🗺️ The Nerve's Journey
- A branch of the Vagus Nerve (CN X), the RLN has an asymmetric thoracic course before ascending into the neck.
- Right RLN: Loops inferior to the right subclavian artery. Has a shorter, more oblique path.
- Left RLN: Loops inferior to the aortic arch (near the ligamentum arteriosum). Has a longer, more vertical path.
- Both ascend in the tracheoesophageal groove, closely related to the Inferior Thyroid Artery (ITA), to enter the larynx.
⭐ A Non-Recurrent Laryngeal Nerve (NRLN) is a rare anomaly (~1%), almost always on the right, linked to an aberrant right subclavian artery (arteria lusoria). High risk of iatrogenic injury.
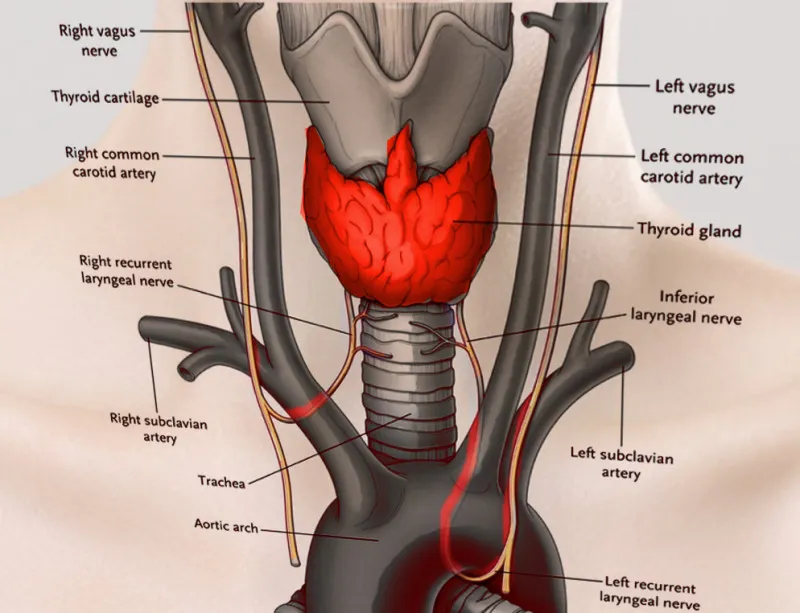
🗣️ Anatomy: Functional relevance - The Voice Box Boss
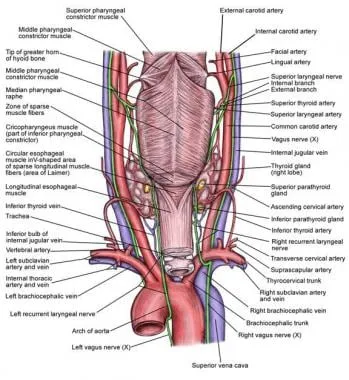
- Origin: Branch of the Vagus nerve (CN X).
- Motor: Innervates all intrinsic laryngeal muscles except the cricothyroid (innervated by the superior laryngeal nerve).
- Posterior Cricoarytenoid (PCA): The only vocal cord abductor.
- 📌 Mnemonic: PCA = Pulls Cords Apart.
- Sensory: Sensation to the larynx below the vocal cords.
