Alcohol Withdrawal - Shakes, Seizures, & DTs
- Clinical Timeline: Symptom onset after last drink.
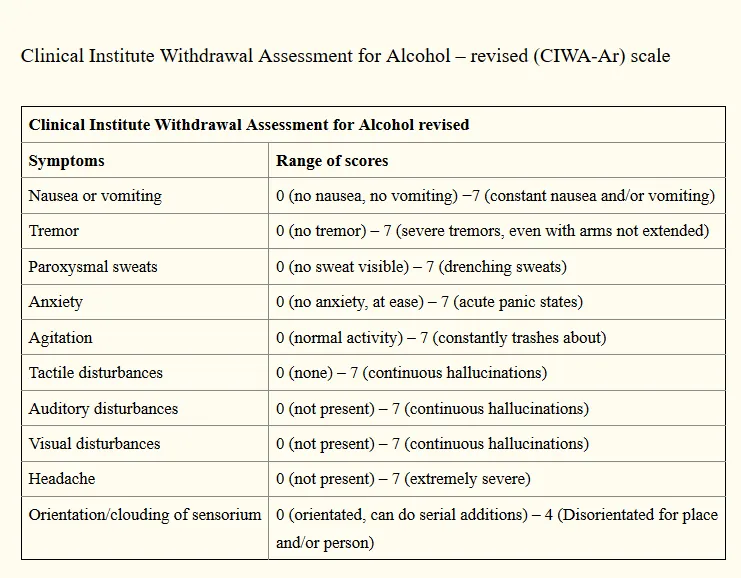
- Assessment: Use CIWA-Ar scale to guide therapy.
- Score > 15 indicates severe withdrawal requiring medication.
- Management Protocol:
- Benzodiazepines: First-line treatment (e.g., Chlordiazepoxide, Diazepam, Lorazepam). Titrate dose to CIWA-Ar score.
- Thiamine (Vitamin B1): Administer 100mg IV/IM before glucose to prevent Wernicke-Korsakoff syndrome.
⭐ In patients with liver failure/cirrhosis, use Lorazepam, Oxazepam, or Temazepam (LOT) as they undergo glucuronidation without forming active metabolites.
Opioid Withdrawal - The Unbearable Flu
- Presentation: Resembles a severe flu. Onset varies by opioid half-life (e.g., heroin: 6-12h; methadone: 24-48h).
- Symptoms: Dysphoria, myalgia, nausea/vomiting/diarrhea.
- Autonomic signs: Lacrimation, rhinorrhea, yawning, piloerection ("cold turkey").
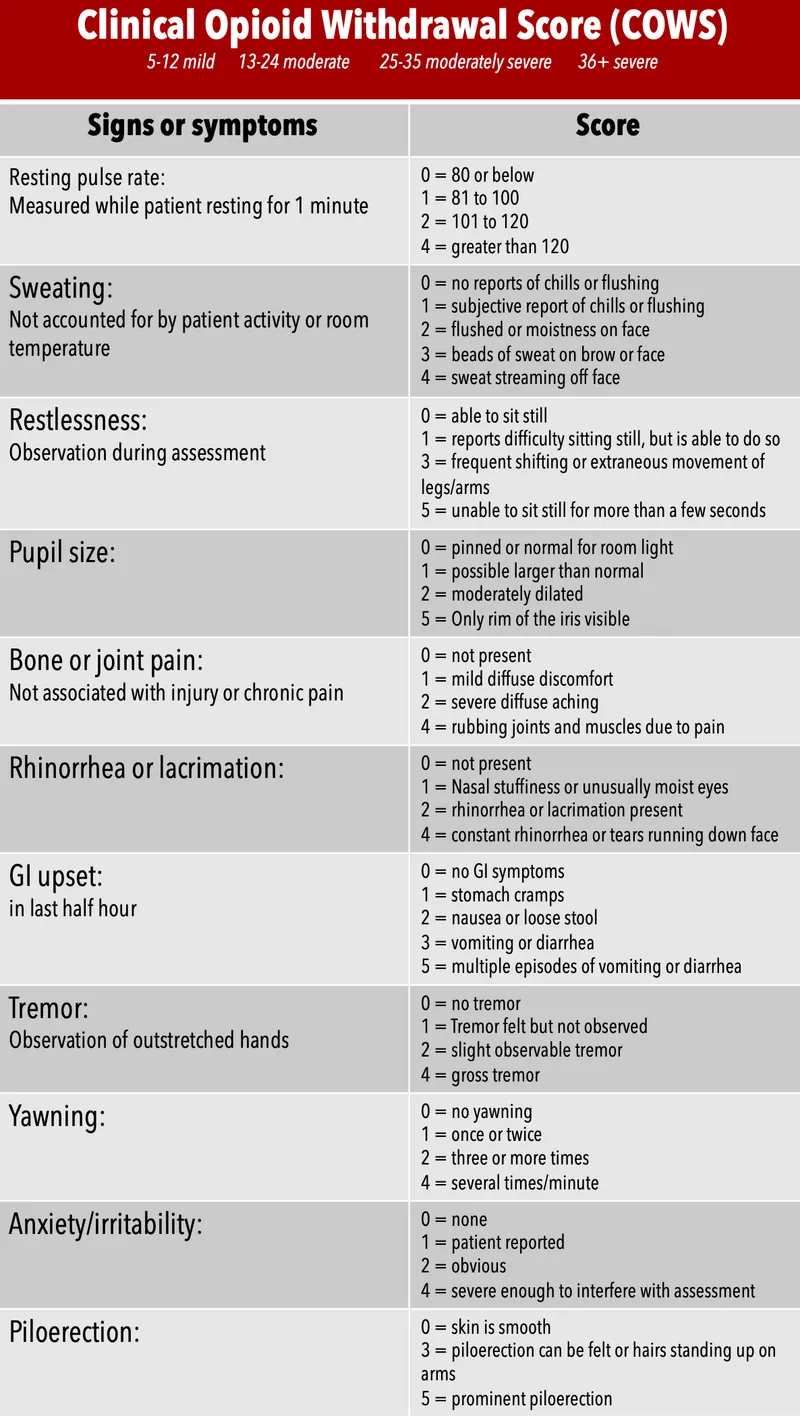
- Assessment: Clinical Opioid Withdrawal Scale (COWS). Treatment indicated for moderate-to-severe withdrawal (COWS > 12).
- Management:
- Agonist replacement: Methadone (long-acting) or Buprenorphine (partial agonist).
- Symptomatic control: Clonidine (α2-agonist) for autonomic hyperactivity; loperamide for diarrhea, ondansetron for nausea.
⭐ High-Yield: Buprenorphine can precipitate withdrawal if given to a patient not yet in withdrawal, due to its high receptor affinity but lower intrinsic activity, displacing other opioids.
Sedative-Hypnotic Withdrawal - The Taper Imperative
- Causative Agents: Primarily Benzodiazepines (e.g., alprazolam, lorazepam) and Barbiturates.
