Restless Legs Syndrome (RLS) - Jumping Beans at Bedtime
-
Core Feature: An irresistible urge to move the legs, often with uncomfortable crawling, pulling, or creeping sensations.
-
Diagnostic Criteria (📌 Mnemonic: URGE):
- Urge to move legs.
- Rest-induced (symptoms worsen with inactivity).
- Gets better with movement.
- Evening or nighttime worsening (circadian pattern).
-
Key Associations & Secondary Causes:
- Iron deficiency (check ferritin!).
- Uremia (ESRD), pregnancy, diabetes.
- Medications: Antidepressants, antipsychotics, antihistamines.
-
Management:
- Treat underlying cause; supplement iron if ferritin < 75 ng/mL.
- First-line: Dopamine agonists (Pramipexole, Ropinirole).
- Alternatives: Alpha-2-delta ligands (Gabapentin, Pregabalin).
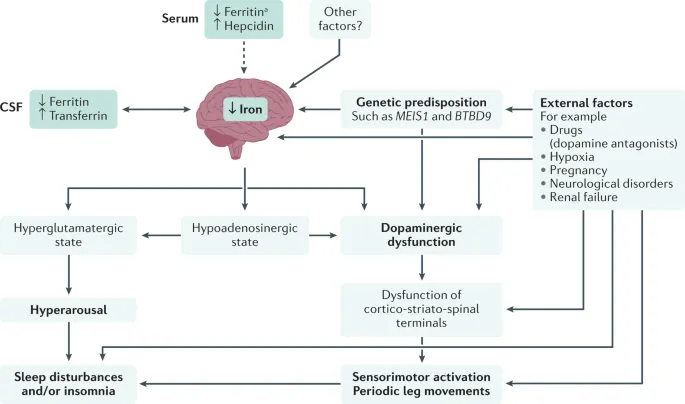
⭐ High-Yield: The link between RLS and iron deficiency is frequently tested. Low CNS iron is a primary hypothesis for RLS pathophysiology, making ferritin level a crucial initial lab test.
Periodic Limb Movement Disorder (PLMD) - Night Kicks Unchained
- What: Repetitive, stereotyped limb movements (typically leg dorsiflexion, "night kicks") occurring primarily during NREM sleep. Patients are usually unaware of the movements themselves.
- Clinical Picture: Presents as excessive daytime sleepiness, frequent nocturnal awakenings, or insomnia due to sleep fragmentation. Often first reported by a bed partner.
- Diagnosis: Polysomnography (PSG) is the definitive diagnostic tool.
- Diagnostic threshold: PLM index (PLMI) ≥ 15 movements/hour in adults.
- Associations: Strong overlap with Restless Legs Syndrome (RLS), but can occur independently. Also check for iron deficiency, uremia, and medication side effects (e.g., SSRIs, TCAs).
- Management:
- Treat underlying conditions (e.g., iron supplementation).
- First-line agents: Dopamine agonists (Pramipexole, Ropinirole).
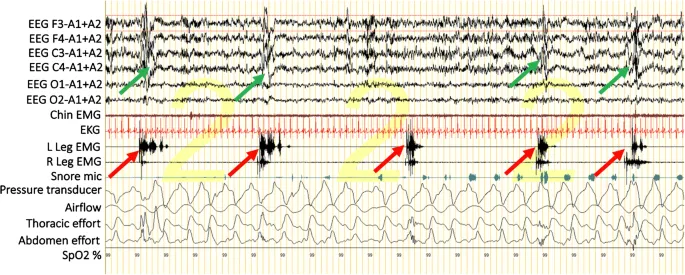
⭐ High-Yield: PLMD is a polysomnographic diagnosis, not a clinical one. Unlike RLS, the urge to move is absent, and the movements occur during sleep, not while awake. The primary complaint is non-restorative sleep, not the movements themselves.
Other Movement Disorders - The Night Shift Grind
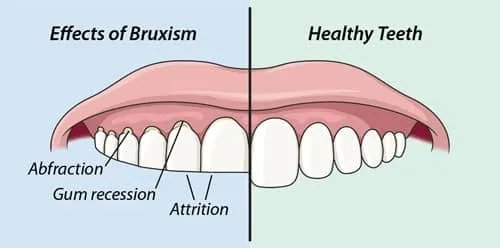
- Bruxism (Teeth Grinding):
- Involuntary, forceful clenching or grinding of teeth, primarily during sleep.
- Associated with stress, anxiety, obstructive sleep apnea (OSA), and medications.
- Leads to jaw pain (TMD), morning headaches, and significant tooth wear.
- Management: Custom dental guards, stress reduction, treating associated OSA.
⭐ SSRI-Associated Bruxism: A notable side effect, particularly with fluoxetine. May require dose adjustment, switching the agent, or adding buspirone.
- Rhythmic Movement Disorder (RMD):
- Repetitive, stereotyped movements involving large muscle groups, often at sleep onset (e.g., head banging, body rocking).
- Primarily a disorder of infancy/childhood; typically benign and self-limited.
High‑Yield Points - ⚡ Biggest Takeaways
- Restless Legs Syndrome (RLS) is a clinical diagnosis characterized by an irresistible urge to move the legs, which is worse at night and relieved by movement.
- Always evaluate for iron deficiency anemia (check ferritin), a key secondary cause of RLS.
- First-line pharmacotherapy includes dopamine agonists (pramipexole, ropinirole) or gabapentin.
- Periodic Limb Movement Disorder (PLMD) involves stereotyped limb jerks during sleep, diagnosed via polysomnography.
- Unlike the clinical diagnosis of RLS, PLMD is a polysomnographic finding.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

