💨 Core principles - Gas, Light, & Action!
-
Gas (Pneumoperitoneum):
- Insufflation: Carbon Dioxide ($CO_2$) is standard.
-
- Why $CO_2$? Non-flammable, high blood solubility (↓ embolism risk), rapidly excreted via lungs.
-
- Pressure: Maintained at 12-15 mmHg.
- Access: Veress needle (blind) or Hasson technique (open cut-down).
- ⚠️ Complications: Hypercarbia, respiratory acidosis, subcutaneous emphysema, gas embolism.
- Insufflation: Carbon Dioxide ($CO_2$) is standard.
-
Light (Vision System):
- Components: Light source (Xenon/LED) → Laparoscope (camera) → Monitor.
- Scopes: 0° for direct view; 30° angled scope to visualize around structures.
-
Action (Instruments):
- Trocars: Ports for instrument entry (e.g., 5mm, 12mm).
- Core Tools: Graspers, dissectors (e.g., Maryland), scissors, energy devices.
⭐ High-Yield: A sudden drop in end-tidal $CO_2$, hypotension, and a "mill-wheel" murmur suggest a venous gas embolism. Immediately stop insufflation and place the patient in the left lateral decubitus (Durant's) position.
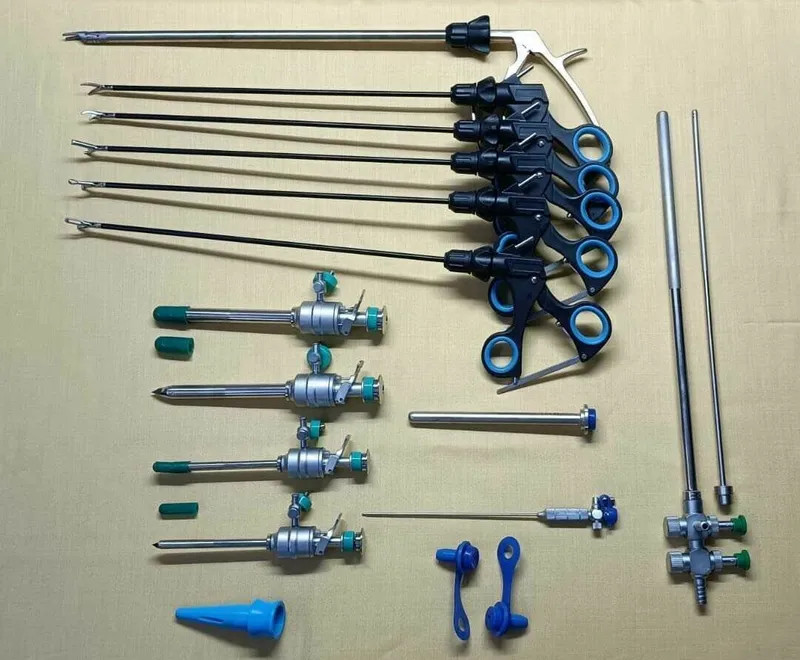
🛠️ The Laparoscopic Toolbox
Fundamental instruments for minimally invasive surgery, enabling access, visualization, and manipulation within a closed abdomen.
-
Access & Insufflation
- Veress Needle: Blind, spring-loaded needle for initial CO₂ insufflation.
- Hasson Trocar: Open cut-down technique for the first port; safer with prior abdominal surgery.
- Trocars: Ports for instrument passage, typically 5-12 mm diameter.
- Insufflator: Delivers CO₂ to create pneumoperitoneum, maintaining pressure at 12-15 $mmHg$.
-
Visualization & Manipulation
- Laparoscope: Telescope with a camera and light source (0° or 30° view).
- Graspers: Atraumatic (e.g., Babcock) for delicate tissue; traumatic for tissue to be resected.
- Dissectors: e.g., Maryland dissector for fine tissue separation.
- Energy Devices: Monopolar (requires grounding pad) vs. Bipolar (safer, current confined between tips).
