🫒 Pathophysiology - The Olive Pit Stop
- Progressive hypertrophy and hyperplasia of the pyloric muscularis propria (both circular and longitudinal layers).
- This narrows the pyloric channel, leading to a functional gastric outlet obstruction.
- Etiology is multifactorial, with a key association being neonatal macrolide exposure (e.g., erythromycin).
- 📌 Mnemonic: The pylorus becomes a muscular "pit stop" too thick for food to pass.
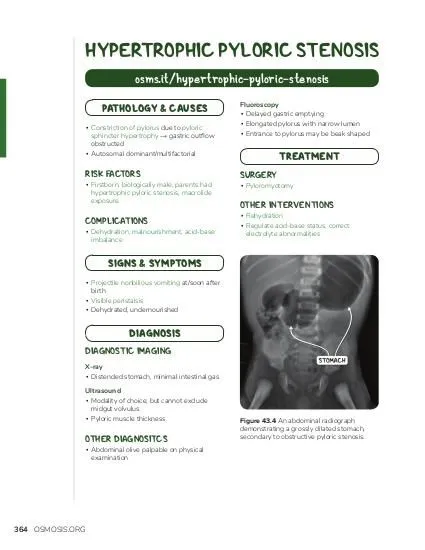
⭐ The thickened muscle creates the pathognomonic physical finding: a palpable, firm, mobile, ~2 cm "olive-shaped" mass in the epigastrium.
🤮 Clinical Manifestations - Projectile Problems
- Classic Onset: Healthy infant (often first-born male) at 2-8 weeks of age.
- Hallmark Vomiting:
- Projectile, non-bilious emesis, typically 30-60 min after feeding.
- Infant is a "hungry vomiter," eager to feed again immediately.
- Physical Exam Findings:
- Palpable, firm, mobile "olive-shaped" mass in the epigastrium/RUQ.
- Visible peristaltic waves moving left-to-right across the upper abdomen.
- Consequences:
- Dehydration (↓ skin turgor, sunken fontanelle).
- Failure to thrive or weight loss.
⭐ The classic metabolic disturbance is a hypokalemic, hypochloremic metabolic alkalosis. Paradoxical aciduria may occur as kidneys excrete H+ to conserve K+.
🫒 Diagnosis - Finding the Olive
- Physical Exam: A palpable, firm, mobile "olive-sized" mass in the RUQ/epigastrium is pathognomonic but often absent.
- Labs: Reveal hypokalemic, hypochloremic metabolic alkalosis from emesis of gastric $HCl$. Paradoxical aciduria may occur as kidneys conserve $K^+$ at the expense of $H^+$.
- Imaging:
- Abdominal Ultrasound (US): Test of choice.
- Pyloric muscle thickness > 4 mm
- Channel length > 16 mm
- Upper GI Series (if US non-diagnostic): Shows "string sign."
- Abdominal Ultrasound (US): Test of choice.
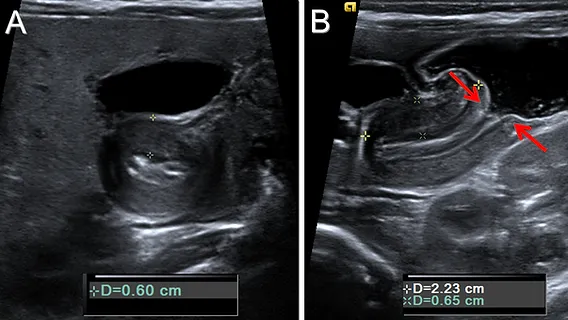
⭐ Pre-op management is key: Correct dehydration and electrolyte abnormalities with IV fluids before pyloromyotomy. Surgery is not an emergency.
🔪 Management - Pre-Op to Pyloromyotomy
-
Pre-operative Stabilization (CRUCIAL):
- Correct dehydration & hypochloremic, hypokalemic metabolic alkalosis ($↓Cl⁻, ↓K⁺, ↑HCO₃⁻$).
- IV fluids: Start with Normal Saline (NS) bolus.
- Maintenance: D5 1/2 NS + KCl (add K⁺ only after urination confirmed).
- Surgical clearance: Cl⁻ > 85 mEq/L, HCO₃⁻ < 30 mEq/L, adequate urine output.
-
Definitive Treatment: Pyloromyotomy
- Ramstedt pyloromyotomy: Longitudinal incision of the hypertrophied pyloric muscle, leaving mucosa intact.
- Can be done open or laparoscopically.
⭐ Pyloromyotomy is urgent, but NOT an emergency. Surgery is delayed until fluid and electrolyte abnormalities are corrected to reduce anesthetic risk.
⚠️ Complications - Post-Op Pitfalls
- Persistent Vomiting: Most common post-op issue.
- Causes: Incomplete pyloromyotomy, GERD, gastritis.
- Mucosal Perforation: Intra-op complication requiring immediate repair.
- Wound Infection/Dehiscence: Standard surgical site risks.
⭐ Persistent emesis for 24-48h post-op is common due to gastric atony. If vomiting continues >5 days, suspect incomplete myotomy.
⚡ Biggest Takeaways
- Classic triad: Non-bilious projectile vomiting, a palpable "olive-like" mass, and visible peristalsis in a 2-6 week old infant.
- Diagnosis: Abdominal ultrasound is the gold standard, showing a thickened (>4 mm) and elongated (>14 mm) pylorus.
- Lab hallmark: Hypokalemic, hypochloremic metabolic alkalosis with paradoxical aciduria due to volume contraction and RAAS activation.
- Pre-op management is critical: First, correct dehydration and electrolytes with IV fluids (NS, then D5 ½ NS + KCl).
- Definitive treatment: Ramstedt pyloromyotomy, an incision of the hypertrophied pyloric muscle.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

