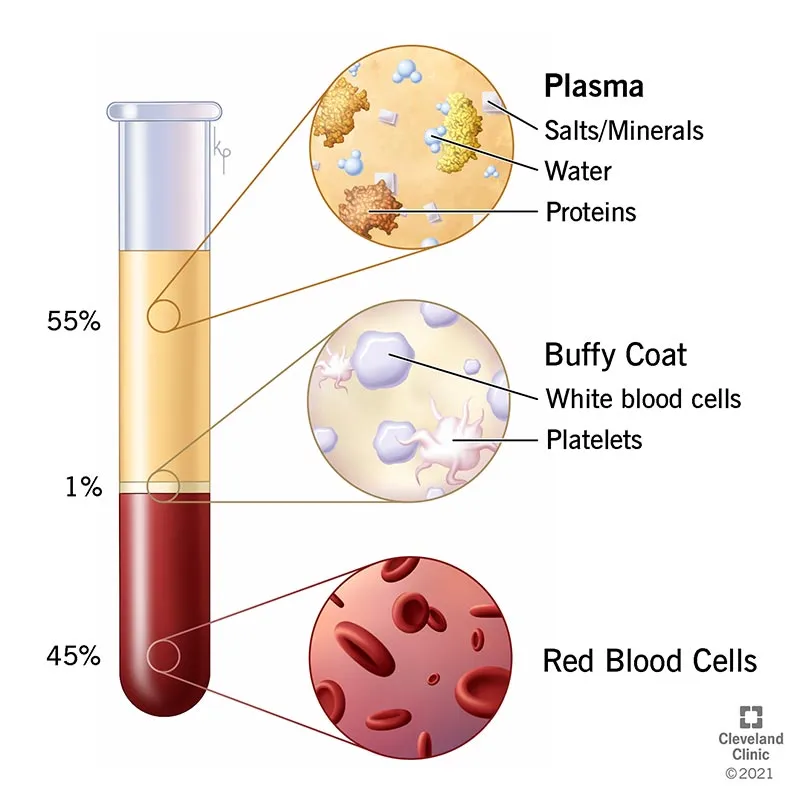
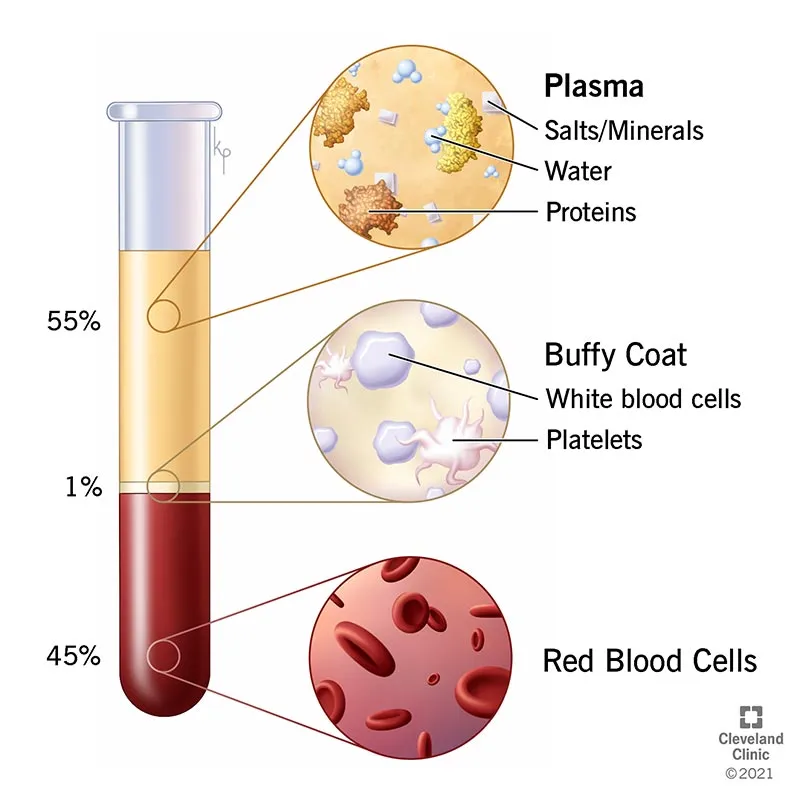
Blood Components - The Bloody Basics
- Packed Red Blood Cells (PRBCs): ↑ O₂ capacity & tissue perfusion. 1 unit (~300mL) ↑ Hb by 1 g/dL & Hct by 3%.
- Platelets: For active bleeding with thrombocytopenia (<50,000/μL) or dysfunction. 1 apheresis pack ↑ count by 30-60k.
- Fresh Frozen Plasma (FFP): Replaces all clotting factors. Use for coagulopathy (INR >1.5), warfarin reversal.
- Cryoprecipitate: Concentrated fibrinogen, vWF, Factor VIII. Use for fibrinogen <100-150 mg/dL.
⭐ FFP from an AB donor is universal because it contains no anti-A or anti-B antibodies.