⭐ The most feared complication of Veress needle or primary trocar insertion is major vascular injury (aorta, IVC, iliac vessels).
⚠️ Complications - When Tools Turn Treacherous
-
Access Injuries (Veress/Trocar):
- Risk of major vascular (aorta, IVC, iliacs) or visceral (bowel, bladder) injury.
- ⚠️ Highest risk during initial blind entry, especially with prior abdominal surgery (adhesions).
- Suspect with sudden hypotension or free blood on aspiration.
-
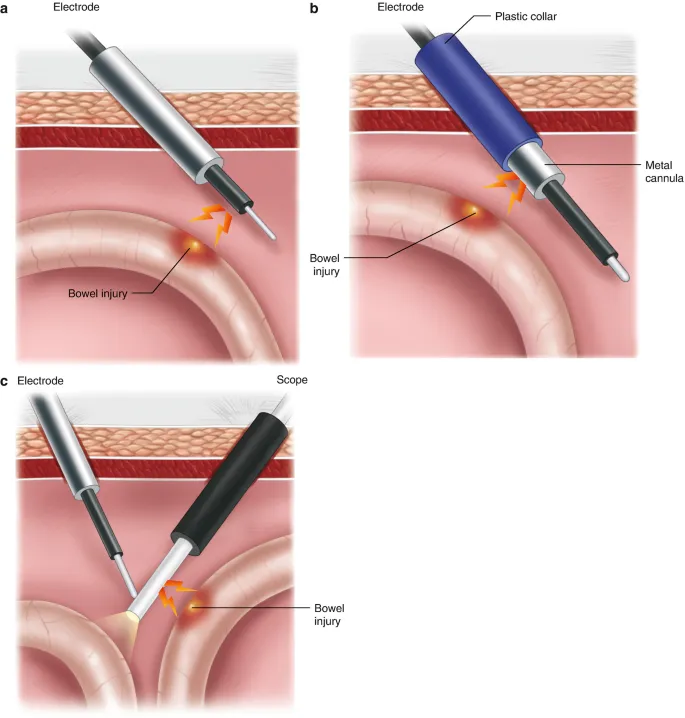
Electrosurgical Burns:
- Direct Coupling: Active electrode touches another metal instrument.
- Insulation Failure: Current leaks from a break in the instrument's sheath.
- Capacitive Coupling: Stray current induced in a non-contacted conductor.
⭐ Delayed Presentation: Bowel thermal injuries are often missed intra-op. Suspect in patients presenting with fever, abdominal pain, and leukocytosis 2-7 days post-laparoscopy.
🛠️ Management - The Damage Control Crew
- Hemostasis: The primary goal in managing intra-op complications.
- Vessel Ligation: Titanium clips (Hemoclips) or absorbable clips (Lapro-clips).
- Energy Devices: Control bleeding from small vessels to larger pedicles.
- Ultrasonic (Harmonic Scalpel): Cuts & coagulates with minimal thermal spread.
- Advanced Bipolar (LigaSure): Fuses vessel walls.
- Suturing: Intracorporeal suturing for complex repairs or large vessel control.
- Containment: Endo-bags for specimen retrieval prevent contamination or tumor seeding.
⭐ The most feared complication is unrecognized thermal bowel injury, often from monopolar cautery's wide energy spread.
⚡ Biggest Takeaways
- Pneumoperitoneum uses CO2 at 12-15 mmHg; its high solubility prevents fatal gas embolism.
- The Hasson (open) technique is safer than the blind Veress needle, especially with abdominal adhesions.
- Bipolar cautery is safer than monopolar (no grounding pad, less stray current).
- ↑IAP causes ↓ venous return, ↓ cardiac output, and ↑ SVR.
- Hypercarbia from CO2 absorption can lead to respiratory acidosis.
- Most feared complications are major vascular/bowel injury during access and gas embolism.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

