Primary Survey - First Things First
Follows the ABCDE algorithm to identify and manage immediate life-threats.
- Airway: Secure airway, maintain C-spine. Intubate if GCS ≤ 8.
- Breathing: Treat life-threats:
- Tension Pneumothorax: Needle decompression → chest tube.
- Open Pneumothorax: 3-sided dressing.
- Massive Hemothorax: Chest tube (>1500 mL initial).
- Circulation: Control hemorrhage, 2 large-bore IVs. Suspect tamponade (Beck's triad) → FAST scan.
⭐ In tension pneumothorax, clinical diagnosis trumps radiographic confirmation. Do not delay life-saving needle decompression for a chest X-ray.
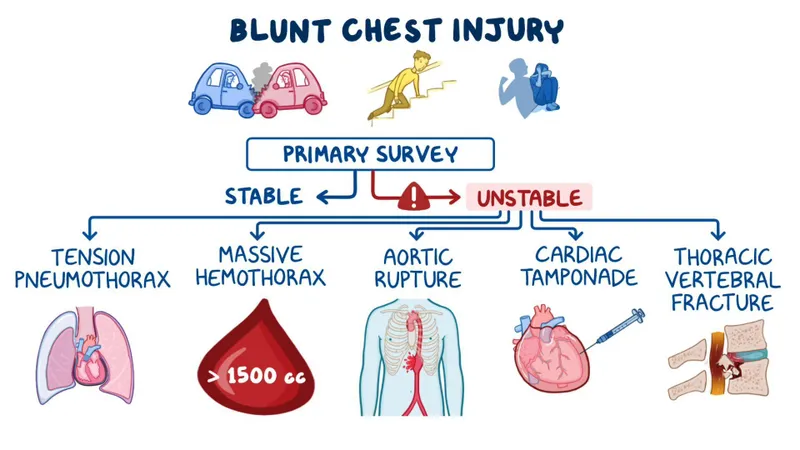
Immediate Threats - Thoracic Terrors
- Airway Obstruction: Stridor, gurgling, hoarseness. Secure airway immediately.
- Tension Pneumothorax: Hypotension, JVD, absent breath sounds, tracheal deviation. Immediate needle decompression (2nd ICS MCL or 5th ICS AAL) followed by chest tube.
- Open Pneumothorax: Sucking chest wound. Place a three-sided occlusive dressing.
- Massive Hemothorax: >1500 mL blood on initial chest tube placement. Requires thoracotomy.
- Cardiac Tamponade: Beck's Triad (hypotension, JVD, muffled heart sounds). Pericardiocentesis.
- Flail Chest: Paradoxical chest wall movement. Requires intubation and positive pressure ventilation.
⭐ Beck's triad for cardiac tamponade is only present in a minority of cases; a high index of suspicion and FAST exam are critical.
Pleural Space Problems - Air & Blood Blues
- Tension Pneumothorax: Clinical Dx! Hypotension, JVD, absent breath sounds, tracheal deviation.
- Immediate needle decompression (2nd ICS, MCL) → chest tube.
- Open Pneumothorax (“sucking chest wound”): Three-sided occlusive dressing.
- Hemothorax: Blood in pleural space; dullness to percussion.
- Tube thoracostomy (chest tube) is standard.
- Thoracotomy indicated for massive hemothorax: >1500 mL initial output, or >200 mL/hr for 2-4 hours.
⭐ In a tension pneumothorax, do not wait for a chest X-ray to confirm. Treat clinically with immediate needle decompression.
Pump & Pipe Injuries - Cardiac Catastrophes
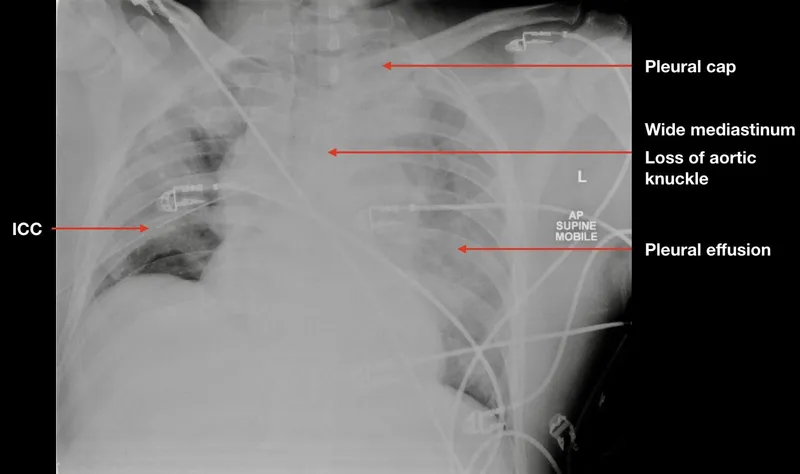
- Aortic Injury: Deceleration injury classic. Look for widened mediastinum (>8cm) on CXR, left hemothorax. Gold standard: CT Angio. Manage BP & HR (Labetalol) before surgical/endovascular repair.