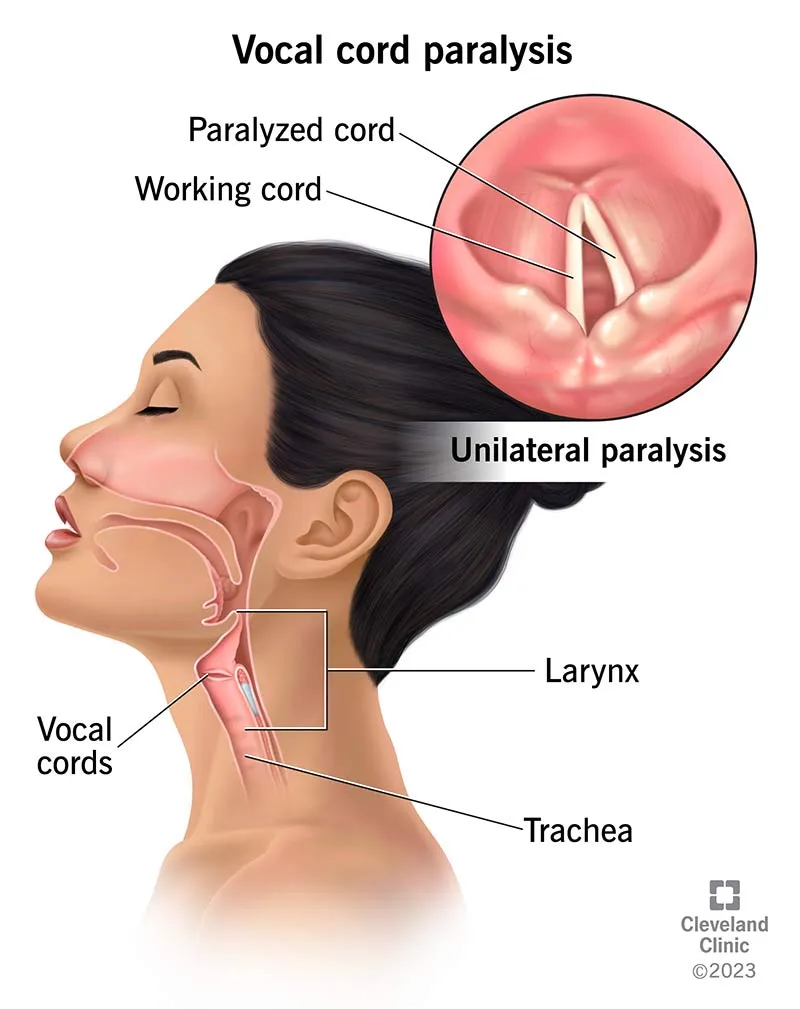
⭐ Unilateral RLN injury causes hoarseness (paramedian vocal cord). Bilateral injury causes acute airway obstruction (median vocal cords).
🗺️ Anatomy: Clinical Correlations - Danger Zones
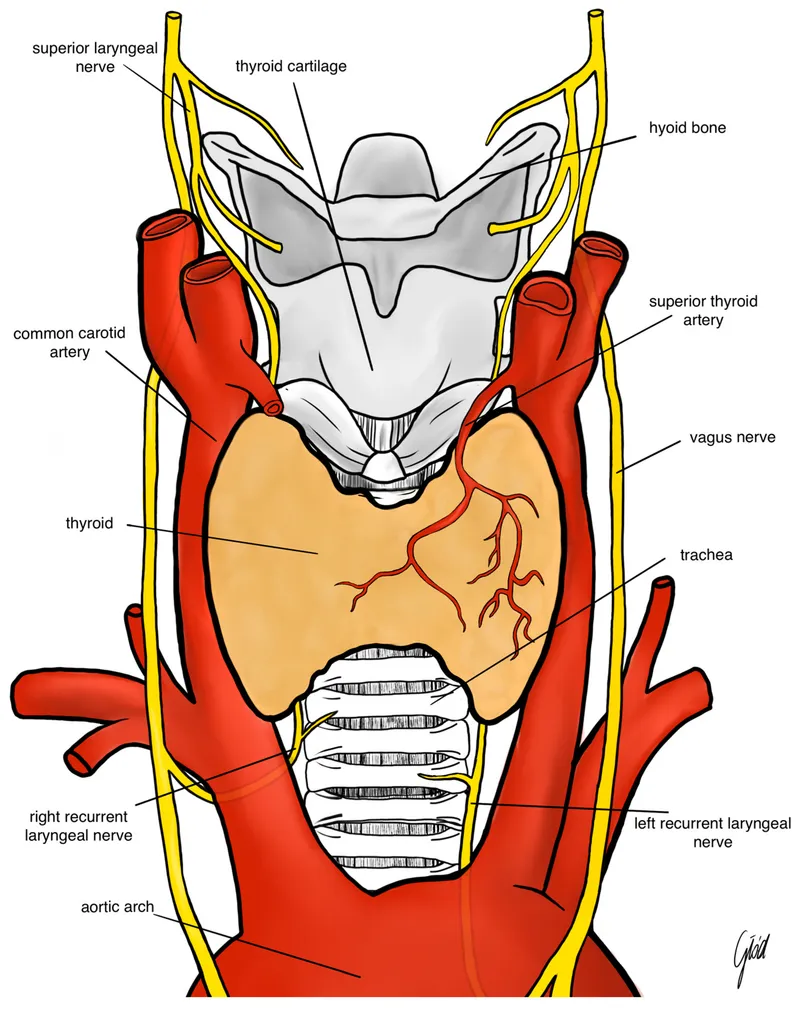
- Inferior Thyroid Artery (ITA) Crossing:
- RLN course is variable: posterior, anterior, or between ITA branches.
