Initial Assessment - First Look & Fix
- Exsanguinating Hemorrhage: Control immediately with direct pressure or tourniquet.
- Vascular Exam: Assess for hard & soft signs of vascular injury.
- Hard Signs: Pulsatile bleeding, expanding hematoma, audible bruit, palpable thrill, absent distal pulses.
- Soft Signs: History of hemorrhage, diminished pulses, adjacent nerve injury.
- 📌 6 P's of Ischemia: Pain, Pallor, Pulselessness, Paresthesia, Paralysis, Poikilothermia.
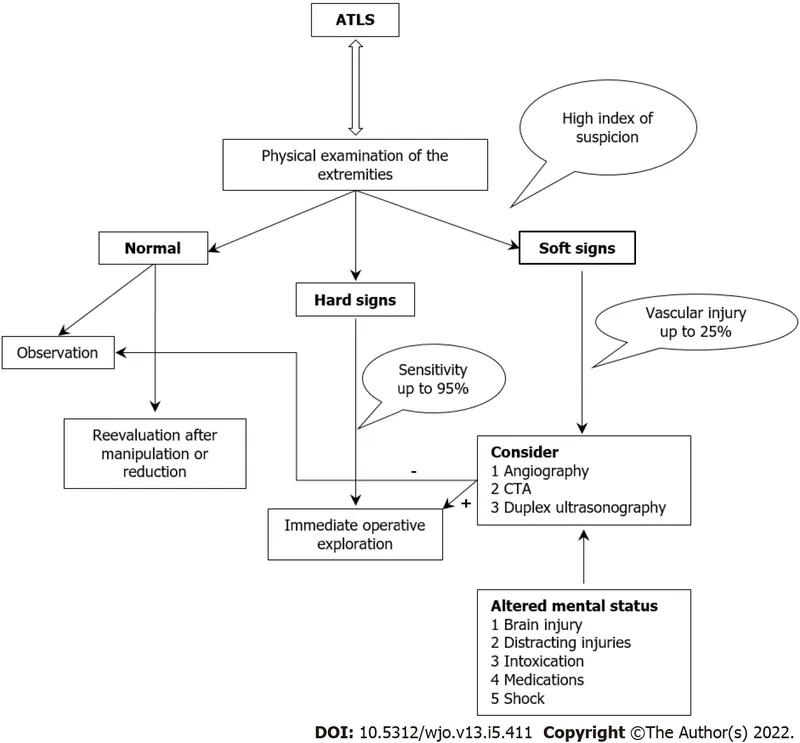
⭐ A normal pulse exam does not rule out a clinically significant vascular injury. Up to 20% of patients with arterial injuries can have palpable distal pulses.
Vascular Injuries - Red Flags & Reroutes
- Hard Signs (Red Flags) → Straight to OR
- Pulsatile bleeding, expanding hematoma
- Audible bruit, palpable thrill
- Signs of distal ischemia (6 P's)
- Absent distal pulses
- Soft Signs → Further Investigation
- History of major bleeding
- Diminished pulses
- Associated nerve deficit
- Significant bony injury (e.g., knee dislocation)
⭐ Following a knee dislocation, a normal distal pulse does NOT rule out a popliteal artery injury. Perform an Ankle-Brachial Index (ABI); if < 0.9, a CTA is mandatory due to high risk of intimal tear and delayed thrombosis.
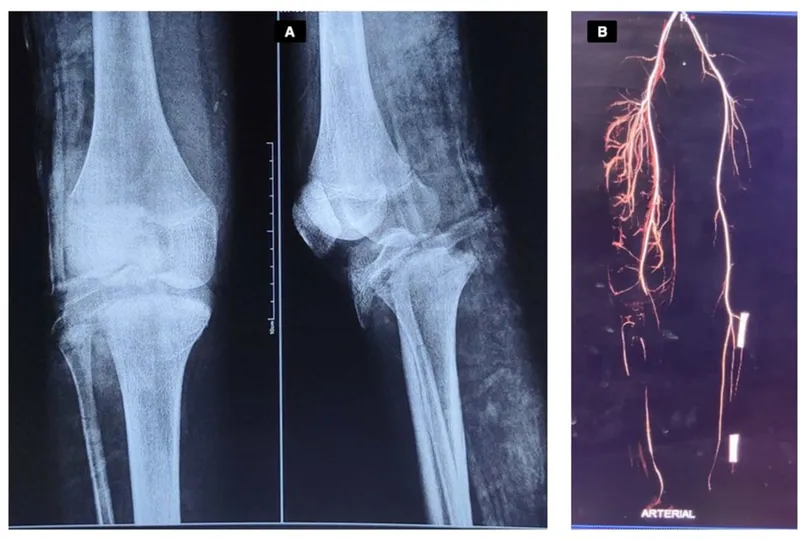
Fractures & Dislocations - Snaps, Cracks & Pops
- General: Open (skin breach) vs. Closed. Simple (2 fragments) vs. Comminuted (>2 fragments).
