🔪 Core Concept - The Why & The What
-
Primary Goals (The Why):
- Restore Function: Correcting severe reflux (GERD), obstruction (achalasia, strictures), or dysphagia.
- Resect Pathology: Removing malignancy (adenocarcinoma, SCC) or large diverticula (Zenker's).
- Repair Anatomy/Injury: Managing large hiatal hernias or life-threatening perforations (e.g., Boerhaave syndrome).
-
Key Procedures (The What):
- Fundoplication (e.g., Nissen): Reinforces the Lower Esophageal Sphincter (LES) for GERD.
- Heller Myotomy: Divides LES muscle fibers for achalasia.
- Esophagectomy: Resection of esophagus, typically with gastric pull-up for reconstruction.
⭐ Post-esophagectomy, the stomach replaces the resected esophagus. Patients must eat small, frequent meals and remain upright after eating to prevent reflux and dumping syndrome.
🔪 Management - The Surgical Playbook
-
Nissen Fundoplication (360° wrap):
- Indication: Medically refractory GERD, large hiatal hernias.
- Procedure: Gastric fundus is mobilized and wrapped completely around the distal esophagus to augment LES pressure.
- ⚠️ Complications: Dysphagia ("too tight"), gas-bloat syndrome.
-
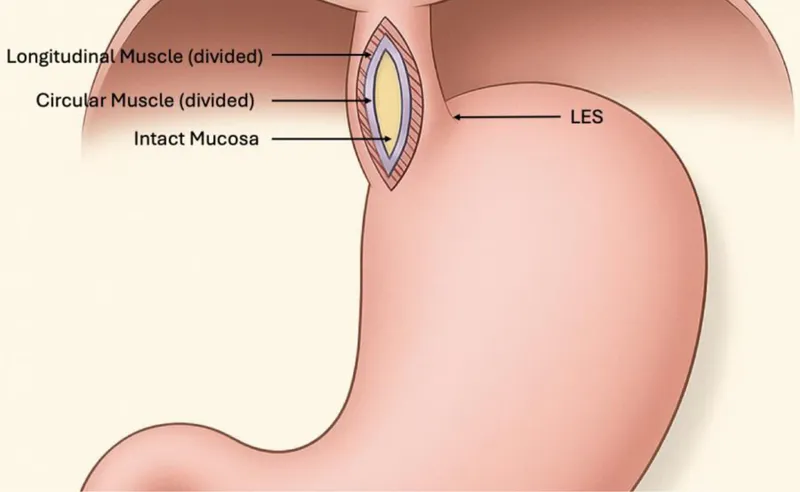
Heller Myotomy:
- Indication: Achalasia.
- Procedure: Longitudinal myotomy of the LES and proximal gastric cardia.
- 💡 Often combined with a partial fundoplication (e.g., Dor) to prevent post-op GERD.
-
Esophagectomy:
- Indication: Resectable esophageal cancer, high-grade dysplasia, end-stage benign disease.
- Reconstruction: Gastric pull-up is the most common conduit; colon or jejunum are alternatives.
- Major Risk: Anastomotic leak.
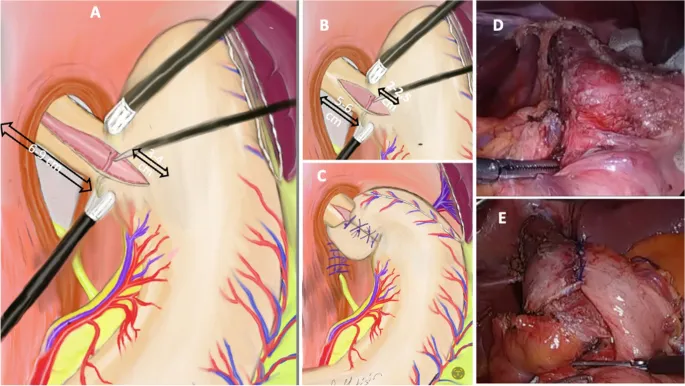
⭐ During esophagectomy, injury to the vagus nerves is common. This denervates the pylorus, often necessitating a drainage procedure (pyloroplasty/pyloromyotomy) to prevent delayed gastric emptying.
⚠️ Complications - Post-Op Pitfalls
- Anastomotic Leak (Most Feared)
- Timing: Post-op days 5-7.
- Signs: Fever, tachycardia, chest pain, sepsis, pleural effusion (often left-sided).
- Dx: CT with oral contrast or gastrografin swallow.
- Mgmt: NPO, broad-spectrum antibiotics, drainage (percutaneous/surgical), possible stent or re-operation.
⭐ Suspect an anastomotic leak in any esophagectomy patient with new-onset atrial fibrillation or sepsis post-op day 5-7. It's a surgical emergency.
-
Recurrent Laryngeal Nerve (RLN) Injury
- Presentation: Hoarseness, weak cough, aspiration.
- Cause: Traction/transection during cervical dissection.
-
Chylothorax
- Cause: Thoracic duct injury.
- Sign: High-volume, milky-white chest tube output.
- Dx: Fluid triglycerides > 110 mg/dL.
- Mgmt: NPO, TPN, octreotide; may require surgical ligation.
-
Late Complications
- Anastomotic Stricture: Dysphagia months later. Tx: Endoscopic dilation.
- Dumping Syndrome: Due to vagotomy.
⚡ Biggest Takeaways
- Nissen fundoplication (360° wrap) for GERD risks postoperative dysphagia and gas-bloat syndrome.
- Heller myotomy for achalasia cuts the LES; a partial fundoplication is added to prevent iatrogenic reflux.
- Esophagectomy for cancer has high morbidity; anastomotic leak is a life-threatening complication.
- Ivor Lewis esophagectomy uses a thoracic anastomosis; Transhiatal esophagectomy uses a cervical anastomosis, risking recurrent laryngeal nerve injury.
- Zenker's diverticulum repair requires a cricopharyngeal myotomy.
- Boerhaave syndrome is a surgical emergency requiring primary repair.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

