🧬 Anatomy - Nerve Network Blueprint
- Epineurium: Outermost dense connective tissue sheath enclosing the entire nerve; contains the vasa nervorum.
- Perineurium: Surrounds each nerve fascicle (a bundle of axons).
- Forms the blood-nerve barrier, regulating the endoneurial microenvironment.
- Endoneurium: Delicate connective tissue surrounding individual nerve fibers (axons) and their associated Schwann cells.
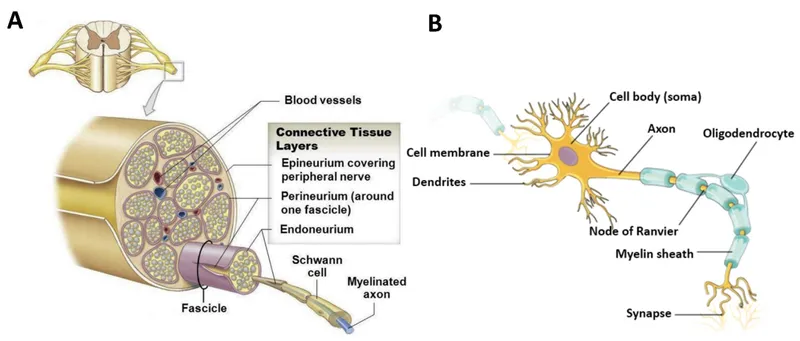
- Schwann Cells: Glial cells of the PNS that produce the myelin sheath. One Schwann cell myelinates one segment of a single axon.
⭐ The Perineurium is the key layer for surgical coaptation (nerve repair). Aligning fascicles using perineurial sutures is critical for successful axonal regeneration and functional recovery.
⚡ Pathology - When Nerves Snap
- Wallerian Degeneration: An active process of anterograde degeneration affecting the axon and myelin sheath distal to an injury site (occurs in axonotmesis/neurotmesis). Begins within 24-72 hours.
- Cleanup: Axonal cytoskeleton disintegrates; myelin breaks into ovoids. Macrophages are recruited to phagocytose debris.
- Regeneration: The proximal stump forms axonal sprouts. Schwann cells proliferate, forming Bands of Büngner that guide sprouts toward their distal target.
⭐ Axonal regeneration proceeds at ~1 mm/day or 1 inch/month. This slow rate is critical for predicting recovery time and preventing irreversible muscle atrophy after ~18-24 months.
Nerve Injury Classifications
| Seddon Class | Sunderland Grade | Key Structure Damaged | Prognosis & Notes |
|---|---|---|---|
| Neuropraxia | I | Myelin (focal demyelination) | Excellent; full recovery in days/weeks. |
| Axonotmesis | II | Axon (endoneurium intact) | Good; requires axonal regeneration. |
| III | + Endoneurium | Fair; intrafascicular fibrosis can block. | |
| IV | + Perineurium | Poor; neuroma-in-continuity common. | |
| Neurotmesis | V | Full Transection (epineurium) | Very poor; requires surgical repair. |
⚡ Clinical - Shocking Solutions & Fixes
-
Diagnosis:
- History & Physical: Note sensory (paresthesia, numbness) & motor (weakness, atrophy) deficits.
- Provocative Tests: Tinel's sign (tapping nerve → distal tingling), Phalen's test (wrist flexion → median nerve symptoms).
-
Electrodiagnostics (EDx):
- Nerve Conduction Study (NCS): Differentiates pathology.
- ↓ Conduction Velocity → Demyelination (focal compression).
- ↓ Amplitude → Axonal loss (severe injury).
- Electromyography (EMG): Needle in muscle assesses denervation.
- Fibrillations & positive sharp waves indicate active denervation.
- Nerve Conduction Study (NCS): Differentiates pathology.
⭐ Wallerian degeneration (axonal breakdown distal to injury) begins 24-72 hours post-injury. However, EMG changes like fibrillations are not apparent for 2-3 weeks, making early EMG less useful for acute transection prognosis.
- Management Flow:
⚡ Biggest Takeaways
- Seddon classification guides management: Neurapraxia (conduction block, full recovery), Axonotmesis (axon loss, sheath intact), and Neurotmesis (transection, requires surgery).
- Wallerian degeneration is the breakdown of the axon distal to the injury site in axonotmesis and neurotmesis.
- Nerve regeneration proceeds at ~1 mm/day (1 inch/month); a positive Tinel's sign tracks progress.
- EMG/NCS are essential to localize the lesion and assess severity and recovery.
- Surgical options for neurotmesis include direct repair, nerve grafting (sural nerve donor), or nerve transfer.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

