Drain Fundamentals - Meet the Tubes
- Purpose: Evacuate fluid (blood, pus, serum), obliterate dead space, and monitor for anastomotic leaks.
- Classification by Mechanism:
- Open (Passive): Rely on gravity/capillary action; higher infection risk.
- Examples: Penrose, corrugated rubber.
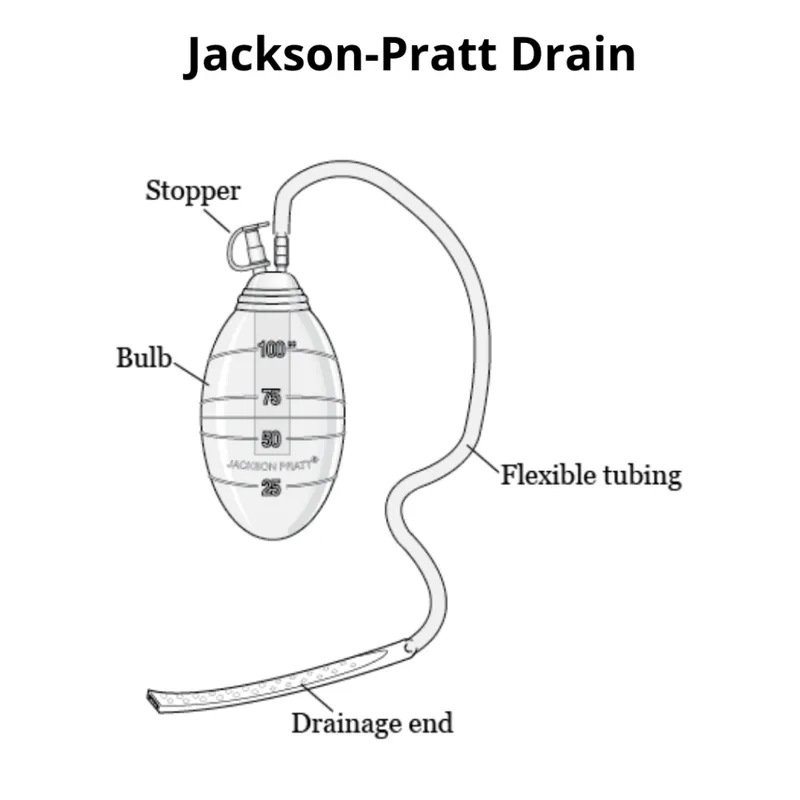
- Closed (Active): Use suction (negative pressure); lower infection risk.
- Examples: Jackson-Pratt (JP), Blake, Hemovac.
- Open (Passive): Rely on gravity/capillary action; higher infection risk.
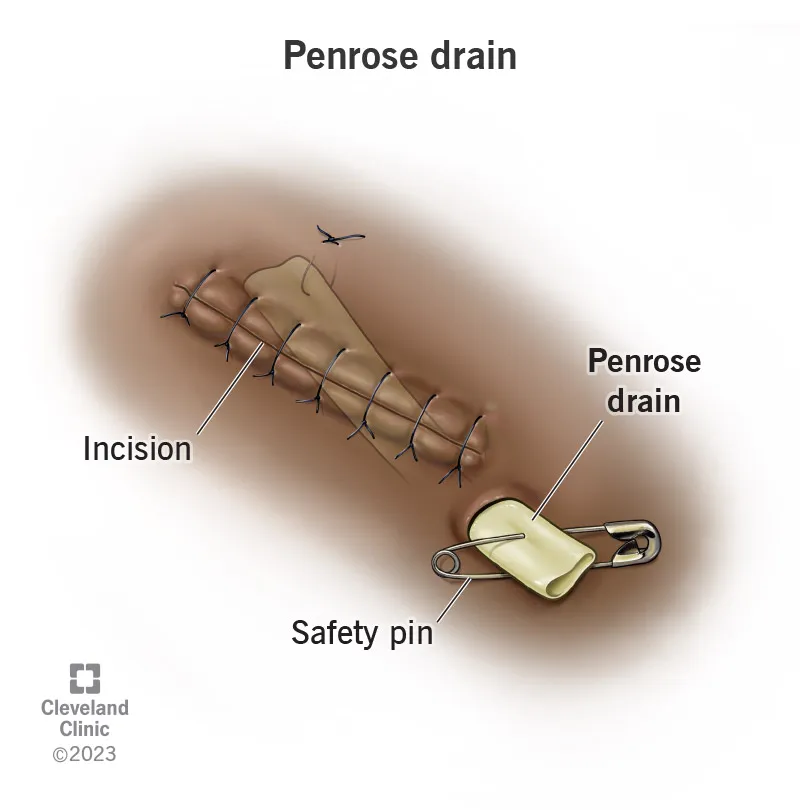
⭐ Drain output character is a vital sign for post-op complications. Milky/chylous fluid suggests thoracic duct injury, while cloudy/purulent fluid indicates infection.
