💥 The Initial Hit
-
Primary Injury: Irreversible mechanical damage from trauma (e.g., fracture, dislocation). Causes immediate neuronal and glial cell death at the injury site.
-
Spinal Shock: A transient physiological shutdown of spinal cord function below the lesion.
- Features: Flaccid paralysis, areflexia (loss of deep tendon reflexes), and sensory loss.
- Duration: Lasts hours to weeks.
⭐ The end of spinal shock is heralded by the return of the bulbocavernosus reflex (BCR). The true extent of permanent injury (e.g., UMN signs) can be assessed after this point.
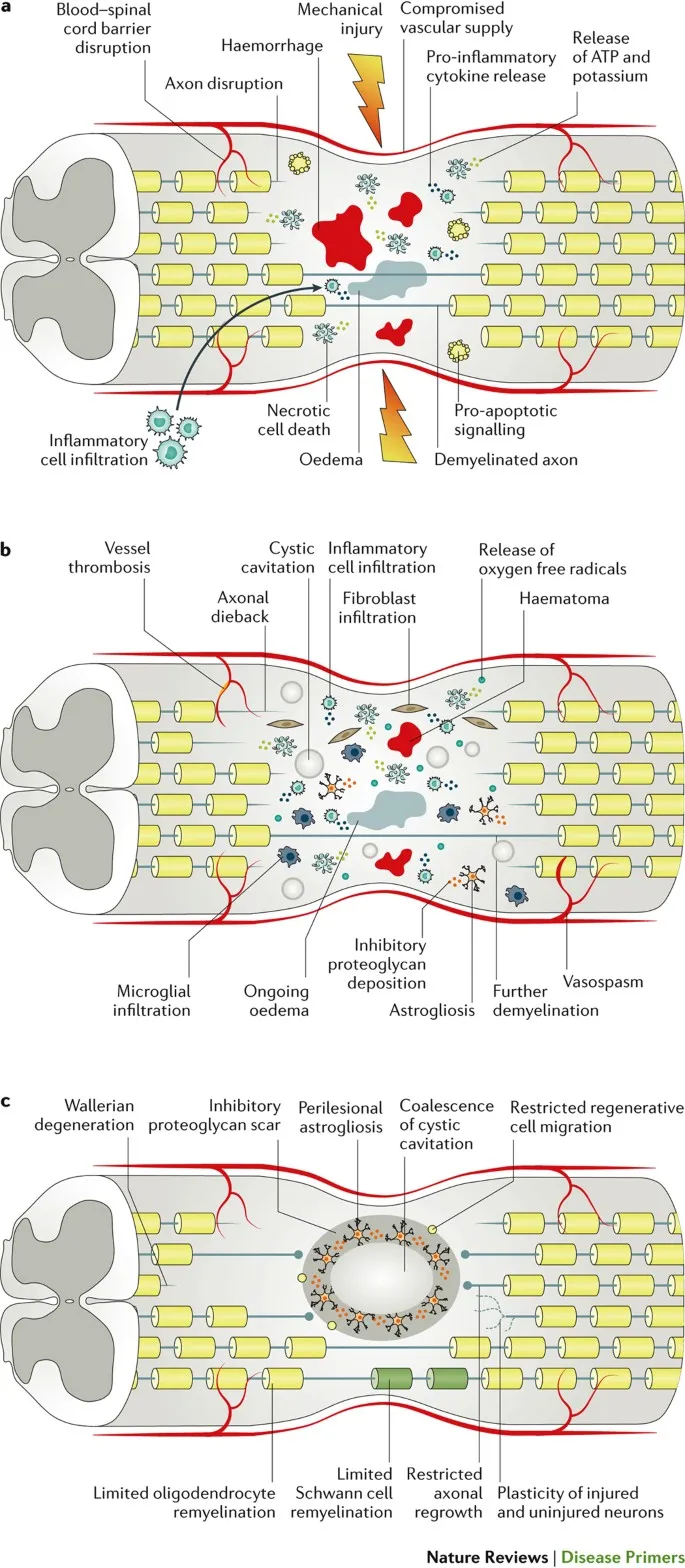
💥 Pathophysiology - Damage Cascade
- Primary Injury: Irreversible mechanical damage from the initial trauma (e.g., compression, laceration). This sets the stage for further damage.
