🔬 Pathophysiology - Hormone Havoc Headquarters
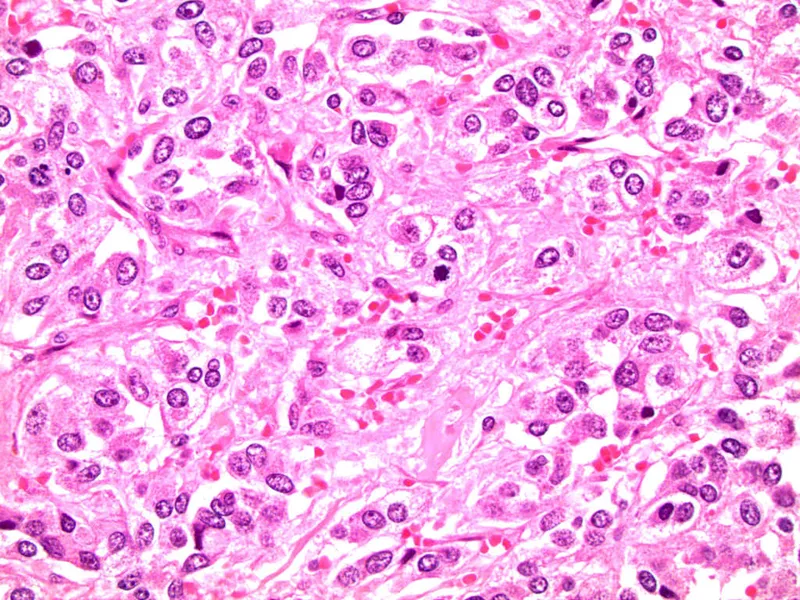
- Origin: Tumor of chromaffin cells (neuroectodermal crest origin) located in the adrenal medulla.
- Secretion: Produces, stores, and secretes catecholamines (norepinephrine, epinephrine) in an unregulated, episodic manner.
- Synthesis: Tyrosine → DOPA → Dopamine → Norepinephrine → Epinephrine.
- The final step, NE → Epi, is catalyzed by Phenylethanolamine-N-methyltransferase (PNMT).
- Metabolism: Catecholamines are degraded to metanephrines and vanillylmandelic acid (VMA), which are measured for diagnosis.
⭐ 📌 Rule of 10s: A classic mnemonic stating 10% of pheochromocytomas are:
- Malignant
- Bilateral
- Extra-adrenal
- In children
- Calcified
🚨 Clinical Manifestations - The Catecholamine Crisis
- Caused by episodic surges of catecholamines (epinephrine, norepinephrine), leading to paroxysmal symptoms.
- 📌 Classic Triad (PHEochromocytoma):
- Palpitations & Tachycardia
- Headache (severe, throbbing)
- Episodic sweating (profuse diaphoresis)
- Severe hypertension is the hallmark; can be sustained or paroxysmal and often resistant to standard therapy.
- Other symptoms include anxiety, panic attacks, tremor, pallor (vasoconstriction), and chest/abdominal pain.
- ⚠️ Triggers: Anesthesia induction, surgery, childbirth, certain drugs (e.g., TCAs, metoclopramide).
⭐ Catecholamine excess can cause severe, reversible LV dysfunction (catecholamine-induced cardiomyopathy), mimicking myocardial infarction or Takotsubo cardiomyopathy.
🔬 Diagnosis - Finding the Pheo
-
Biochemical Confirmation (Step 1):
- Best initial test: Plasma free metanephrines (Sensitivity >95%).
- Confirmatory: 24-hour urine for fractionated metanephrines & catecholamines.
- ⚠️ Avoid interfering meds (e.g., TCAs, levodopa, decongestants).
-
Localization (Step 2 - after biochemical proof):
- First-line: CT or MRI of abdomen/pelvis.
- If negative, extra-adrenal, or metastatic suspicion: Functional imaging (e.g., MIBG scan, Ga-DOTATATE PET/CT).
⭐ Clonidine Suppression Test: Used for borderline cases. In pheochromocytoma, autonomous tumor secretion means plasma catecholamines are NOT suppressed by clonidine (an α2-agonist).
💊 Management - Taming the Tumor
Pre-operative preparation is crucial to prevent intraoperative hypertensive crisis. The goal is to "tame" the tumor's catecholamine effects before resection.
- Pharmacologic Blockade:
- Step 1: α-Blockade (start 10-14 days pre-op)
- Phenoxybenzamine (irreversible, non-selective) is classic.
- Selective α1-blockers (Doxazosin, Prazosin) are alternatives with fewer side effects.
- Titrate to BP <130/80 mmHg seated, with mild orthostasis (systolic >90 mmHg standing).
- Step 2: β-Blockade (start 2-3 days after α-blockade)
- Add only AFTER adequate α-blockade to control reflex tachycardia.
- e.g., Propranolol, Metoprolol.
- Step 3: Volume Expansion
- Liberal salt intake and IV fluids to counteract catecholamine-induced volume contraction and prevent post-op hypotension.
- Step 1: α-Blockade (start 10-14 days pre-op)
⭐ Alpha-blockade FIRST, then Beta-blockade. Unopposed alpha-stimulation from beta-blockade alone (blocking vasodilatory β2 receptors) can lead to a life-threatening hypertensive crisis.
Pre-Op Blockade Sequence:
- Intra-operative:
- Hypertension: IV Nitroprusside, Phentolamine.
- Hypotension: After adrenal vein ligation, treat with fluids & pressors.
⚡ High-Yield Points - Biggest Takeaways
- Pre-op alpha-blockade (e.g., phenoxybenzamine) for 10-14 days is ESSENTIAL to prevent hypertensive crisis.
- Add beta-blockade ONLY AFTER adequate alpha-blockade to avoid unopposed alpha-stimulation and hypertensive crisis.
- Liberal IV fluids are required pre-op to expand volume and prevent post-resection hypotension.
- Manage intra-op hypertension with short-acting agents like nitroprusside or phentolamine.
- Anticipate post-op hypotension from catecholamine withdrawal; treat with fluids/pressors.
- Screen for associated syndromes: MEN 2A/2B, VHL, NF1.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

