🌪️ Pathophysiology - The Ovarian Twist
- The ovary and fallopian tube twist around the infundibulopelvic (suspensory) ligament and the utero-ovarian ligament.
- This rotation initially obstructs the low-pressure venous and lymphatic outflow, leading to congestion, edema, and ovarian enlargement.
- Continued swelling and twisting eventually compromise the high-pressure arterial inflow, causing ischemia and hemorrhagic infarction.
⭐ The presence of arterial flow on Doppler ultrasound does NOT rule out ovarian torsion, as venous occlusion occurs first.
😱 Clinical Manifestations - Sudden, Sharp & Scary
- Pain:
- Sudden-onset, severe, unilateral lower abdominal/pelvic pain.
- Character: Sharp, stabbing, or colicky.
- Radiation: May radiate to flank, back, or groin.
- Intermittent pain suggests episodes of torsion and detorsion.
- Associated Symptoms:
- Nausea & vomiting are very common (~70%).
- Low-grade fever may be present.
- Physical Exam:
- Unilateral adnexal tenderness.
- Palpable adnexal mass.
- ⚠️ Peritoneal signs (guarding, rebound) suggest ischemia or necrosis.
⭐ While the classic presentation is acute, ~50% of patients report subacute, intermittent pain for days or weeks before the acute event.
🩺 Diagnosis - Spotting the Spin
-
Initial Workup:
- Based on high clinical suspicion (acute severe pain, nausea/vomiting, adnexal mass).
- Labs: Stat β-hCG to rule out ectopic pregnancy, CBC.
-
Imaging Gold Standard: Pelvic Ultrasound with Doppler.
- Key Findings:
- Unilateral enlarged, edematous ovary (>4 cm).
- Peripherally displaced follicles.
- 💡 "Whirlpool sign": pathognomonic finding of a twisted pedicle.
- ↓ or absent blood flow on Doppler (venous flow lost before arterial).
- Key Findings:
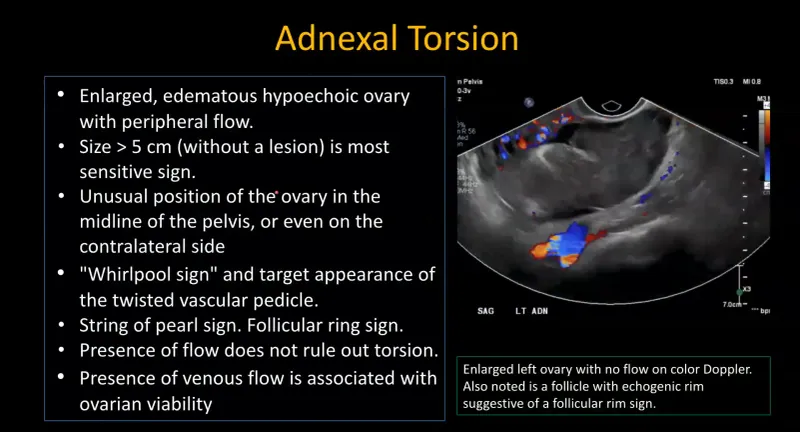
⭐ High-Yield: Normal Doppler flow is seen in up to 60% of surgically confirmed cases and does NOT rule out torsion. Clinical suspicion dictates management.
- Definitive Diagnosis: Direct visualization via laparoscopy.
✂️ Management - Untwist and Untack
- Approach: Urgent surgical exploration, typically via laparoscopy.
- Primary Goal: Ovarian salvage.
- Procedure Steps:
- Detorsion (Untwist): The twisted adnexa is untwisted to restore blood flow.
- Cystectomy: If a benign cyst is the lead point, it is removed while preserving ovarian tissue.
- Oophoropexy (Tack): Consider suturing the ovary to the pelvic sidewall to prevent recurrence, especially in pediatric patients.
- Salpingo-oophorectomy: Reserved for necrotic, non-viable tissue or suspected malignancy.
⭐ Even a dusky or "black" appearing ovary should be untwisted and conserved. Ovarian color is a poor predictor of viability; most regain function after reperfusion.
🌪️ Complications - The Twisted Aftermath
- Ovarian Necrosis/Infarction: Most severe outcome from prolonged ischemia, leading to irreversible tissue death and loss of function.
- Infertility: Risk ↑ with oophorectomy (if ovary is non-viable) or significant damage.
- Peritonitis/Sepsis: From ruptured necrotic tissue or secondary infection.
- Hemorrhage & Adhesions: Post-operative risks.
⭐ Pearl: A dusky, cyanotic ovary upon detorsion does not mandate oophorectomy. Many regain viability and function.
⚡ High-Yield Points - Biggest Takeaways
- Sudden, severe unilateral pelvic pain with nausea/vomiting is the classic presentation.
- Ultrasound with Doppler is the initial imaging of choice, showing an enlarged ovary with absent/decreased blood flow.
- Definitive diagnosis is made via direct surgical visualization.
- Management is urgent diagnostic laparoscopy with detorsion to attempt ovarian conservation.
- A necrotic-appearing ovary should still be detorsed and conserved in premenopausal women.
- Salpingo-oophorectomy is considered for postmenopausal patients or suspected malignancy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

