🗺️ Anatomy - Where are those Glands?
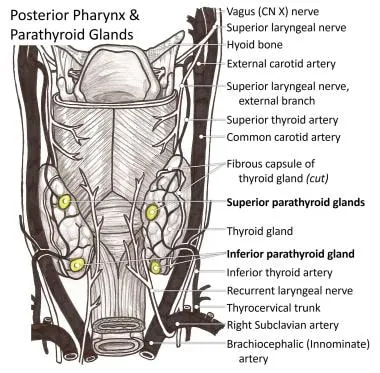
- General: Typically 4 small, ovoid, tan-colored glands on the posterior surface of the thyroid.
- Blood Supply: Primarily from the Inferior Thyroid Artery (ITA).
- Embryology & Location:
- Superior Glands (4th pouch): More constant. Posterior to the Recurrent Laryngeal Nerve (RLN), near the cricothyroid junction.
- Inferior Glands (3rd pouch): More variable due to descent with the thymus. Usually anterior to the RLN, near the lower thyroid pole.
- 📌 Mnemonic: Inferior glands from pouch 3 follow the Thymus.
⭐ Surgical Pearl: The relationship to the RLN is a critical landmark. Superior glands are typically posterior to the nerve, while inferior glands are anterior.
- Ectopic Glands: More common for inferior glands. Locations: mediastinum (thymus), retroesophageal, carotid sheath, intrathyroidal.
🩺 Diagnosis - Calcium Chaos Crew
-
Biochemical Confirmation:
- Initial finding: Persistent ↑ Serum Calcium.
- Key diagnostic test: ↑ PTH level (or inappropriately normal for the calcium level).
- Associated labs: ↓ serum phosphate, ↑ alkaline phosphatase.
- 📌 Differentiate from Familial Hypocalciuric Hypercalcemia (FHH) with a 24-hour urine calcium. FHH has ↓ urine calcium; surgery is not indicated.
-
Localization Studies (Finding the Gland):
- 1st Line: Sestamibi scan (Technetium-99m) and high-resolution neck Ultrasound are complementary.
- 2nd Line: 4D-CT or MRI for equivocal/negative initial scans or re-operative cases.
⭐ Surgical indications for asymptomatic primary hyperparathyroidism: Age < 50, Serum Ca²⁺ > 1 mg/dL above normal, T-score ≤ -2.5 (osteoporosis), vertebral fracture, or CrCl < 60 mL/min.
🔪 Management - The Gland Heist
-
Goal: Excise hyperfunctioning gland(s) while preserving normal tissue and avoiding complications. Pre-operative localization (Sestamibi, US) guides the approach.
-
Intraoperative PTH (ioPTH) Monitoring:
- Miami Criterion: >50% drop in PTH from the highest pre-excision level 10 minutes post-resection.
- Confirms successful removal: $PTH_{10min} < 0.5 \times PTH_{baseline}$
⭐ Failed parathyroidectomy? Suspect a missed ectopic gland. Common locations: mediastinum, retroesophageal, intrathyroidal, or within the carotid sheath.
- Complications:
- ⚠️ Hypocalcemia: Most common (hungry bone syndrome, hypoparathyroidism).
- Recurrent Laryngeal Nerve Injury: Hoarseness.
- Hematoma: Potential airway compromise.
⚠️ Complications - Post-Op Perils
- Hypocalcemia (Most Common):
- Causes: Hungry Bone Syndrome (severe pre-op bone disease), iatrogenic hypoparathyroidism.
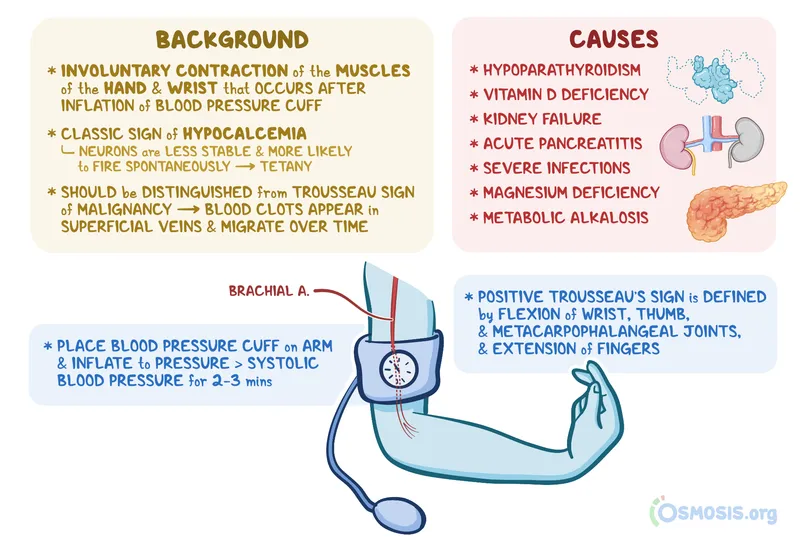
- Symptoms: Perioral numbness, paresthesias, Chvostek's/Trousseau's signs, tetany.
- Tx: Oral Ca$^{2+}$ & calcitriol. Severe/symptomatic: IV Calcium Gluconate.
- Recurrent Laryngeal Nerve (RLN) Injury:
- Unilateral: Hoarseness, breathy voice.
- Bilateral (⚠️ Airway Emergency): Stridor, respiratory distress.
- Neck Hematoma:
- Can cause rapid airway compression.
- Requires immediate bedside incision & drainage.
⭐ Hungry Bone Syndrome: Profound, prolonged hypocalcemia with hypophosphatemia post-op. Occurs in patients with severe pre-op hyperparathyroidism (e.g., osteitis fibrosa cystica) due to rapid bone remineralization.
⚡ High-Yield Points - Biggest Takeaways
- Primary hyperparathyroidism is the main indication; surgery is for symptomatic or severe asymptomatic disease.
- Sestamibi scan and ultrasound are key for pre-op localization to guide minimally invasive parathyroidectomy (MIP).
- A >50% drop in intraoperative PTH from baseline confirms successful resection.
- Key risks: recurrent laryngeal nerve injury (hoarseness) and severe post-op hypocalcemia ("hungry bone syndrome").
- In MEN1/2A, suspect multiglandular disease, often requiring subtotal parathyroidectomy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