- Myocardial Contusion: Blunt trauma mimics MI. ECG changes, ↑Troponins. Monitor for arrhythmias, manage supportively. Echocardiogram assesses wall motion abnormalities & valvular function.
- Cardiac Tamponade: 📌 Beck's Triad: ↓BP, ↑JVP, muffled heart sounds.
⭐ The most common site of traumatic aortic rupture is the aortic isthmus, just distal to the left subclavian artery.
Diagnostics & Interventions - See, Stick, Solve
- See (Diagnose): Rapidly assess with eFAST and portable CXR. Reserve CT for stable patients requiring detailed anatomical views.
- Stick (Intervene):
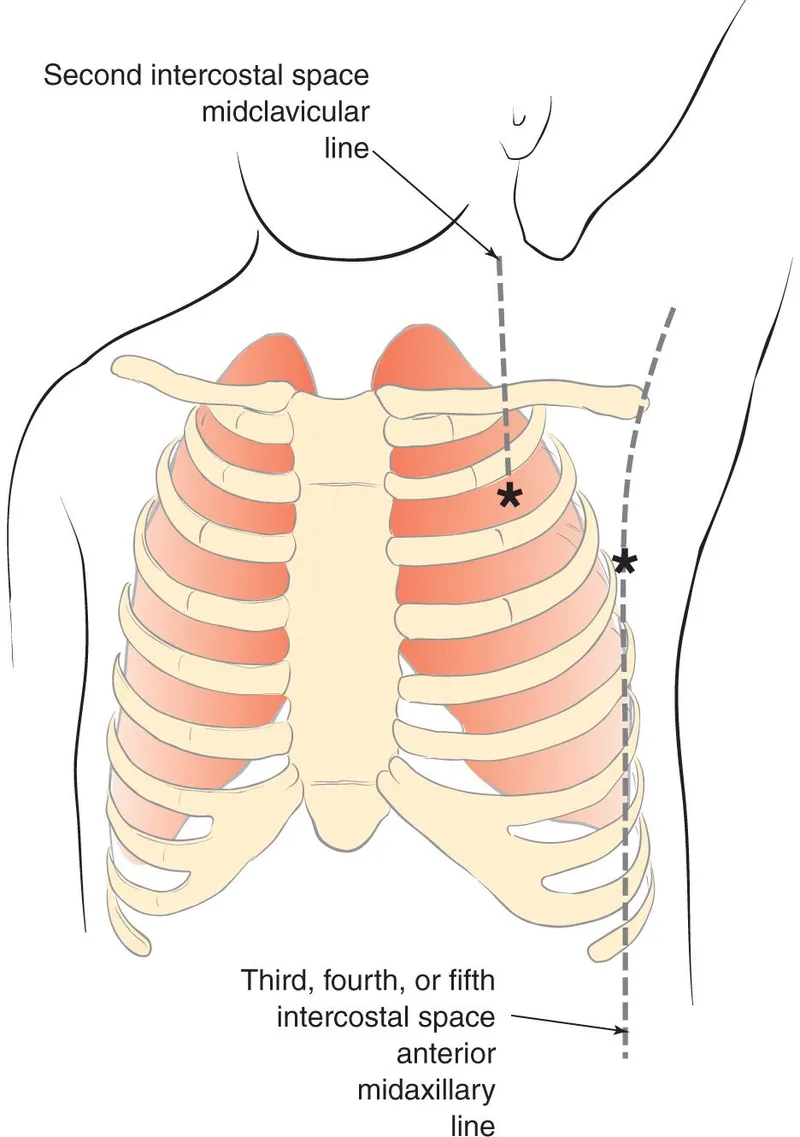
- Needle Decompression: 2nd ICS, mid-clavicular line.
- Tube Thoracostomy: 4th/5th ICS, anterior-axillary line.
- Emergency Thoracotomy: Penetrating trauma, recent signs of life.
⭐ A massive hemothorax is defined by an initial chest tube output of >1500 mL or persistent bleeding of >200 mL/hr for 2-4 hours, often requiring thoracotomy.
High‑Yield Points - ⚡ Biggest Takeaways
- Always start with ABC (Airway, Breathing, Circulation).
- Tension pneumothorax: Perform immediate needle decompression based on clinical signs, before a chest X-ray, followed by a chest tube.
- Open pneumothorax (sucking chest wound) requires a three-sided occlusive dressing.
- Massive hemothorax (>1.5L initial chest tube output) is an indication for urgent thoracotomy.
- Flail chest management focuses on pain control and positive pressure ventilation.
- Cardiac tamponade: Diagnose with FAST scan; treat with pericardiocentesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