- Specific Injuries:
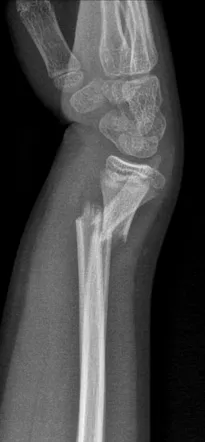
- Colles' Fx: Distal radius, dorsal displacement ("dinner fork"). Common with FOOSH.
- Scaphoid Fx: Anatomical snuffbox tenderness. High risk of avascular necrosis (AVN).
- Hip Fx: Leg shortened & externally rotated. High mortality in elderly.
- Shoulder Dislocation: Anterior is most common; risk of axillary nerve injury.
- Complications:
- Compartment Syndrome: ⚠️ Pain out of proportion. 📌 6 P's: Pain, Paresthesia, Pallor, Pulselessness, Poikilothermia, Paralysis.
- Fat Embolism: From long bone fx. Triad: neurologic changes, respiratory distress, petechial rash.
⭐ Scaphoid fractures can be occult on initial X-ray. If snuffbox tenderness is present, immobilize in a thumb spica cast and repeat imaging in 1-2 weeks to prevent AVN.
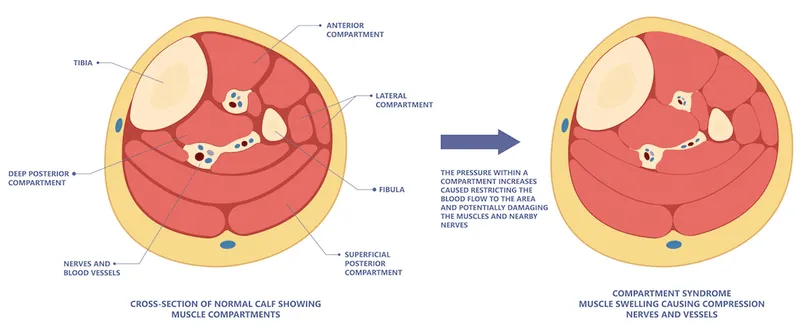
Compartment Syndrome - The Pressure Cooker
- Pathophysiology: Increased pressure within a closed fascial compartment, leading to compromised blood flow and tissue necrosis.
- Causes: Primarily long bone fractures (e.g., tibia, supracondylar), crush injuries, reperfusion swelling.
- Clinical Signs (The 6 P's): 📌 Pain out of proportion to injury, Paresthesias, Pallor, Paralysis, Pulselessness, and Poikilothermia (coldness).
- Diagnosis: Primarily clinical. Compartment pressure > 30-45 mmHg warrants fasciotomy. Consider if $P_{diastolic} - P_{compartment} < 20-30$ mmHg.
⭐ Pain on passive stretch of the affected muscles is the most sensitive early sign.
High‑Yield Points - ⚡ Biggest Takeaways
- Hard signs of vascular injury (e.g., pulsatile bleeding, expanding hematoma, bruit/thrill) mandate immediate surgical exploration.
- Soft signs (e.g., diminished pulses, non-expanding hematoma) warrant an Ankle-Brachial Index (ABI); if < 0.9, proceed to CTA.
- Compartment syndrome's earliest sign is pain out of proportion; pulselessness is a late finding. Treatment is emergent fasciotomy.
- Knee dislocations carry a high risk of popliteal artery injury.
- Suspect fat embolism syndrome (petechial rash, hypoxemia, neurologic changes) after long bone fractures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