- Clinical Features: A life-threatening emergency. Presents with anxiety, insomnia, perceptual disturbances, and autonomic hyperactivity (↑tachycardia, ↑hypertension). Severe cases can progress to generalized seizures and psychosis.
- Management: The core principle is a gradual taper to prevent seizures.
⭐ Abrupt cessation, especially of short-acting benzodiazepines, poses the highest risk for severe withdrawal, including refractory seizures.
Stimulant Withdrawal - The Depressive Crash
- Substances: Cocaine, amphetamines.
- Clinical Picture (The "Crash"): A distinct dysphoric period following cessation of use.
- Symptoms: Severe depression, anhedonia, fatigue, hypersomnia, increased appetite (hyperphagia), and intense craving.
- Patients may also experience vivid and unpleasant dreams.
- Management: Primarily supportive care.
- There are no FDA-approved medications for stimulant withdrawal.
- ⚠️ Crucial: Monitor for suicidality risk, which can be significant during the crash phase.
⭐ While not typically medically dangerous, the primary risk in stimulant withdrawal is suicide due to the severe depressive symptoms.
High‑Yield Points - ⚡ Biggest Takeaways
- Alcohol withdrawal: Manage with benzodiazepines (e.g., lorazepam, chlordiazepoxide) to prevent life-threatening seizures and delirium tremens.
- Opioid withdrawal: Treat flu-like symptoms and autonomic hyperactivity with supportive care, clonidine, or opioid agonists like buprenorphine.
- Benzodiazepine withdrawal: Requires a slow taper of a long-acting agent to prevent potentially fatal seizures.
- Stimulant withdrawal: Characterized by a dysphoric "crash" with severe depression and fatigue; management is supportive.
- Delirium tremens: A medical emergency 48-96 hours post-alcohol; treat aggressively with IV benzodiazepines.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

