👶 Management - Little Lungs, Big Challenges
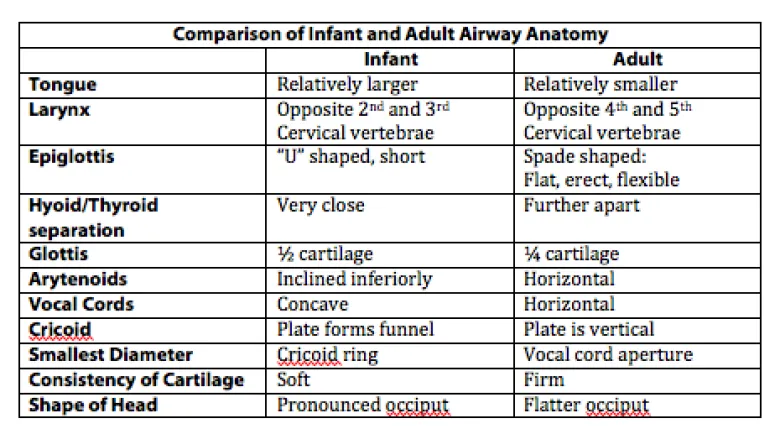
- Airway Anatomy:
- Large occiput & tongue, anterior/cephalad larynx (C3-C4).
- Epiglottis is long & floppy (omega-shaped).
- Narrowest point: cricoid cartilage (funnel-shaped).
- Physiology:
- Respiratory: ↑ O₂ consumption, ↓ Functional Residual Capacity (FRC) → rapid O₂ desaturation.
- Cardiovascular: Cardiac output is heart rate-dependent.
- Pharmacology: ↑ Volume of distribution for hydrophilic drugs; ↑ Minimum Alveolar Concentration (MAC) for volatile anesthetics (except neonates).
- Management:
- 📌 Uncuffed ETT size: $(Age/4) + 4$.
- Fluids: Use isotonic solutions (e.g., LR).
⭐ Bradycardia in a pediatric patient during anesthesia is a sign of hypoxia until proven otherwise. The primary response is to ensure adequate oxygenation and ventilation.
👐 Management - Handle With Care
- Pediatrics: ↑ risk of laryngospasm. Faster inhalation induction due to ↑ alveolar ventilation/FRC ratio. Precise, weight-based dosing is critical.
- Geriatrics: ↓ MAC requirements. Slower circulation time delays IV drug onset. ↑ risk of postoperative cognitive dysfunction (POCD). 📌 Start low, go slow.
- Obstetrics: Aortocaval compression requires left uterine displacement. ↑ aspiration risk may necessitate rapid sequence intubation (RSI).
- Obesity (BMI > 30): Anticipate difficult airway. ↑ risk of OSA and VTE. Drug dosing adjusted (ideal vs. total body weight).
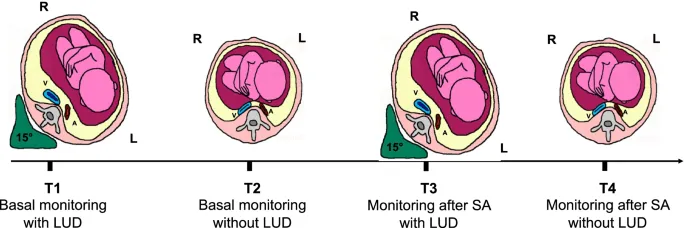
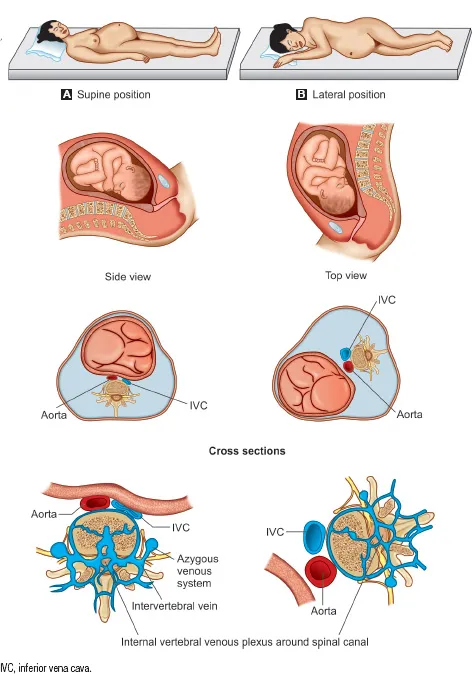
⭐ In pregnant patients, aortocaval compression by the gravid uterus can cause significant hypotension, especially in the supine position. Always use left uterine displacement after 20 weeks gestation.