RBC Transfusion - Seeing Red Signals
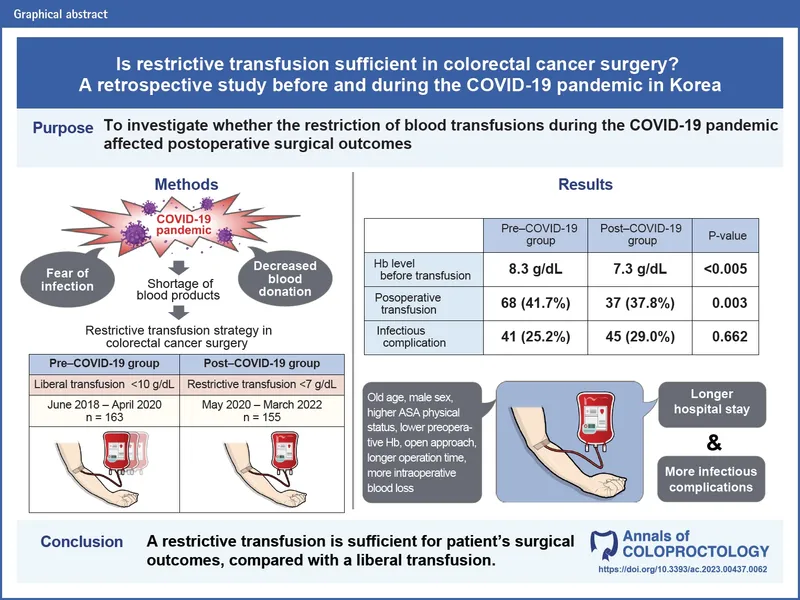
- Restrictive Strategy (Standard): Transfuse for Hemoglobin (Hgb) < 7 g/dL.
- Target Hgb: 7-9 g/dL.
- Liberal Strategy (Exceptions): Consider for Hgb < 8 g/dL in specific cases:
- Acute Coronary Syndrome (ACS) with active ischemia.
- Symptomatic anemia (e.g., chest pain, dyspnea).
- Active bleeding / hemorrhagic shock.
- Each unit of packed RBCs (pRBCs) should ↑ Hgb by ~1 g/dL and Hematocrit (Hct) by ~3%.
⭐ In stable, hospitalized patients, a restrictive transfusion threshold of 7 g/dL is associated with better outcomes compared to a liberal strategy.
Platelets & Plasma - The Clotting Crew
-
Platelets (Thrombocytes): For severe thrombocytopenia or platelet dysfunction with active bleeding.
- Prophylactic Triggers:
- < 10,000/μL to prevent spontaneous hemorrhage.
- < 50,000/μL prior to most invasive procedures.
- < 100,000/μL for neuro/ocular surgery.
- Therapeutic: Active bleeding with platelets < 50,000/μL.
- Prophylactic Triggers:
-
Fresh Frozen Plasma (FFP): Replaces all clotting factors.
- Triggers:
- Active bleeding with INR > 1.7.
- Massive Transfusion Protocol (MTP): often a 1:1:1 ratio (RBC:FFP:Platelets).
- Triggers:
⭐ FFP requires ABO compatibility. For urgent warfarin reversal, Prothrombin Complex Concentrate (PCC) is faster than FFP.
Massive Transfusion - Code Red Tsunami
- Activation: For hemorrhagic shock. Defined as transfusion of >10 units pRBCs in 24 hrs, or >4 units in 1 hr.
- Strategy: Use a balanced 1:1:1 ratio of pRBCs:FFP:Platelets to mimic whole blood.
- Goals: Restore volume, reverse coagulopathy, and prevent the lethal triad.
⭐ Lethal Triad: MTP aims to prevent or reverse the deadly cycle of acidosis, hypothermia, and coagulopathy seen in massive hemorrhage.
Transfusion Reactions - When Good Blood Goes Bad
- Immediate Action: Stop transfusion, maintain IV access with normal saline.
- Common Types & Hallmarks:
- Acute Hemolytic: Type II HSR (ABO incompatibility). Fever, flank pain, hemoglobinuria. Positive Coombs test.
- Febrile Non-Hemolytic (FNHTR): Most common. Cytokine-mediated. Fever, chills, rigors.
- Allergic/Anaphylactic: Type I HSR. Urticaria, pruritus. Anaphylaxis if IgA-deficient.
- TRALI: Donor anti-leukocyte antibodies. Acute respiratory distress within 6 hours.
- TACO: Volume overload. Dyspnea, hypertension, pulmonary edema.
⭐ Febrile Non-Hemolytic Transfusion Reaction (FNHTR) is the most frequent reaction, managed with antipyretics. Leukoreduction of blood products can prevent it.
High-Yield Points - ⚡ Biggest Takeaways
- A restrictive transfusion strategy (trigger Hb <7 g/dL) is generally preferred for most stable, hospitalized patients.
- Consider a higher threshold (Hb <8 g/dL) for patients with symptomatic cardiovascular disease or those undergoing cardiac/orthopedic surgery.
- Transfuse for symptomatic anemia (e.g., chest pain, dyspnea) regardless of the absolute Hb value.
- For massive hemorrhage, activate the Massive Transfusion Protocol (MTP) with a 1:1:1 ratio of pRBCs:FFP:Platelets.
- Transfuse platelets if <10,000/µL or <50,000/µL before major surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

