Stimulants 101 - The Fast Lane
-
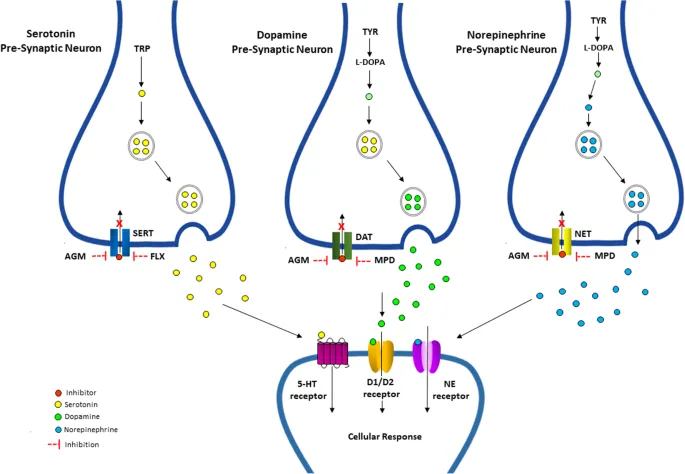
Core Mechanism: Primarily block reuptake of key monoamines, leading to ↑ synaptic levels.
- Dopamine (DA): Central to reward, motivation, and addiction.
- Norepinephrine (NE): Mediates sympathomimetic effects (↑ heart rate, blood pressure).
- Serotonin (5-HT): Influences mood and perception.
-
Key Agents & Nuances:
- Cocaine: Pure reuptake inhibitor (DA > NE > 5-HT).
- Amphetamines: Inhibit reuptake AND enhance presynaptic release of DA and NE.
- MDMA (Ecstasy): Similar to amphetamines but with greater 5-HT effects.
⭐ Cocaine is unique among stimulants for its additional local anesthetic and potent vasoconstrictive effects, achieved by blocking sodium channels. This vasoconstriction can lead to myocardial infarction and nasal septal perforation.
Clinical Picture - Highs and Crashes
| Intoxication ("High") | Withdrawal ("Crash") |
|---|---|
| Psychiatric: * Euphoria, grandiosity * Psychomotor agitation * Anxiety, paranoia, psychosis * Tactile hallucinations (e.g., "cocaine bugs") | Psychiatric: * Severe depression ("crash") * Anhedonia, dysphoria * Suicidal ideation * Intense craving |
| Physical: * Sympathetic overdrive: ↑ HR, ↑ BP * Mydriasis (pupil dilation) * Diaphoresis, hyperthermia * Seizures, cardiac arrhythmias | Physical: * Fatigue, lethargy * Hypersomnia, vivid dreams * Increased appetite * Psychomotor retardation |
Complications - The Body Under Siege
-
Cardiovascular:
- Acute Coronary Syndrome (vasospasm-induced MI).
- Aortic Dissection (from severe hypertension).
- Chronic use → Dilated Cardiomyopathy.
- Tachyarrhythmias, sudden cardiac death.
-
Neurological:
- Stroke (ischemic & hemorrhagic).
- Seizures (lowered threshold).
- Severe hyperthermia → rhabdomyolysis.
-
Psychiatric:
- Psychosis: Paranoid delusions, hallucinations (visual, tactile).
- Formication: Sensation of insects crawling on skin.
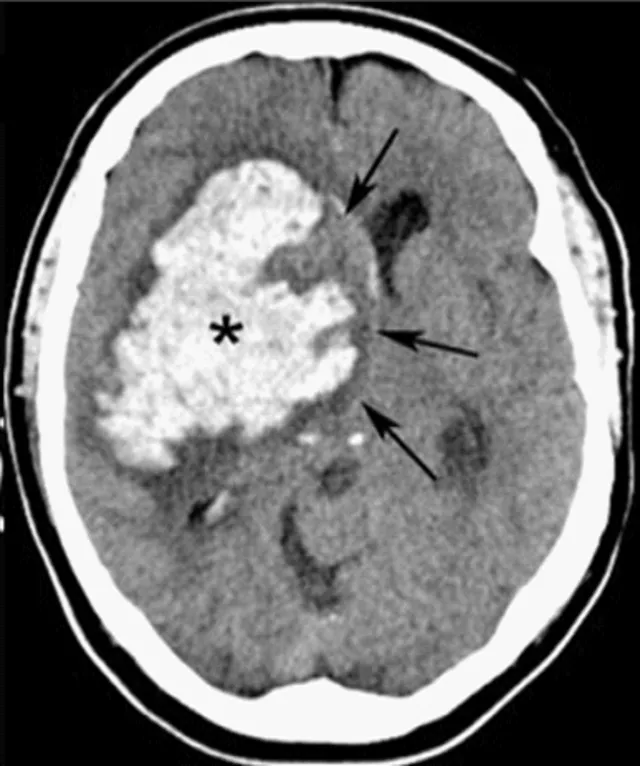
⭐ In stimulant-induced chest pain, avoid isolated beta-blockers. This can cause unopposed alpha-stimulation, worsening coronary vasospasm. Prioritize benzodiazepines.
Management - The Intervention Playbook
-
Acute Intoxication: Primarily supportive and symptom-directed.
- Agitation/Psychosis: Benzodiazepines (e.g., lorazepam).
- Hyperthermia (>40°C / 104°F): Rapid cooling measures.
- Severe Hypertension: Phentolamine, nitroprusside.
- Avoid pure beta-blockers (risk of unopposed alpha-stimulation).
-
Withdrawal: Supportive care is the mainstay.
- Focus on monitoring for depression and suicidal ideation.
-
Long-Term Treatment: Psychosocial interventions are first-line.
- Cognitive-Behavioral Therapy (CBT): Develops coping skills.
- Contingency Management: Uses motivational incentives (vouchers, prizes) to promote abstinence.
⭐ There are currently no FDA-approved medications for the treatment of stimulant use disorder. Management relies heavily on psychosocial support and symptomatic treatment.
High-Yield Points - ⚡ Biggest Takeaways
- Stimulant intoxication mimics sympathetic overdrive: ↑ HR, ↑ BP, mydriasis, agitation, and potential for cardiac ischemia or seizures.
- Withdrawal presents as a "crash" with severe depression, hypersomnia, fatigue, and intense craving.
- Manage acute intoxication with benzodiazepines; avoid beta-blockers in cocaine toxicity due to risk of unopposed alpha-stimulation.
- Chronic use can cause dilated cardiomyopathy, psychosis with tactile hallucinations (formication), and severe dental caries ("meth mouth").
- The core mechanism is ↑ dopamine in the synaptic cleft.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

