Rejection Types - Immune System Overdrive
📌 Mnemonic: HACk the graft! (Hyperacute, Acute, Chronic)
| Type | Onset | Pathophysiology (HSR Type) | Key Histology/Features |
|---|---|---|---|
| Hyperacute | Minutes-Hours | Pre-formed anti-donor Abs (Type II) | Widespread thrombosis, vessel occlusion, ischemia. Irreversible. |
| Acute | < 6 months | T-cell mediated cellular infiltrate (Type IV) | Interstitial lymphocytic infiltrate, tubulitis. Usually reversible. |
| Chronic | > 6 months | Mixed T-cell/Ab-mediated (Type III/IV) | Irreversible fibrosis, atrophy. Graft arteriosclerosis, vanishing bile ducts. |
⭐ Acute rejection is the most common type, typically occurring within the first 6 months. It's often reversible with bolstered immunosuppression.
Diagnosis - Spotting the Attack
- Clinical Clues: Fever, malaise, and tenderness over the graft site.
- Organ-Specific Signs:
- Kidney: ↑ Serum Creatinine (>25% from baseline), ↓ urine output.
- Liver: ↑ LFTs (ALT, AST, GGT), ↑ bilirubin.
- Heart: Symptoms of heart failure (e.g., dyspnea, edema).
- Non-Invasive Tests:
- Donor-derived cell-free DNA (dd-cfDNA) levels may rise, indicating graft injury.
- Ultrasound to rule out vascular or surgical complications.
- Gold Standard:
- Allograft biopsy is definitive for diagnosis and grading rejection.
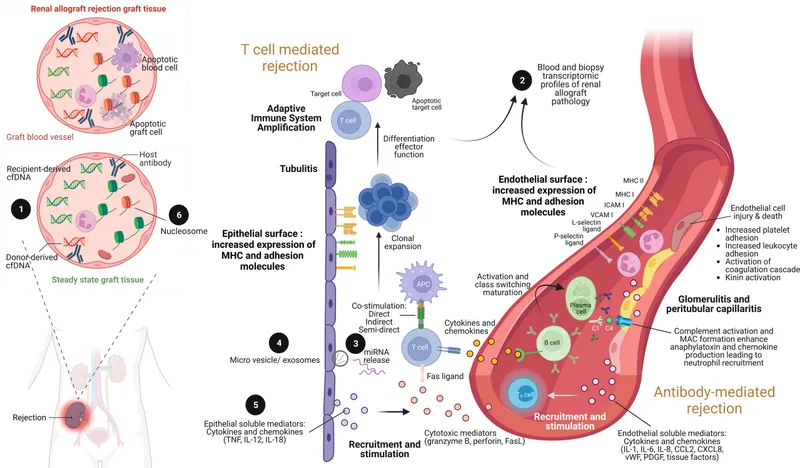
⭐ C4d deposition in peritubular capillaries on biopsy is a hallmark of antibody-mediated rejection, indicating complement activation.
Management - Calming the Storm
-
General Principle: Increase net immunosuppression. Biopsy is key to guide therapy.
-
Acute Cellular Rejection (ACR):
- 1st Line: High-dose pulse IV corticosteroids (e.g., methylprednisolone).
- Steroid-Refractory: Lymphocyte-depleting agents (e.g., anti-thymocyte globulin [ATG]) or other monoclonal antibodies (Alemtuzumab).
-
Antibody-Mediated Rejection (AMR):
- Goal: Remove circulating donor-specific antibodies (DSAs) & suppress B-cells.
- Multi-modal approach:
- Plasmapheresis (PP) or Immunoadsorption (IA) to remove antibodies.
- IV Immunoglobulin (IVIG) to neutralize antibodies.
- Targeted therapy: Rituximab (anti-CD20), Bortezomib (proteasome inhibitor).
-
Chronic Rejection / Chronic Allograft Vasculopathy (CAV):
- Largely irreversible; management is supportive.
- Optimize immunosuppression, manage risk factors (HTN, HLD).
- Eventual re-transplantation is the only definitive treatment.
⭐ The first-line therapy for acute T-cell mediated rejection is a high-dose pulse of corticosteroids. Most rejection episodes are steroid-responsive.
High‑Yield Points - ⚡ Biggest Takeaways
- Hyperacute rejection is immediate due to pre-formed recipient antibodies; causes graft thrombosis.
- Acute rejection occurs weeks to months later, is T-cell mediated, and usually reversible with immunosuppressants.
- Chronic rejection develops over months to years, causing irreversible graft fibrosis and arteriosclerosis.
- Graft-versus-host disease (GVHD) occurs when donor T-cells attack host tissues, typically after bone marrow transplant.
- Biopsy is the gold standard for diagnosing rejection.
- Manage acute rejection with corticosteroids and calcineurin inhibitors.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

