Ongoing Losses - The Body's Leaks
Ongoing losses are abnormal fluid and electrolyte deficits occurring in real-time, distinct from maintenance or pre-existing deficit corrections. Replacement therapy must match the volume and composition of the fluid being lost.
- Gastrointestinal (GI):
- Nasogastric tube (NGT) output, emesis
- Fistula / Stoma output
- Diarrhea
- Renal:
- Polyuria (e.g., diabetes insipidus)
- Insensible / Third Space:
- Fever, tachypnea
- Burns, pancreatitis, sepsis
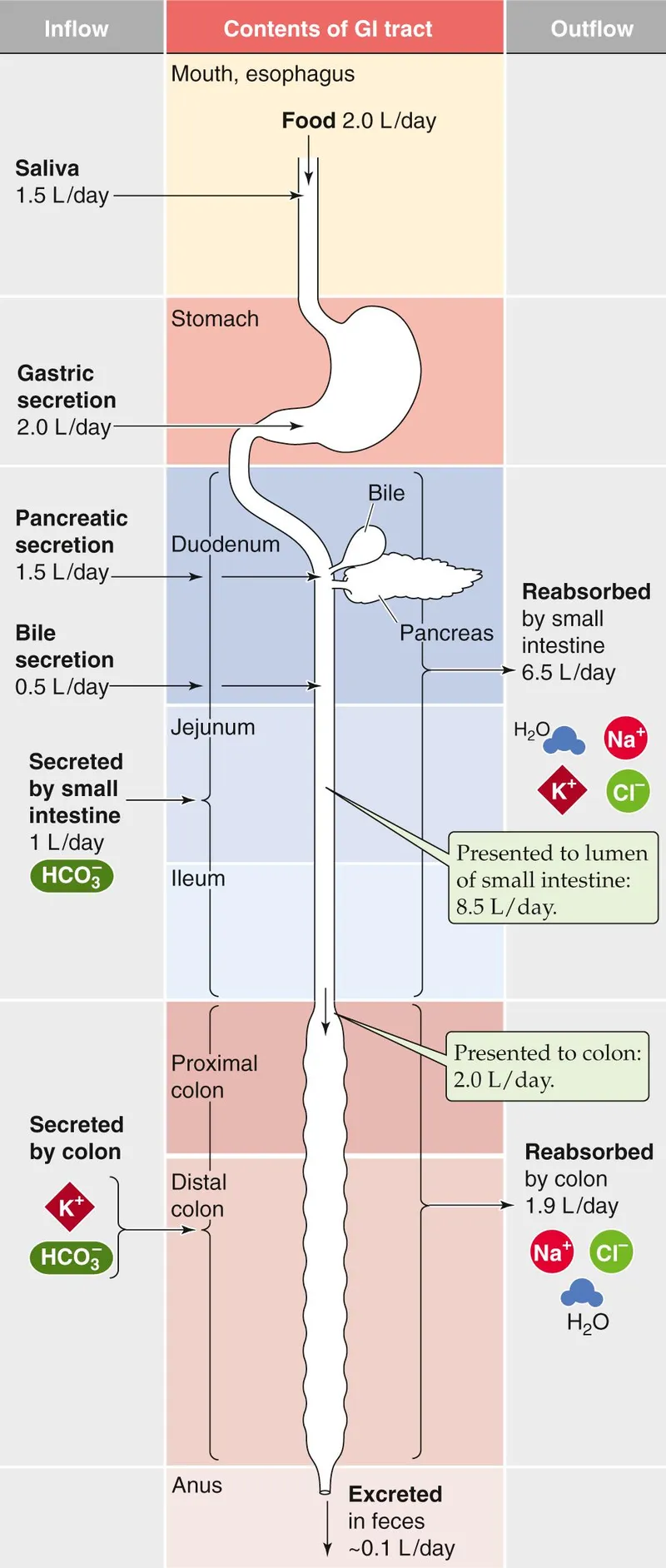
⭐ Gastric fluid is rich in H⁺, Cl⁻, and K⁺. Large volume losses via NGT suction or vomiting classically cause hypochloremic, hypokalemic metabolic alkalosis.