Drain Indications - A Necessary Evil
-
Therapeutic: To evacuate established fluid collections.
- Abscess, hematoma, seroma
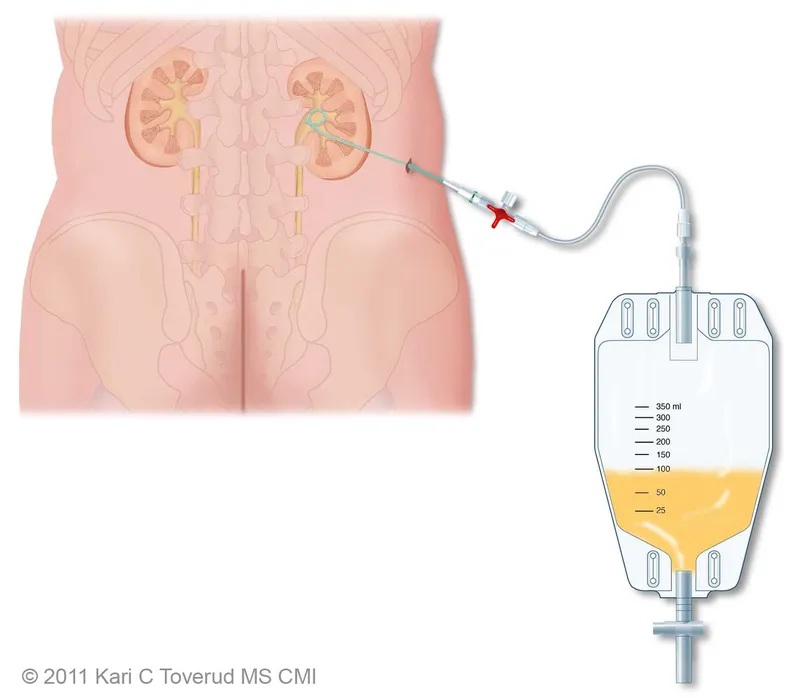
- Contaminated fluid (e.g., bile, enteric contents, urine)
-
Prophylactic: To prevent fluid accumulation & monitor for leaks.
- Obliterate dead space (e.g., mastectomy, axillary dissection).
- Provide early warning for anastomotic leakage (e.g., colorectal surgery).
- Reduce seroma/hematoma formation in high-risk procedures.
