Post-Op Atelectasis - Lungs Gone Flat
- Pathophysiology: Alveolar collapse from airway obstruction (mucus plugs) and shallow breathing (pain, anesthesia), leading to ventilation/perfusion (V/Q) mismatch and hypoxemia.
- Timeline: Highest risk 24-48 hours after surgery.
- Signs: Fever, tachypnea, tachycardia, ↓ breath sounds, dullness to percussion, tracheal deviation towards the affected side.
- Prevention/Tx: Lung expansion is critical.
- 📌 Mnemonic: IS COPE → Incentive Spirometry, Coughing, Opioid minimization, Pain control, Early ambulation.
⭐ Atelectasis is the most common cause of fever on post-op days 1-2 ("Wind").

Aspiration & Pneumonitis - Wrong Pipe Woes
- Aspiration Pneumonitis (Chemical): Acute lung injury from inhaling sterile acidic gastric contents (pH < 2.5).
- Onset: Rapid, within 2-12 hours.
- Sx: Hypoxemia, non-productive cough, respiratory distress.
- Tx: Supportive care (O₂, ventilation). Antibiotics not initially indicated.
- Aspiration Pneumonia (Infectious): Lung infection from inhaling colonized oropharyngeal bacteria.
- Onset: Slower, 1-5 days.
- Sx: Fever, productive cough (may be putrid), consolidation.
- Tx: Antibiotics (e.g., Clindamycin).
⭐ Exam Favorite: Infiltrate location varies with patient position during aspiration. Supine: posterior segments of upper lobes or superior segments of lower lobes. Erect: basilar segments of lower lobes (esp. Right Lower Lobe).
Post-Op Pneumonia - Buggy Lung Blues
- Onset: Typically >48 hours after surgery.
- Pathophysiology: Impaired secretion clearance and aspiration lead to bacterial growth. Atelectasis is a major precursor.
- Common Organisms:
- S. pneumoniae, H. influenzae.
- Hospital-Acquired (HAP): Pseudomonas, MRSA, GNRs.
- Aspiration: Anaerobes (e.g., Bacteroides, Prevotella).
- Prevention & Rx:
- 📌 Prevention: Pain control, Positioning (head elevation), incentive sPirometry, early amPulation.
- Rx: Empiric broad-spectrum antibiotics, then tailor to cultures.
⭐ Aspiration pneumonia classically affects the right lower lobe (RLL) due to the more vertical angle of the right mainstem bronchus. Suspect anaerobes if foul-smelling sputum or abscess develops.

Pulmonary Embolism - Clot on the Move
- Pathophysiology: Obstruction of pulmonary artery, usually from deep vein thrombosis (DVT).
- Risk Factors: Virchow's Triad (stasis, hypercoagulability, endothelial injury) - recent surgery, malignancy, immobility.
- Presentation: Sudden-onset dyspnea, pleuritic chest pain, tachypnea, tachycardia. Massive PE can cause syncope, hypotension.
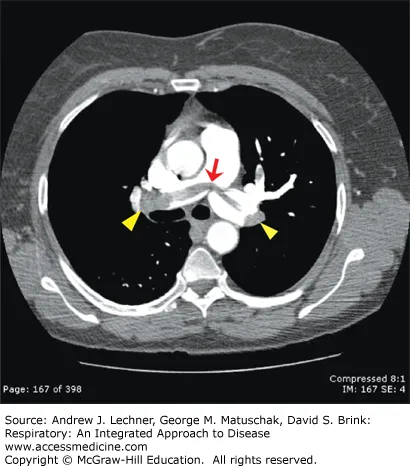
- Diagnosis: Best initial test is CT Angiogram (CTA). V/Q scan if CTA contraindicated.
⭐ ECG Finding: The classic S1Q3T3 pattern (deep S in lead I, Q wave and inverted T in lead III) is highly specific but rarely seen.
- Atelectasis is the most common cause of fever in the first 48 hours; prevent with incentive spirometry.
- Suspect pulmonary embolism (PE) with sudden-onset dyspnea and pleuritic chest pain.
- Postoperative pneumonia typically occurs 3-5 days later, with productive cough and fever.
- Aspiration pneumonitis causes acute hypoxemia after potential aspiration during anesthesia induction or emergence.
- Major risk factors include smoking, COPD, obesity, and anesthesia time >3 hours.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

