due to technical error or thrombosis. Failure from 1-24 months is typically from intimal hyperplasia, especially at anastomotic sites. Late failure is due to atherosclerosis.
📉 Complications - When Bypasses Fail
- Graft failure is categorized by time of onset, which strongly suggests the underlying cause.
- Early Failure (<30 days):
- Technical Error: Anastomotic flaw, graft kinking, retained valve cusp (in-situ vein).
- Thrombosis: Due to poor runoff, hypercoagulable state, or low flow.
- Intermediate Failure (1 mo - 2 yrs):
- Neointimal Hyperplasia: Proliferation of smooth muscle cells at the anastomosis, causing stenosis.
- Late Failure (>2 yrs):
- Progressive Atherosclerosis: New disease in inflow/outflow vessels.
- Graft material degeneration (e.g., vein graft aneurysm).
⭐ Intimal hyperplasia is the most common cause of infrainguinal vein graft failure between 1 month and 2 years post-op. It's a key target for surveillance.
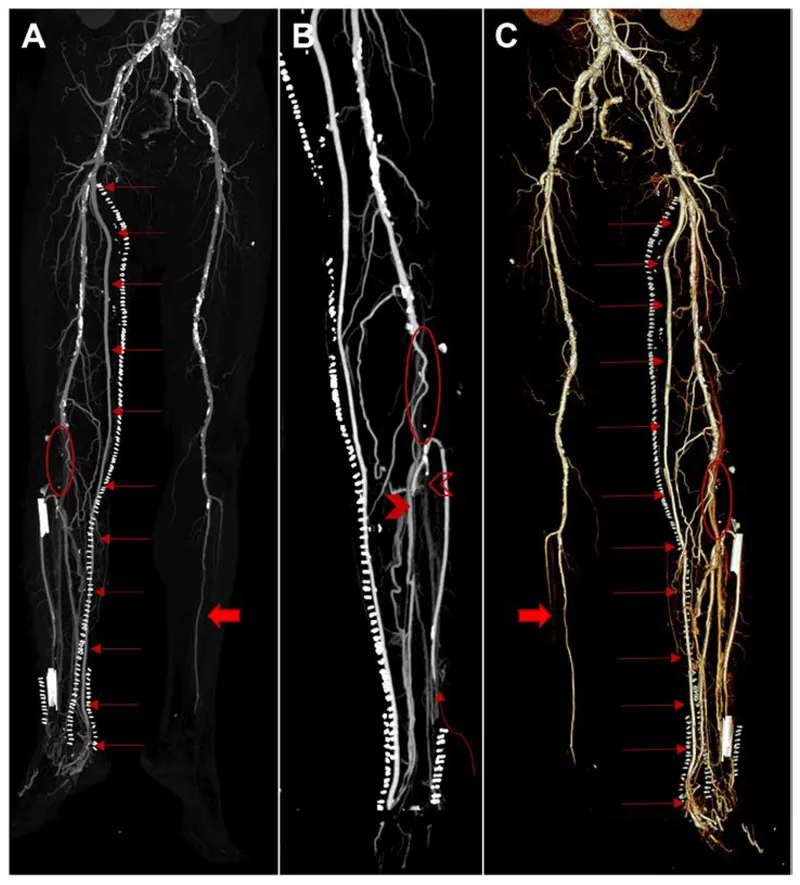
- Diagnosis: ↓ Ankle-Brachial Index (ABI), duplex ultrasound, CTA/MRA, or catheter angiography.
⚡ Biggest Takeaways
- Autologous saphenous vein is the gold standard for below-knee bypass due to superior patency and infection resistance.
- Prosthetic grafts (e.g., PTFE) are used for high-flow, large-caliber vessels (above-knee) or when vein is unavailable.
- In-situ technique leaves the vein in its native bed, requiring valve lysis.
- Reversed vein graft involves excising and flipping the vein to render valves incompetent.
- Most common cause of late graft failure is intimal hyperplasia at the distal anastomosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

