Anatomy & Classification - The Pelvic Puzzle
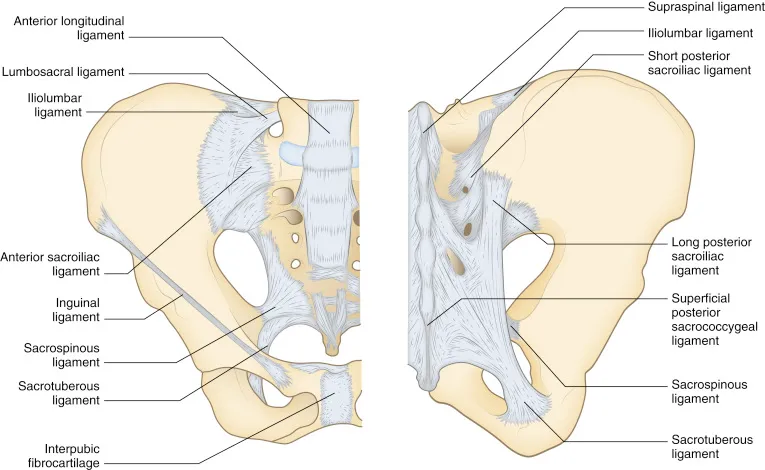
- Pelvic Ring: Composed of two innominate bones and the sacrum. Stability depends on the posterior ligamentous complex.
- Key Ligaments: Sacrospinous, sacrotuberous, and the critical posterior sacroiliac (SI) ligaments.
- Young-Burgess Classification (by mechanism):
- Anteroposterior Compression (APC): "Open book" injury.
- Lateral Compression (LC): Most common type.
- Vertical Shear (VS): High-energy, unstable; disrupts pelvic floor.
⭐ The posterior SI ligament complex is the primary stabilizer of the pelvis; its disruption signifies major instability.
Initial Assessment & Resuscitation - Code Red Protocol
- Primary Survey (ATLS): Focus on C (Circulation). Suspect pelvic fracture in any high-energy trauma, especially with hypotension.
- Hemodynamic Instability: SBP < 90 mmHg or HR > 120 bpm despite initial fluid bolus.
- Immediate Actions:
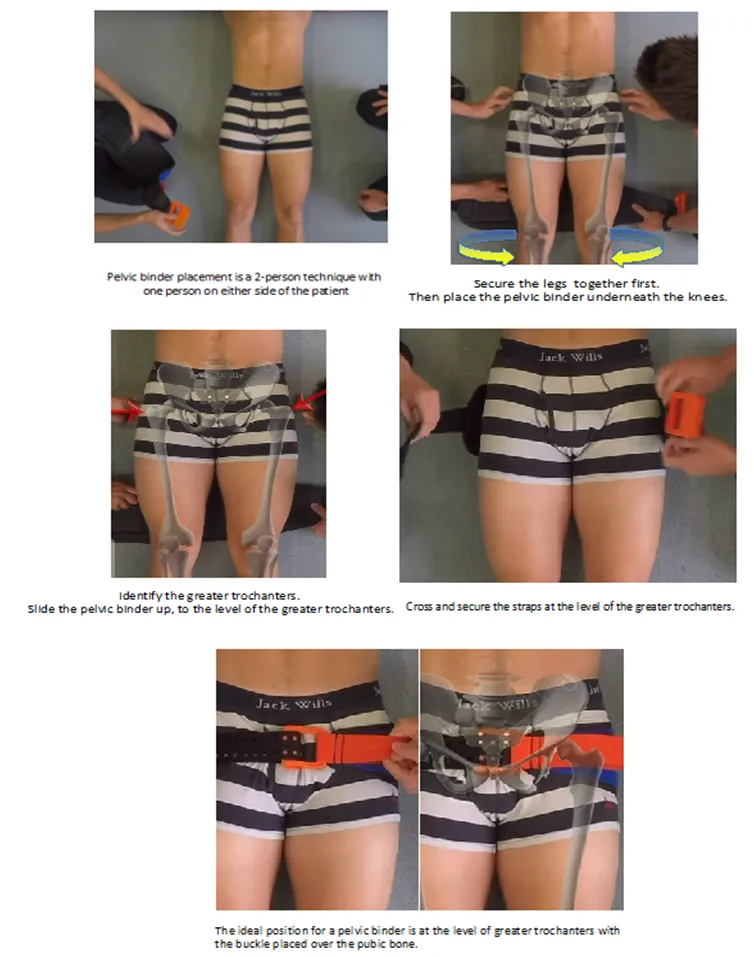
- Apply pelvic binder at the level of greater trochanters.
- Activate Massive Transfusion Protocol (MTP) / Code Red.
⭐ Early administration of Tranexamic Acid (TXA) within 3 hours of injury significantly reduces mortality from bleeding in trauma patients. Administer a 1g load over 10 min, then 1g infusion over 8 hours.
Hemorrhage Control - Plugging the Dam
- Source of Bleeding: Primarily from the posterior venous plexus (85%) and raw bone surfaces, not major arteries.
