Chronic Rejection - The Slow Burn
- Timeline: Occurs months to years post-transplant.
- Pathogenesis: A slow, progressive, and often irreversible graft dysfunction. It's a mixed T-cell and antibody-mediated process causing chronic inflammation, fibrosis, and eventual atrophy.
- Key Organ-Specific Manifestations:
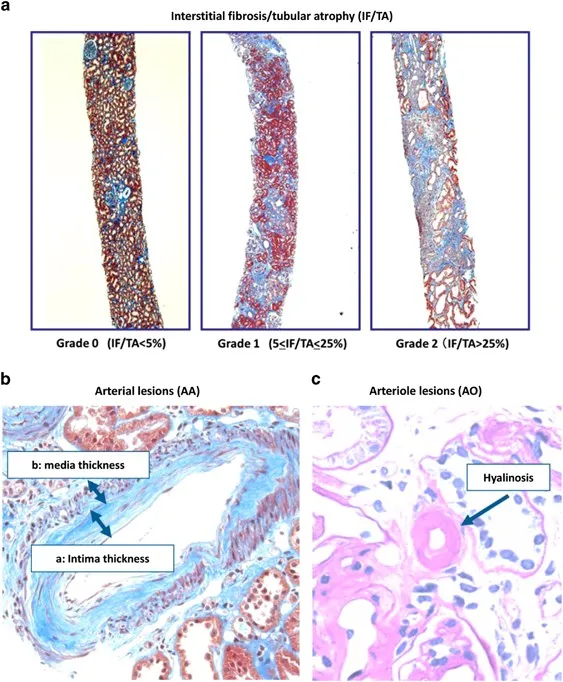
- Kidney: Interstitial fibrosis & tubular atrophy (IF/TA), graft glomerulopathy.
- Lung: Bronchiolitis obliterans (presenting with dry cough, dyspnea).
- Liver: Vanishing bile duct syndrome.
- Heart: Graft arteriosclerosis (accelerated coronary artery disease).
- Management: Generally refractory to immunosuppressive therapy; re-transplantation is often the only definitive treatment.
⭐ In lung transplants, chronic rejection manifests as Bronchiolitis Obliterans Syndrome (BOS), an obstructive process seen on PFTs.
Infections & Malignancy - Unwanted Guests
- Infections: Risk is stratified by time from transplant, reflecting the net state of immunosuppression. See timeline below.
- Malignancy: Chronic immunosuppression significantly increases risk.
- Skin Cancers: Most common malignancy. Squamous Cell Carcinoma (SCC) is much more frequent and aggressive than Basal Cell Carcinoma (BCC).
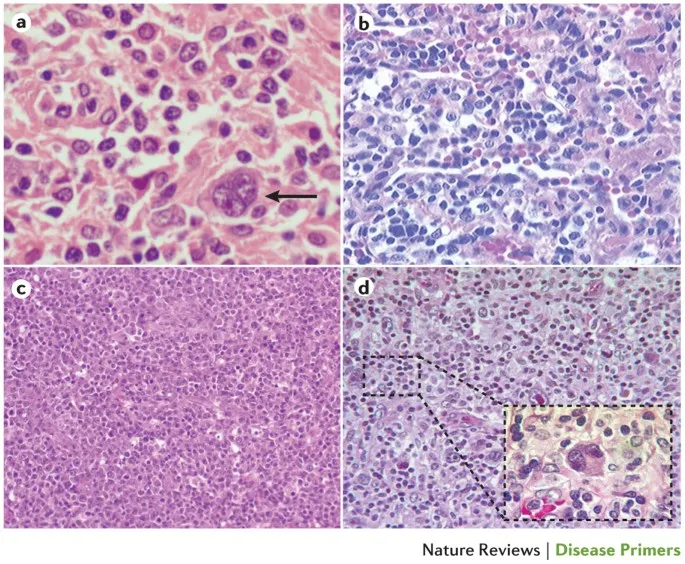
- PTLD (Post-Transplant Lymphoproliferative Disorder): Strongly associated with Epstein-Barr Virus (EBV). Presents as a spectrum from hyperplasia to lymphoma.
