ASA Classification - Status Check
- ASA 1: Normal healthy patient.
- ASA 2: Mild systemic disease (e.g., controlled HTN or DM, smoking, obesity). No functional limitations.
- ASA 3: Severe systemic disease with functional limitations (e.g., stable angina, ESRD on dialysis, post-MI >3 months).
- ASA 4: Severe systemic disease that is a constant threat to life (e.g., recent MI <3 months, sepsis, ARDS).
- ASA 5: Moribund; not expected to survive without the operation.
- ASA 6: Declared brain-dead; organ procurement.
- Modifier E: Added for emergency surgery (e.g., ASA 2E).
⭐ The ASA classification is an independent predictor of perioperative morbidity and mortality. Each increasing class doubles the risk of adverse outcomes.
Airway Assessment - Open Sesame
Predicting a difficult airway is key to preventing a "can't intubate, can't ventilate" crisis.
📌 LEMON Method:
- Look: External signs (e.g., small jaw, large tongue, facial trauma).
- Evaluate: 3-3-2 Rule
- Mouth Opening: > 3 fingers
- Thyromental Distance: > 3 fingers
- Hyoid-to-Thyroid: > 2 fingers
- Mallampati Score: Assesses oral opening; higher class = more difficult.
- Obstruction: Any signs of upper airway obstruction?
- Neck Mobility: Limited C-spine movement is a red flag.
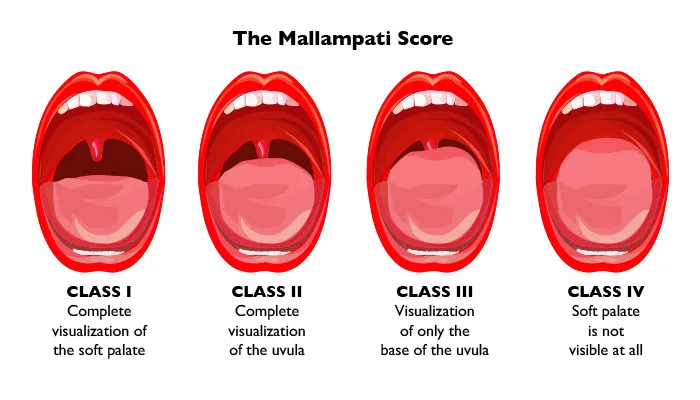
⭐ A Mallampati score of III or IV significantly increases the likelihood of a difficult intubation, as less of the pharyngeal structure is visible.
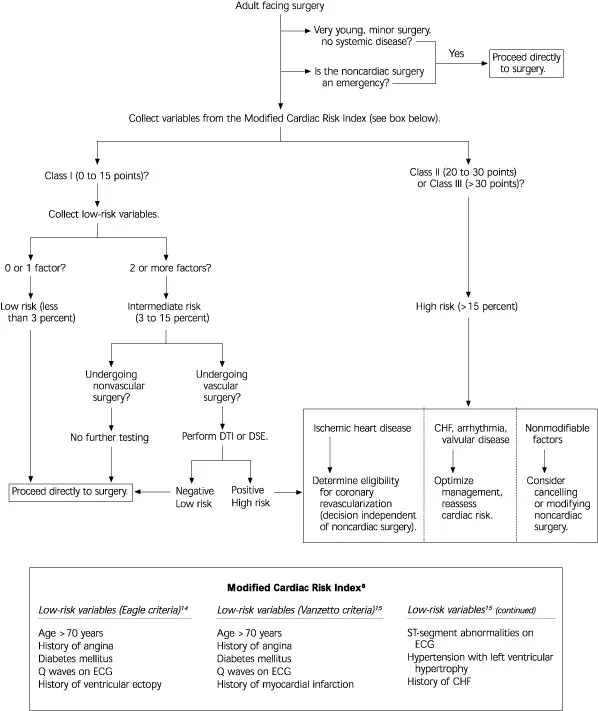
Cardiac Risk Stratification - Heart Smart
Assesses risk of Major Adverse Cardiac Events (MACE) in non-cardiac surgery using the Revised Cardiac Risk Index (RCRI). One point for each:
- High-Risk Surgery: intraperitoneal, intrathoracic, suprainguinal vascular
- Ischemic Heart Disease: hx of MI, + stress test, current angina, nitrates use
- Congestive Heart Failure: hx of CHF, pulmonary edema, PND
- Cerebrovascular Disease: hx of stroke or TIA
- Diabetes Mellitus: requiring pre-op insulin
- Chronic Kidney Disease: pre-op creatinine >2.0 mg/dL
⭐ Beta-blockers are recommended to be continued if the patient is already on them. Starting them perioperatively is not routinely recommended for beta-blocker naive patients unless there is a clear indication like untreated severe hypertension or symptomatic arrhythmia.
Perioperative Medication - Stop or Go?
General Principle: Continue most essential medications, especially those for cardiovascular stability. Stop those that increase surgical risk (bleeding, hypotension).
| Medication Class | Action | Timing / Notes |
|---|---|---|
| Antihypertensives | ||
| - Beta-blockers | Continue | Prevents rebound tachycardia/hypertension. |
| - ACEi / ARBs | Stop | Hold on the morning of surgery (risk of refractory hypotension). |
| Antiplatelets/Anticoagulants | ||
| - Aspirin / Clopidogrel | Stop | Hold 5-7 days prior, unless high cardiac risk. |
| - Warfarin | Stop | Hold 5 days prior; bridge if high thromboembolic risk. |
| - DOACs | Stop | Hold 2-3 days prior (depends on drug & renal function). |
| Diabetes Meds | ||
| - Oral agents | Stop | Hold morning of surgery (risk of hypoglycemia). |
| - Insulin | Adjust | Take half dose of long-acting insulin; hold short-acting. |
| Psychiatric Meds | Continue | Avoid withdrawal syndromes. |
High-Yield Points - ⚡ Biggest Takeaways
- The ASA classification is a cornerstone for predicting perioperative risk.
- The Mallampati score predicts the ease of intubation; higher classes mean more difficulty.
- Use the RCRI to assess cardiac risk; recent MI, decompensated HF, and severe valve disease are major risks.
- Advise smoking cessation at least 8 weeks pre-op to decrease pulmonary complications.
- Continue β-blockers perioperatively; hold most anticoagulants based on procedure-specific bleeding risk.
- Standard NPO guidelines: 2 hours for clear liquids, 6-8 hours for solids.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