- Secondary Injury: A delayed, progressive cascade that is a key therapeutic target. It evolves over hours to weeks, expanding the initial lesion.
⭐ Excitotoxicity is a major driver: excessive glutamate release overstimulates NMDA/AMPA receptors. This causes a massive influx of $Ca^{2+}$, activating proteases and lipases, leading to neuronal apoptosis and necrosis.
⚠️ Clinical Manifestations - Signs of Trouble
-
Spinal Shock:
- Transient loss of all spinal reflexes and flaccid paralysis below the injury level.
- Duration: hours to weeks.
- 💡 The return of the Bulbocavernosus Reflex (BCR) signals its end.
-
Neurogenic Shock: (Injury at or above T6)
- Distributive shock from loss of sympathetic tone.
- Classic triad: Hypotension (unopposed vagal tone), Bradycardia, Poikilothermia.
⭐ Distinguishing Shock: Spinal shock involves loss of reflexes (neurologic deficit). Neurogenic shock involves loss of sympathetic tone (hemodynamic instability). A patient can have both.
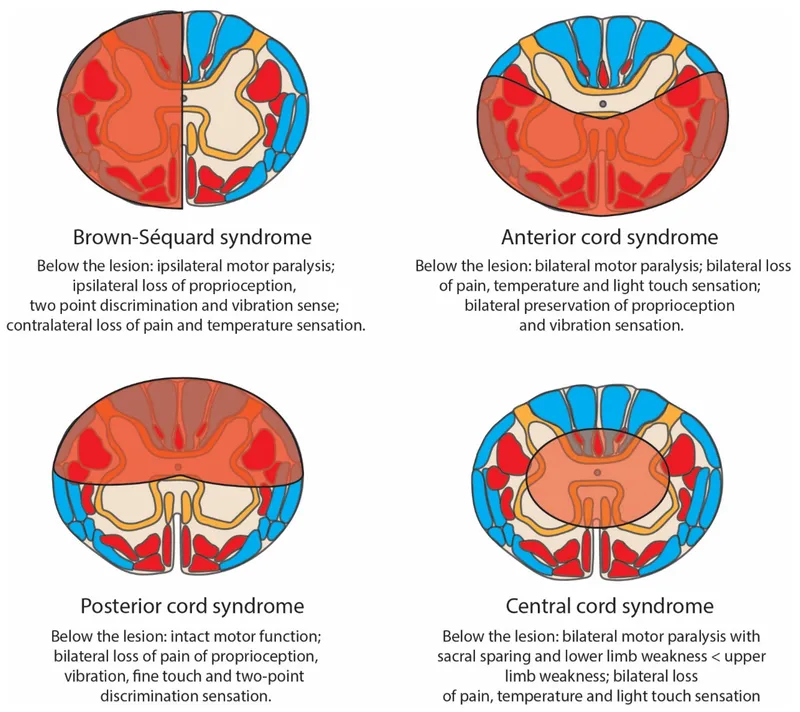
- Incomplete Cord Syndromes:
- Anterior Cord: Motor, pain, temp loss. Dorsal columns (proprioception, vibration) spared.
- Central Cord: Upper extremity weakness > lower. Common in elderly hyperextension injuries.
- Brown-Séquard: Hemisection. Ipsilateral motor/proprioception loss; contralateral pain/temp loss.