- Immediate Management:
- Apply a pelvic binder or sheet at the level of the greater trochanters.
- This reduces pelvic volume, stabilizes fracture, and promotes tamponade.
- Initiate massive transfusion protocol for persistent hypotension.
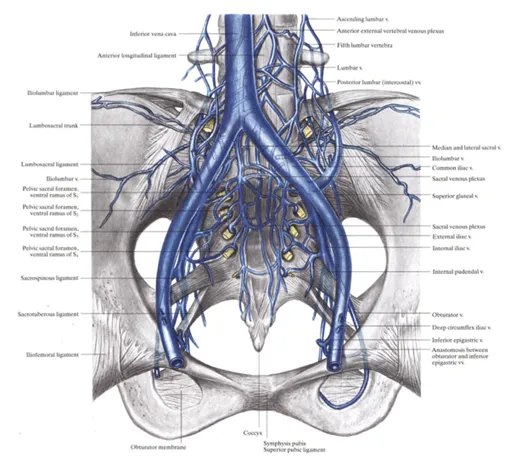
⭐ Most bleeding is venous. However, persistent hemodynamic instability despite binder application and fluid resuscitation strongly suggests an arterial injury requiring intervention.
Definitive Management & Complications - The Aftermath
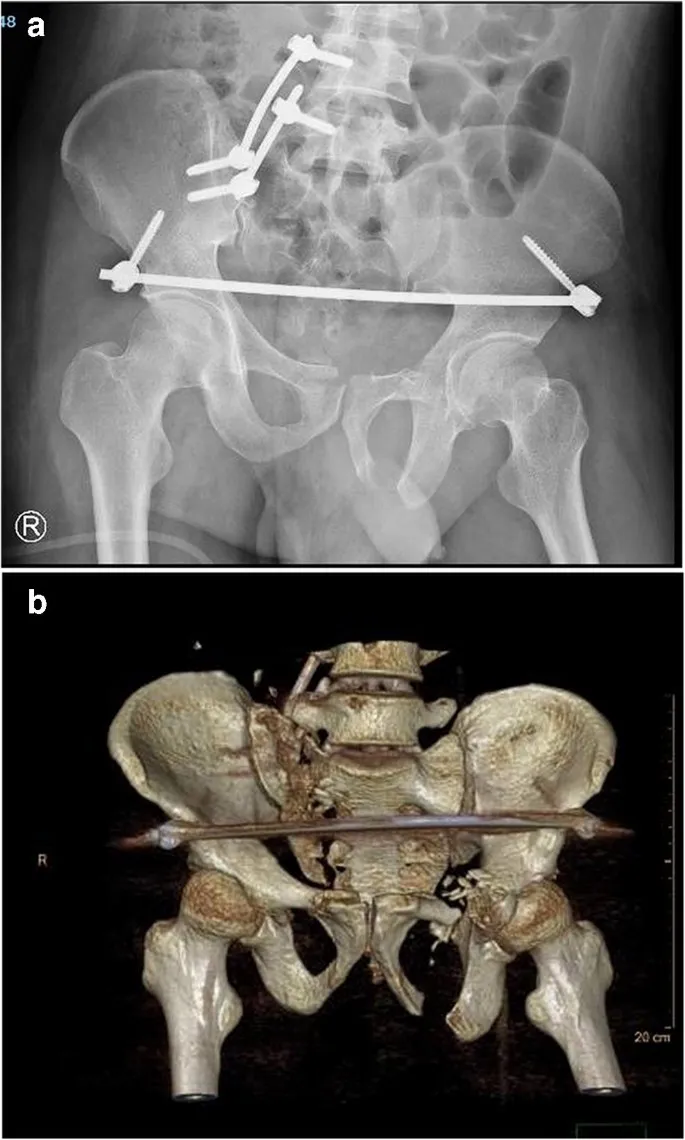
- Surgical Fixation (ORIF):
- Indicated for unstable fractures after the patient is hemodynamically stable.
- Goal: Restore pelvic ring integrity, enabling early mobilization.
- Major Complications:
- Neurologic Injury: Damage to the lumbosacral plexus (L5/S1 nerve roots common), potentially causing foot drop.
- Urogenital Injury: Urethral tears and bladder rupture are frequent. Suspect with blood at the meatus.
- Thromboembolism: High risk for DVT/PE; requires chemical and/or mechanical prophylaxis.
- Long-term: Chronic pain, gait disturbance, sexual dysfunction.
⭐ Injury to the lumbosacral plexus is a classic complication, especially with posterior pelvic ring disruptions. Always perform a thorough neurovascular exam of the lower extremities.
High‑Yield Points - ⚡ Biggest Takeaways
- Pelvic fractures from high-energy trauma can cause life-threatening hemorrhage, a key ATLS priority.
- Initial management: apply a pelvic binder to stabilize the pelvis and control common venous bleeding.
- For unstable patients with ongoing bleeding, angiography with embolization is critical for arterial hemorrhage.
- CT imaging is the gold standard for stable patients to define fracture anatomy.
- Always suspect associated urogenital injuries, like posterior urethral disruption in males.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