- ⚠️ Ligate ITA branches individually, close to the thyroid capsule, not the main trunk.
- Ligament of Berry:
- Fibrovascular band attaching thyroid to trachea.
- RLN passes deep or through it; high risk of injury during final gland mobilization.
- Tubercle of Zuckerkandl (ToZ):
- Posterolateral thyroid projection; often covers the RLN.
- 💡 A reliable landmark to identify the nerve.
⭐ Non-Recurrent Laryngeal Nerve (NRLN): A rare (~1%) anomaly, almost exclusively on the right, associated with an aberrant right subclavian artery (arteria lusoria).
🛡️ The Guardian's Playbook
- Pre-op: Baseline laryngoscopy for patients with pre-existing hoarseness, dysphonia, or history of prior neck surgery.
- Intra-op Gold Standard: Meticulous dissection and definitive visual identification ("see the nerve").
- Medial-to-lateral approach is common.
- Key landmarks: Inferior thyroid artery, Tracheoesophageal groove, Tubercle of Zuckerkandl, Ligament of Berry.
- Intraoperative Nerve Monitoring (IONM) aids localization and confirms functional integrity post-dissection.
- ⚠️ Avoid blind clamping, excessive traction, and thermal injury from electrocautery near the nerve.
⭐ Non-Recurrent Laryngeal Nerve (NRLN): A rare anomaly (~0.5-1%), almost exclusively on the right, associated with an aberrant right subclavian artery (arteria lusoria).
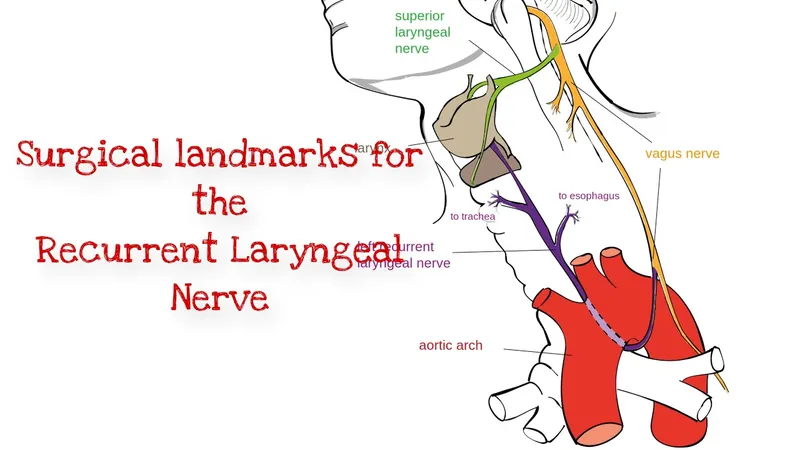
⚠️ Complications - The Aftermath
- Unilateral Injury:
- Presents with hoarseness, dysphonia, and a weak, breathy voice.
- Vocal cord assumes a paramedian position due to unopposed cricothyroid (SLN) action.
- Bilateral Injury:
- A surgical emergency presenting with acute stridor and respiratory distress.
- Both vocal cords are adducted (median position), causing severe airway obstruction.
- Requires immediate airway intervention (intubation/tracheostomy).
⭐ The posterior cricoarytenoid is the only vocal cord abductor. Its paralysis in bilateral RLN injury leads to unopposed adduction and airway closure.
⚡ Biggest Takeaways
- The recurrent laryngeal nerve (RLN), from the vagus nerve (CN X), is at risk during thyroidectomy; visual identification is key.
- Unilateral RLN injury causes hoarseness and a breathy voice due to ipsilateral vocal cord paralysis.
- Bilateral RLN injury is an emergency causing airway obstruction and stridor from paralyzed midline vocal cords.
- Superior Laryngeal Nerve (SLN) injury affects the cricothyroid muscle, causing loss of high-pitched sounds.
- A non-recurrent RLN is a rare anomaly, almost always on the right side.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