🎯 Diagnosis - Pinpointing the Lesion
-
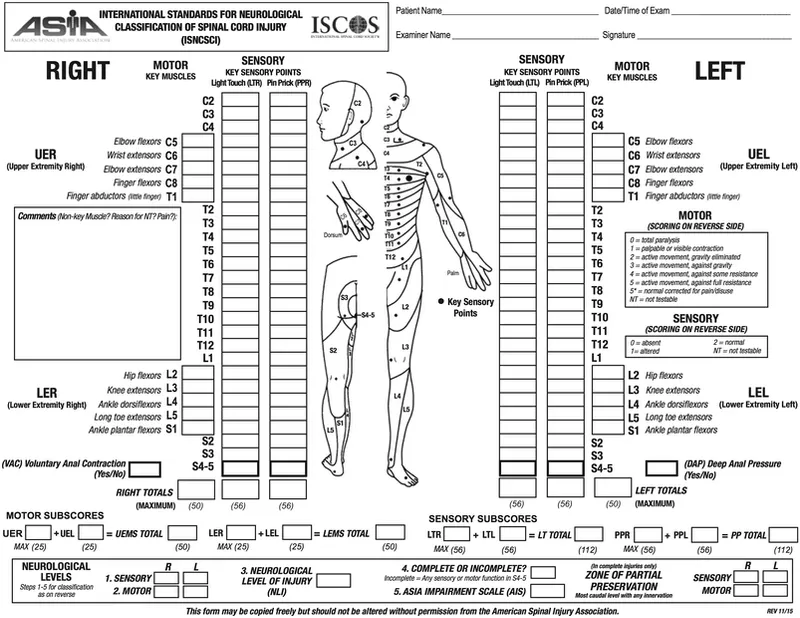
Neurological Exam:
- Assess motor (myotomes), sensory (dermatomes: pinprick, light touch), and deep tendon reflexes.
- 📌 Key: Check for sacral sparing (S4-S5 sensation, voluntary anal contraction) to determine if injury is complete vs. incomplete.
-
ASIA Impairment Scale: Standardizes injury severity.
- A: Complete (no motor/sensory in S4-S5)
- B: Sensory Incomplete
- C/D: Motor Incomplete (differentiated by muscle grade <3 or ≥3)
- E: Normal
-
Imaging:
- CT (non-contrast): Best initial test for bony fractures & malalignment.
- MRI: Gold standard for cord parenchyma, ligaments, and hematomas.
⭐ Sacral sparing is the most critical finding distinguishing an incomplete (ASIA B-D) from a complete (ASIA A) injury, significantly impacting prognosis.
🚑 Management - The Rescue Mission
- Pre-hospital: Immediate spinal immobilization (rigid collar, backboard).
- Airway: Secure airway early; high cervical injuries (C3-C5) risk respiratory failure.
- Circulation: Aggressively manage hypotension (neurogenic shock).
- Medical:
- DVT prophylaxis (e.g., LMWH).
- Stress ulcer prophylaxis (e.g., PPIs).
- Surgical: Decompression and/or stabilization for unstable fractures, cord compression, or progressive neurological deficit.
- ⚠️ Steroids: High-dose methylprednisolone is no longer recommended as standard practice due to increased risk of complications (infection, GI bleed).
⭐ Maintain Mean Arterial Pressure (MAP) at 85-90 mmHg for the first 7 days post-injury to optimize spinal cord perfusion and prevent secondary injury.
⚡ Biggest Takeaways
- ABCDEs first, with strict cervical spine immobilization until cleared.
- Neurogenic shock (injury ≥T6): hypotension + bradycardia. Treat with IVF and vasopressors.
- Spinal shock: transient areflexia and flaccid paralysis. Ends with return of bulbocavernosus reflex.
- High-dose steroids (methylprednisolone) are not standard of care due to high risk of complications.
- Autonomic dysreflexia (injury ≥T6): severe HTN, bradycardia, sweating. Sit patient up, remove stimulus.
- Injuries above C5 risk respiratory failure from diaphragmatic paralysis (phrenic nerve).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

