🧱 Core concept & Pathophysiology - The Blocked Dam
Inability to voluntarily void, leading to ↑ post-void residual (PVR).
- Acute: Painful inability to void.
- Chronic: Painless; may present with overflow incontinence.
Two Core Mechanisms:
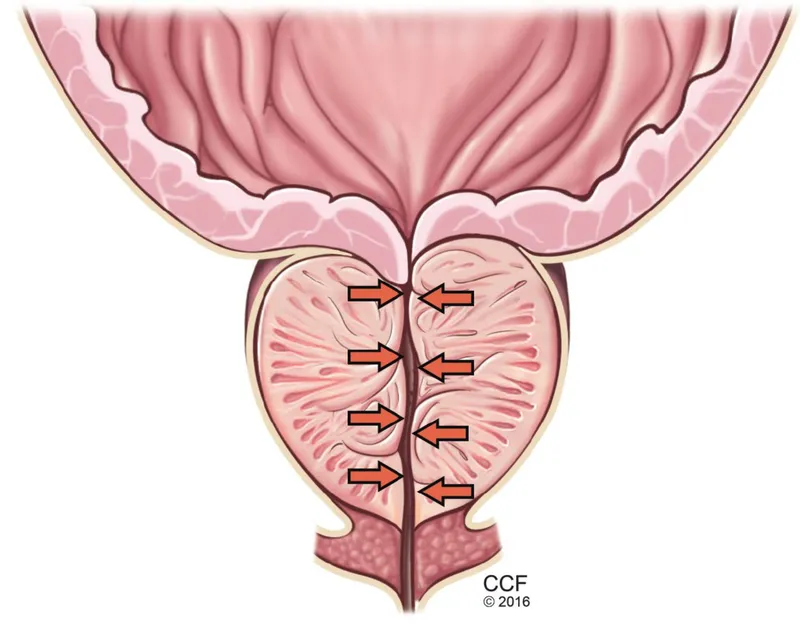
- Bladder Outlet Obstruction (BOO): A physical blockage.
- Most Common: Benign Prostatic Hyperplasia (BPH) in men.
- Others: Urethral strictures, stones, malignancy.
- Detrusor Underactivity (DU): Impaired bladder contractility.
- Neurogenic: Spinal cord injury, MS, diabetic neuropathy.
- Pharmacologic: Anticholinergics, opioids.
- Myogenic: Chronic overdistension injury.
⭐ Post-Operative Urinary Retention (POUR) is common. Anesthesia and opioids impair detrusor contractility and bladder sensation.
📌 Mnemonic (DAMN): Drugs, Anatomic, Myogenic, Neurogenic.
🩺 Diagnosis - Finding the Fault
- Presentation: Patient reports acute inability to void, severe suprapubic pain, and restlessness, sometimes with overflow incontinence. Physical exam reveals a palpable, firm, suprapubic mass (the bladder) that is dull to percussion.
- Diagnostic Flow:
- Workup:
- Catheterization: Confirms diagnosis, measures PVR, and provides immediate relief.
- Labs: Check BUN/Cr for post-renal AKI. Urinalysis to rule out UTI.
- DRE: Essential to evaluate for BPH, prostate cancer, or fecal impaction.
⭐ A post-void residual (PVR) >200 mL is diagnostic. Acute retention often involves volumes >500 mL, risking post-obstructive diuresis after decompression.
🌊 Management - Releasing the Floodgates
Immediate Goal: Prompt bladder decompression to prevent renal damage and provide relief.
- 1st Line: Urethral (Foley) catheter.
- Use a coudé tip catheter for suspected BPH.
- 2nd Line: Suprapubic catheter if urethral access fails (e.g., stricture, false passage) or is contraindicated (urethral trauma).
Post-Decompression Monitoring:
- ⚠️ Post-Obstructive Diuresis (POD):
- Definition: Urine output > 200 mL/hr for ≥2 consecutive hours after catheterization.
- Pathophys: Physiologic diuresis of retained fluid/solutes; can become pathologic.
- Action: Monitor vitals, electrolytes (Na+, K+), and volume status. Replace fluids if hypotensive.
Long-Term Strategy:
- Address the underlying cause (e.g., stop anticholinergics, treat BPH).
- Plan for a Trial Without Catheter (TWOC).
⭐ High-Yield Pearl: For BPH-induced retention, start an alpha-1 blocker (e.g., tamsulosin) 1-3 days before attempting a TWOC to maximize success by relaxing the bladder neck and prostatic smooth muscle.
💥 Complications - The Aftermath
- Post-Obstructive Diuresis (POD):
- Massive polyuria (>200 mL/hr) after decompression.
- Risks: Dehydration, hypotension, electrolyte loss (↓Na⁺, ↓K⁺).
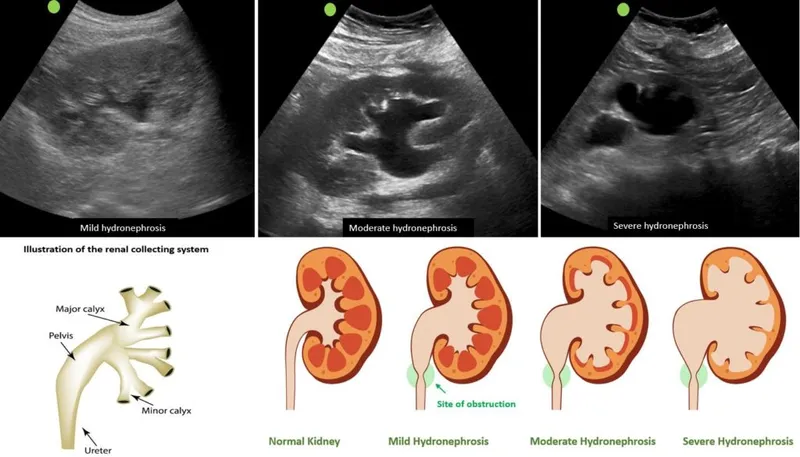
- Hydronephrosis & Renal Damage:
- ↑ back-pressure → renal pelvis dilation → AKI/CKD.
- Infection & Sepsis:
- Urine stasis promotes bacterial growth (UTI, pyelonephritis).
- Bladder Atony:
- Chronic overdistension damages detrusor muscle, causing poor contractility.
⭐ Post-obstructive diuresis is a physiologic response to excrete retained fluid/solutes. Monitor urine output closely; pathologic diuresis may require IV fluid replacement.
⚡ Biggest Takeaways
- Immediate management is bladder decompression via Foley or suprapubic catheter.
- Always monitor for post-obstructive diuresis (POD) (>200 mL/hr); manage with IV fluids.
- Benign Prostatic Hyperplasia (BPH) is the most common cause in men; initiate alpha-blockers (e.g., tamsulosin).
- Acute retention is painful; chronic retention is often painless with overflow incontinence.
- After stabilization, perform a Trial Without Catheter (TWOC), especially after starting BPH meds.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