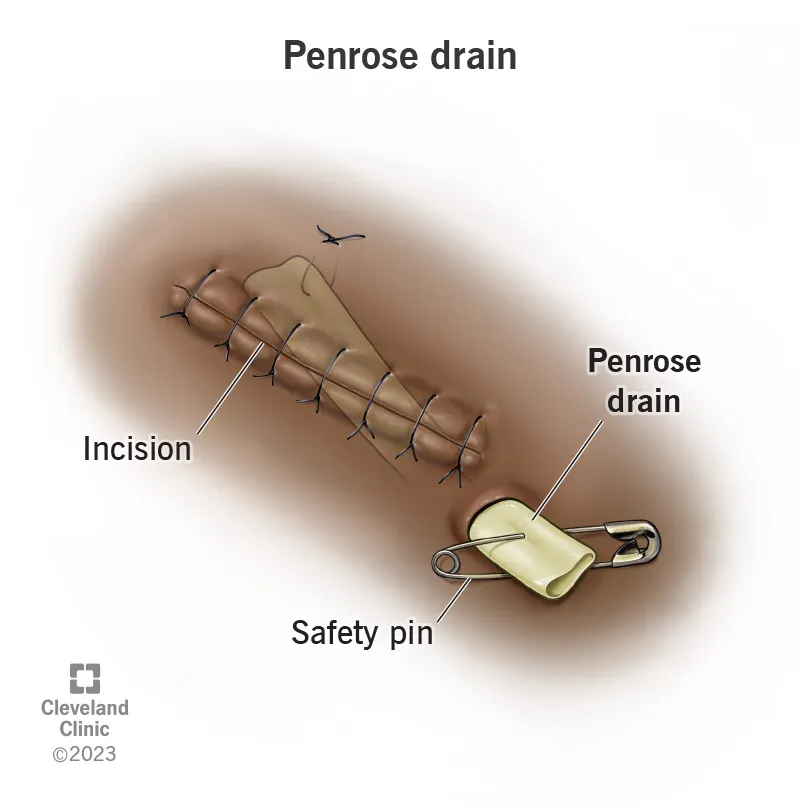
⭐ Drains are foreign bodies that can increase infection risk if left in too long. A common threshold for removal is when output is <25-30 mL/24h.
Drain Care - The Daily Grind
- Monitor Output: Daily, record volume, color (serous, serosanguinous, purulent), and character. Note any abrupt changes.
- Inspect Site: Check for erythema, induration, tenderness, or leakage around the insertion site. Follow local cleansing protocols.
- Maintain Patency: Gently milk or strip tubing only if clots or debris are visible, preventing obstruction.
- Manage Suction: Empty the collection bulb/reservoir, measure the output, and compress the reservoir to re-engage negative pressure.
⭐ A sudden ↓ in output from a high-volume drain often signals an obstruction (e.g., clot), not clinical resolution.
Complications - When Tubes Go Rogue
- Obstruction/Blockage:
- Sudden ↓ output with clinical signs of fluid collection (seroma, hematoma).
- Caused by fibrin clots or debris.
- Management: Gentle flushing with sterile saline.
- Infection:
- Site: Erythema, tenderness, purulent discharge.
- Systemic: Fever, leukocytosis, potential abscess.
- Dislodgement/Migration:
- Tube moves or is prematurely removed. Confirm position with imaging if suspected.
- Retained Fragment:
- Rare; drain breaks on removal. Requires imaging and surgical retrieval.
⭐ A sudden drop in drain output isn't always resolution. Suspect blockage if clinical signs of fluid collection persist; this prevents seroma/hematoma.
Drain Removal - The Grand Finale
-
Key Removal Criteria:
- Output: < 25-30 mL/day for 2 consecutive days.
- Fluid Quality: Serous (clear/yellow) not purulent or chylous.
- Clinical Picture: Patient afebrile, infection resolving, no ongoing leaks (air, bile, enteric).
-
Procedure Essentials:
- Aseptic technique is non-negotiable.
- Cut retaining suture.
- For thoracic drains, instruct patient to perform Valsalva maneuver during removal to prevent pneumothorax.
- Apply a sterile, occlusive dressing immediately.
⭐ A persistent air leak is an absolute contraindication for chest tube removal; premature removal risks tension pneumothorax.
High‑Yield Points - ⚡ Biggest Takeaways
- Drains prevent fluid collections (seromas, hematomas) to reduce infection risk and promote healing.
- Closed-suction drains (e.g., Jackson-Pratt) are preferred over open drains (e.g., Penrose) to minimize infection.
- Remove drains when output is <30 mL/day for two consecutive days.
- A sudden drop in output suggests a clot or blockage, not resolution.
- Analyze drain fluid to diagnose leaks (e.g., amylase for pancreatic, bilirubin for bile).
- Key complications include infection, pain, and erosion into adjacent structures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