Fluid Composition - What's in the Goo?
Knowing the electrolyte profile of lost fluids is key to selecting appropriate replacement therapy. Values are typical mEq/L ranges.
| Fluid Source | $Na^+$ | $K^+$ | $Cl^-$ | $HCO_3^-$ |
|---|---|---|---|---|
| Saliva | 10 | 26 | 10 | 30 |
| Gastric (Stomach) | 60 | 10 | 130 | 0 |
| Pancreatic | 140 | 5 | 75 | 115 |
| Bile | 145 | 5 | 100 | 35 |
| Small Bowel | 110 | 5 | 105 | 30 |
| Diarrhea/Ileostomy | 130 | 20-30 | 110 | 45 |
- Pancreatic/Bile/Small Bowel: High in $HCO_3^-$. Losses from fistulas or drains can cause metabolic acidosis.
⭐ Exam Favorite: Diarrheal fluid is rich in potassium and bicarbonate. Significant losses, especially in children, can rapidly lead to hypokalemia and non-anion gap metabolic acidosis.
Replacement Strategy - The Right Stuff
- Principle: Replace ongoing losses volume-for-volume (e.g., mL-for-mL) in a set time frame, typically every 4-6 hours.
- Fluid Choice Algorithm: The replacement fluid depends on the source of the loss. Match the effluent with the appropriate solution.
⭐ For high-volume nasogastric tube (NGT) output (>1.5 L/day), check gastric fluid electrolytes every 12h and tailor replacement fluids accordingly to prevent metabolic alkalosis.
Monitoring - Checking the Gauges
- Key Indicators & Targets:
- Urine Output: Goal is >0.5 mL/kg/hr.
- Vitals: Normalizing HR, BP.
- Daily Weights: Sensitive indicator of net fluid balance.
- Labs: Serial electrolytes, BUN/Cr.
- Exam: Moist mucous membranes, normal skin turgor, no edema.
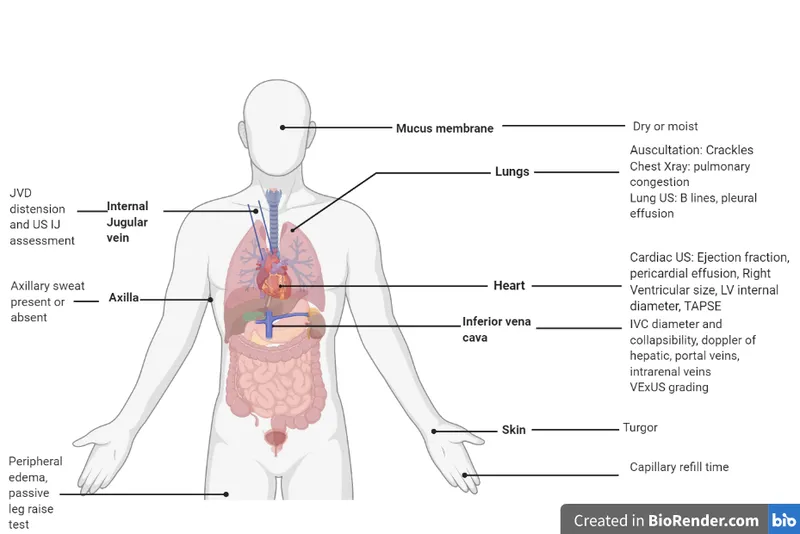
⭐ In elderly patients, skin turgor is less reliable due to decreased elasticity; check mucous membranes for a more accurate assessment of hydration status.
High-Yield Points - ⚡ Biggest Takeaways
- Gastric losses (e.g., NG tube) cause hypokalemic, hypochloremic metabolic alkalosis; replace with Normal Saline + KCl.
- Pancreatic, biliary, or high-output ileostomy losses are rich in bicarbonate, causing normal anion gap metabolic acidosis.
- Replace bicarbonate-rich losses with an isotonic fluid like Lactated Ringer's to prevent acidosis.
- Guide replacement by monitoring serum electrolytes, urine output (>0.5 mL/kg/hr), and vital signs.
- Account for third-space losses post-op or in sepsis with isotonic crystalloids.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