🤰 Management - Two Patients, One Plan
- Maternal Changes & Implications:
- Resp: ↓FRC, ↑O₂ consumption → rapid desaturation. Airway edema → difficult intubation.
- CV: Aortocaval compression → supine hypotension. Prevent with left uterine displacement (LUD).
- GI: ↑Aspiration risk → give sodium citrate.
- Anesthetic: ↓MAC by 40%, ↑sensitivity to neuraxial block.
- Anesthesia for Cesarean Delivery:
- Neuraxial (Spinal/Epidural): Preferred for most cases.
- Pros: Awake mother, minimal fetal drug exposure.
- Cons: Hypotension (treat with phenylephrine).
- General Anesthesia (GA): For emergent cases or contraindications.
- Requires Rapid Sequence Intubation (RSI).
- Neuraxial (Spinal/Epidural): Preferred for most cases.
⭐ Most anesthetics cross the placenta. Exceptions: Glycopyrrolate, Succinylcholine, Heparin (highly ionized/large).
⚖️ Management - A Weighty Matter
- Airway & Respiratory:
- High risk of difficult mask ventilation/intubation & Obstructive Sleep Apnea (OSA).
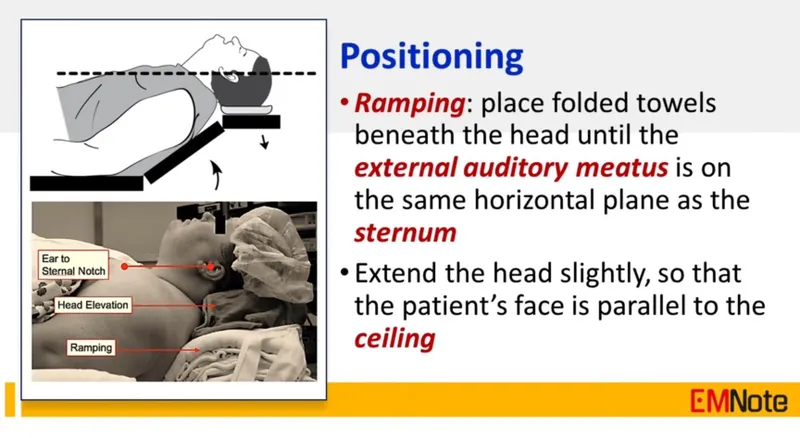
- Use ramped position ("ear-to-sternal-notch") for airway alignment.
- ↓ Functional Residual Capacity (FRC) → rapid O₂ desaturation.
- Pharmacokinetics & Dosing:
- Induction (Propofol): Lean Body Weight (LBW).
- Opioids (Fentanyl): LBW.
- Neuromuscular Blockers (NMBs):
- Succinylcholine: Total Body Weight (TBW).
- Rocuronium/Vecuronium: Ideal Body Weight (IBW).
- 📌 IBW (Devine): Men: $50\text{kg} + 2.3\text{kg}$ per inch > 5 ft.
⭐ Obese patients have a significantly reduced FRC, leading to rapid desaturation during apnea. Effective pre-oxygenation and denitrogenation are critical.
⚡ Biggest Takeaways
- Geriatric patients: ↓ MAC, ↓ organ reserve, slower drug clearance, and ↑ risk of postoperative delirium.
- Pediatric patients: ↑ MAC, faster induction/emergence, and high risk for laryngospasm and bradycardia.
- Pregnant patients: ↓ MAC and ↑ aspiration risk. Prevent aortocaval compression with left uterine displacement.
- Obese patients: Difficult airway, risk of OSA/hypoventilation. Dose some drugs based on lean body weight.
- Malignant Hyperthermia: Triggered by volatile anesthetics/succinylcholine; treat with dantrolene.
- Renal/Hepatic Disease: Requires dose adjustment due to altered drug metabolism/excretion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

