🎭 The Unwanted Encore
-
Immediate (<24h):
- Hemorrhage: ↓BP, ↑HR. Check CBC, coagulation studies. May require fluid resuscitation, transfusion, or return to OR.
- Ureteral/Bladder/Bowel Injury: Often iatrogenic. Suspect with flank pain, hematuria, oliguria, or peritonitis.
-
Early (24h - 30d):
- Infection: Surgical Site Infection (SSI), UTI, pelvic abscess.
- Venous Thromboembolism (VTE): DVT/PE. Prophylaxis is key.
- Ileus: Common; prolonged if >3-5 days.
- Wound Dehiscence/Evisceration: Surgical emergency.
-
Late (>30d):
- Adhesions: Can lead to chronic pain or small bowel obstruction.
- Fistula: Vesicovaginal (painless, continuous watery discharge), Rectovaginal.
- Incisional Hernia, Pelvic Organ Prolapse.
⭐ Post-op Fever Workup: Remember the 5 W's: Wind (Atelectasis, POD 1-2) Water (UTI, POD 3-5) Wound (SSI, POD 5-7) Walking (VTE, POD 7+) Wonder drugs (Anytime)
🚩 Clinical Manifestations - Reading the Red Flags
- Hemorrhage/Hematoma: Tachycardia, hypotension, ↓ Hct, oliguria. Presents with vaginal bleeding, a palpable pelvic mass, or flank pain (retroperitoneal).
- Infection (SSI/Abscess): Fever > 38°C after POD #2, leukocytosis.
- SSI: Localized erythema, induration, purulent drainage.
- Abscess: Persistent fever despite antibiotics, localized pain, ileus.
- Thromboembolism (DVT/PE):
- DVT: Unilateral leg swelling, pain, erythema.
- PE: Sudden dyspnea, pleuritic chest pain, tachycardia, hypoxia.
- Urogenital Injury:
- Ureteral: Flank pain, fever, ileus, ↑ Cr.
- Bladder/Fistula: Hematuria, oliguria, or continuous watery vaginal discharge.
⭐ 📌 Mnemonic for Post-Op Fever ("5 Ws"):
- Wind (Atelectasis): POD 1-2
- Water (UTI): POD 3-5
- Walk (DVT/PE): POD 4-6
- Wound (SSI): POD 5-7
- Wonder Drugs/What did we do? (Abscess, Drug Fever): >POD 7
🕵️♀️ Diagnosis - The Clinical Detective
📌 5 W's of Post-Op Fever:
- Wind (Atelectasis/PNA): POD 1-2. Dx: Chest X-ray.
- Water (UTI): POD 3-5. Dx: Urinalysis, culture.
- Wound (SSI): POD 5-7. Dx: Exam (erythema, drainage), CT for deep abscess.
- Walking (DVT/PE): POD >5. Dx: Doppler US, CT Angiography.
- Wonder Drugs/Abscess: POD >7. Dx: Review meds, CT scan.
- Hemorrhage: Assess vitals, CBC. Pelvic US for hematoma; CT-A for active extravasation.
- Urogenital Injury:
- Ureter: ↑Cr, flank pain. Dx: CT urogram, retrograde pyelogram.
- Bladder: Gross hematuria. Dx: Retrograde cystogram.
⭐ Ureteral injury often presents subtly 5-10 days post-op with flank pain, fever, or watery vaginal discharge (urinoma), not immediate anuria.
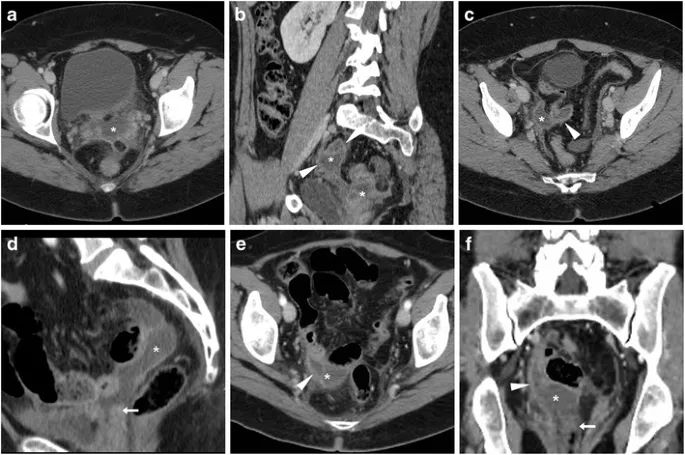
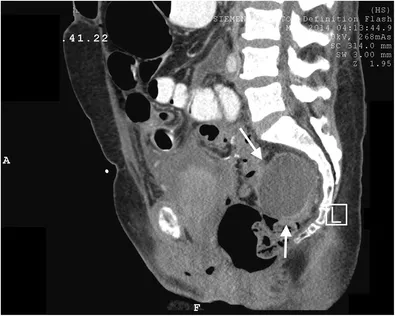
🩹 Management - Damage Control
- Goal: Rapidly stabilize critically ill patients with massive hemorrhage by abbreviating the initial operation.
- Indications: Hemodynamic instability, massive transfusion protocol activation, and development of the lethal triad.
- Key Steps:
- Control Bleeding: Peri-uterine/pelvic packing, vessel ligation (e.g., uterine, internal iliac).
- Control Contamination: Rapid resection of necrotic/perforated tissue.
- Temporary Closure: Use of vacuum-assisted closure (VAC) or Bogota bag.
⭐ Lethal Triad: The vicious cycle of hypothermia (<35°C), metabolic acidosis (pH <7.2), and coagulopathy (INR >1.5). Damage control surgery aims to break this cycle.
⚡ Biggest Takeaways
- Post-op fever follows the "5 W's": Atelectasis (POD 1-2) is most common, then UTI and wound infection.
- Ureteral injury is a key risk during hysterectomy near the uterine artery ("water under the bridge").
- Vaginal cuff dehiscence is a surgical emergency, presenting with a fluid gush and potential bowel evisceration.
- Femoral nerve injury from retractors causes impaired knee extension and loss of the patellar reflex.
- Obturator nerve injury from lymphadenectomy causes weak thigh adduction.
- VTE (DVT/PE) is a major mortality risk; prophylaxis is critical.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

