Indications & Contraindications - Gutsy Decisions
-
Primary Indication: Irreversible Intestinal Failure (IF) with life-threatening complications from Total Parenteral Nutrition (TPN).
-
Common Causes of IF Leading to Transplant:
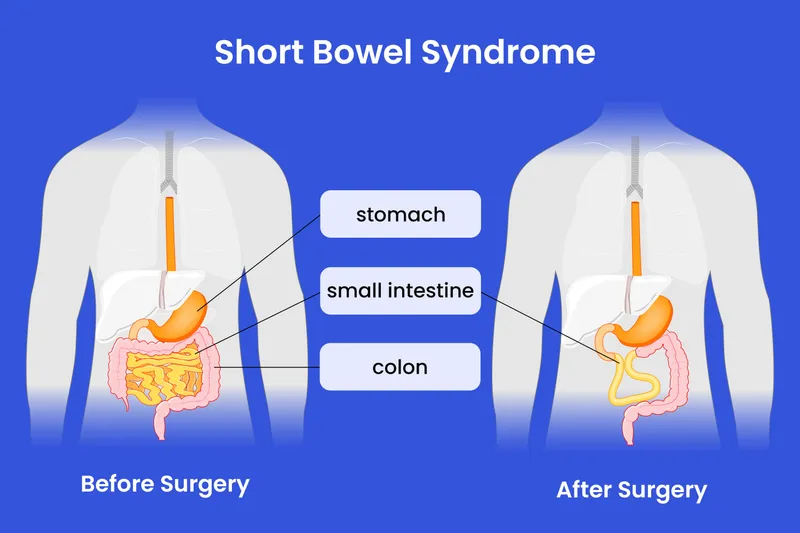
- Short Gut Syndrome (<100-150 cm small bowel): Most frequent cause, post-surgical resection (volvulus, necrotizing enterocolitis, trauma).
- Intestinal Motility Disorders: e.g., Chronic Intestinal Pseudo-obstruction (CIPO).
- Congenital Enteropathies: e.g., Microvillus inclusion disease.
-
Key TPN Complications Forcing Transplant:
- TPN-Associated Liver Disease (PNALD) with progressive fibrosis/cirrhosis.
- Recurrent, severe central line-associated bloodstream infections (CLABSI).
- Thrombosis of ≥2 major central veins.
-
Absolute Contraindications:
- Active malignancy or untreated infection.
- Severe cardiac or pulmonary disease.
- Active substance abuse or profound non-adherence.
⭐ High-Yield: The development of progressive liver failure (PNALD) is often the critical turning point that pushes a patient with intestinal failure towards transplantation evaluation.
Transplant Types - The Surgical Options

-
Isolated Small Bowel Transplant (ISBTx)
- Indication: Intestinal failure (IF) with preserved liver function.
- The most common type of small bowel transplant.
-
Combined Liver-Small Bowel Transplant (CLSBx)
- Indication: IF with irreversible intestinal failure-associated liver disease (IFALD).
- The native liver is removed.
-
Multivisceral Transplant (MVT)
- Indication: Diffuse splanchnic venous thrombosis, locally invasive abdominal tumors (e.g., desmoid), or extensive GI dysmotility.
- Involves stomach, pancreas, duodenum, and small intestine ± liver/colon.
⭐ The transplanted liver in a CLSBx confers an immunological advantage, leading to lower rates of acute rejection of the intestinal graft compared to ISBTx.
Post-Op Management - Rejection & Ruckus
- Rejection: Highest rate of all solid organ transplants due to high immunogenicity of gut-associated lymphoid tissue (GALT).
- Acute Cellular Rejection (ACR): Most common, peaks in first 3 months.
- Signs: ↑ stoma output, fever, abdominal pain, malabsorption.
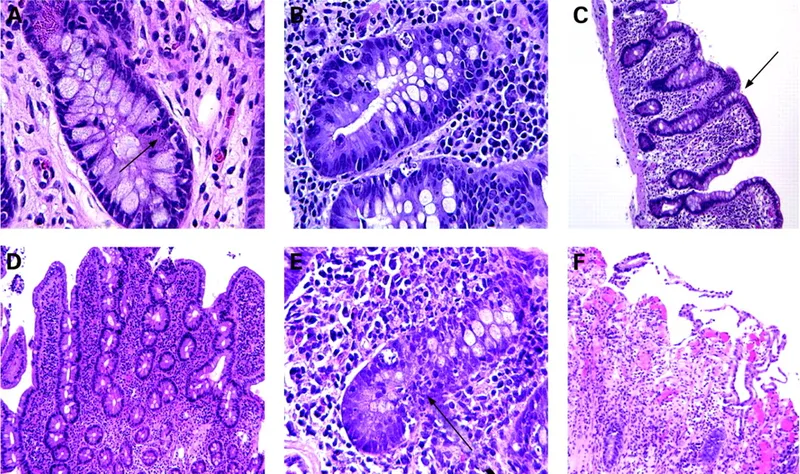
- Dx: Endoscopy with biopsy (gold standard) showing crypt apoptosis & villous blunting.
- Acute Cellular Rejection (ACR): Most common, peaks in first 3 months.
⭐ High stoma output is often the earliest and most reliable clinical sign of acute small bowel rejection.
-
Graft-vs-Host Disease (GVHD): Donor T-cells in the graft attack recipient tissues.
- Classic Triad: Erythematous maculopapular rash, secretory diarrhea, pancytopenia.
- High mortality; may require graft enterectomy.
-
Infections & Complications:
- CMV: Universal prophylaxis (ganciclovir/valganciclovir) and routine PCR monitoring are critical.
- Post-transplant lymphoproliferative disorder (PTLD): EBV-driven; presents with fever, lymphadenopathy.
-
ACR Management Flow:
High‑Yield Points - ⚡ Biggest Takeaways
- Primary indication is intestinal failure with parenteral nutrition (PN) complications, most notably irreversible liver disease.
- Graft types include isolated small bowel, combined liver-small bowel, or multivisceral, tailored to the extent of organ failure.
- The gut is highly immunogenic, necessitating potent immunosuppression (e.g., tacrolimus).
- Acute cellular rejection is the leading cause of graft loss, diagnosed via endoscopy with biopsy.
- High risk for CMV infection and EBV-associated PTLD.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