⭐ First-line therapy for PTLD is reducing immunosuppression. Rituximab is a subsequent option if this fails.
Cardiovascular & Metabolic - The Price of Pills
- Calcineurin Inhibitors (Tacrolimus, Cyclosporine)
- Hypertension (HTN): Common; due to renal vasoconstriction.
- Hyperglycemia: ↓ insulin secretion (Tacrolimus > Cyclosporine).
- Hyperlipidemia: ↑ LDL & triglycerides (Cyclosporine > Tacrolimus).
- Corticosteroids (Prednisone)
- Hyperglycemia/Diabetes: Due to insulin resistance.
- Dyslipidemia & Weight Gain: Central obesity, Cushingoid features.
- Hypertension: Mineralocorticoid effects.
- mTOR Inhibitors (Sirolimus, Everolimus)
- Profound Hypertriglyceridemia & hypercholesterolemia.
- ⚠️ Can impair wound healing; use with caution early post-transplant.
⭐ Sirolimus is particularly notorious for causing severe hypertriglyceridemia, often requiring lipid-lowering therapy.
Renal & Other Effects - Collateral Damage
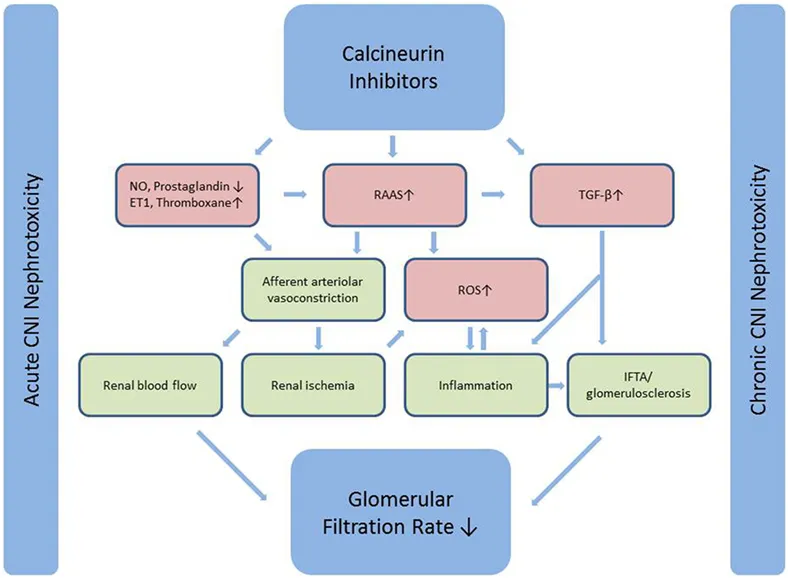
- CNI Nephrotoxicity:
- Acute: Reversible afferent arteriole vasoconstriction.
- Chronic: Irreversible; leads to hyaline arteriolosclerosis, tubular atrophy, interstitial fibrosis → chronic graft failure.
- Hypertension:
- Multifactorial: CNI-induced vasoconstriction, steroid-induced fluid retention, pre-existing disease.
- Metabolic Syndrome:
- Hyperlipidemia: mTOR inhibitors (sirolimus), CNIs, steroids.
- New-Onset Diabetes (NODAT): Tacrolimus & steroids are major culprits.
- Hyperuricemia & Gout:
- CNIs (esp. Cyclosporine) ↓ renal urate excretion.
- Bone Disease:
- Steroid-induced osteoporosis & avascular necrosis.
⭐ CNI-induced afferent arteriole vasoconstriction is a primary driver of both acute and chronic nephrotoxicity, leading to long-term graft loss.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronic rejection is the leading cause of long-term allograft failure, characterized by fibrosis and vascular obliteration.
- Immunosuppression increases risk for opportunistic infections (CMV, PJP) and malignancies, especially skin cancer and PTLD.
- Cardiovascular disease is a major cause of mortality in transplant recipients.
- Calcineurin inhibitor nephrotoxicity (cyclosporine, tacrolimus) is a common cause of renal dysfunction.
- Monitor for metabolic complications like new-onset diabetes, hypertension, and hyperlipidemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

