🧬 Pathophysiology - Why the Wall Fails
- Core Defect: A tear in the tunica intima allows high-pressure blood to enter and split the tunica media, creating a false lumen.
- Histology: Cystic medial necrosis (degeneration) is the hallmark, weakening the aortic wall.
- Key Associations:
- Chronic Hypertension (most common, >75%)
- Genetic: Marfan, Ehlers-Danlos
- Congenital: Bicuspid aortic valve
⭐ The primary event is an intimal tear, not a ruptured vasa vasorum. Hypertension provides the necessary shear stress.
💥 The Sudden Rip
- Pain: Abrupt, severe, "tearing" or "ripping" chest pain.
- Radiation Pattern:
- Anterior chest → Ascending aorta (Type A).
- Interscapular back → Descending aorta (Type B).
- Vascular Signs:
- Pulse deficits (unequal radial/femoral pulses).
- BP differential >20 mmHg between arms.
- Cardiac: New aortic regurgitation murmur (diastolic), hypotension, tamponade.
- Neurologic: Syncope, stroke, Horner's syndrome, paraplegia.
⭐ A variation in systolic blood pressure >20 mmHg between arms is a classic, high-specificity finding.
🩺 Diagnosis - Spotting the Tear
- Initial Tests:
- CXR: Widened mediastinum (>8 cm), pleural effusion.
- ECG: Rules out primary MI; may show nonspecific changes or inferior MI if RCA is involved.
- Definitive Imaging:
- CTA (Chest/Abd/Pelvis): Gold standard for stable patients.
- TEE (Transesophageal Echo): Best for unstable patients or renal failure.
⭐ CXR: A widened mediastinum is the most common finding, but a normal CXR does not rule out dissection.
🚑 Management - Race Against Time
- Initial Medical Stabilization (ALL types):
- Admit to ICU, place arterial line for continuous BP monitoring.
- Primary Goal: Rapidly ↓ BP & ↓ HR to reduce aortic wall stress ($dP/dt$) and limit extension.
- Targets: SBP 100-120 mmHg, HR <60 bpm, achieved within minutes.
- Pharmacology Sequence:
- 1st: IV β-blockers (Labetalol, Esmolol) to control heart rate.
- 2nd: Add IV vasodilator (Nitroprusside, Nicardipine) if SBP remains elevated.
⭐ Beta-blocker BEFORE vasodilator! Isolated vasodilation causes reflex tachycardia, increasing aortic shear stress and worsening the dissection.
- Definitive Treatment by Type:
dominoes Complications - The Deadly Dominoes
- Rupture: Most lethal event.
- Into pericardium → Cardiac Tamponade (Beck's triad: hypotension, JVD, muffled heart sounds).
- Into pleura → Massive Hemothorax.
- Malperfusion (Branch Occlusion): Ischemia/infarction of end-organs.
- Coronary a. → MI (often RCA).
- Carotid/Vertebral a. → Stroke.
- Spinal a. → Paraplegia.
- Renal a. → AKI, severe HTN.
- Aortic Regurgitation: New diastolic murmur from valve incompetence.
⭐ Cardiac tamponade is the #1 cause of death in Type A dissection. It's a primary indication for emergent surgical intervention.
⚡ Biggest Takeaways
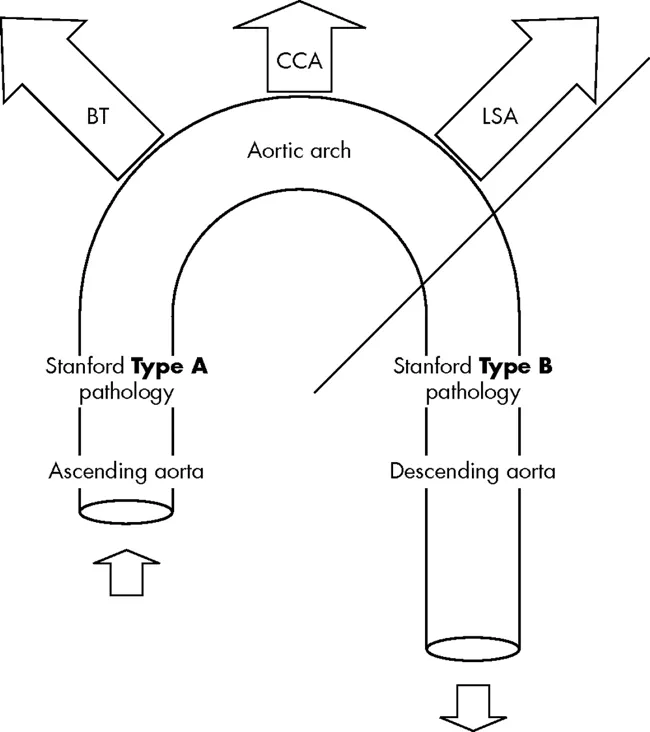
- Stanford Type A (involving ascending aorta) is a surgical emergency.
- Stanford Type B (descending aorta only) is managed medically unless complicated (e.g., malperfusion, rupture).
- Initial management for ALL types: IV beta-blockers (labetalol, esmolol) to target HR <60 & SBP 100-120 mmHg.
- Add vasodilators (nitroprusside) only after achieving heart rate control to avoid reflex tachycardia.
- Hypertension is the single most important risk factor.
- CT angiography is the gold standard for diagnosis in stable patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

