Comorbidity Overview - The Double Trouble Diagnosis
- Personality Disorders (PDs) frequently co-occur with Axis I disorders (e.g., MDD, Anxiety), complicating diagnosis and worsening prognosis. This dual diagnosis often leads to greater functional impairment and treatment resistance.
- Common Pairings:
- Borderline PD: Mood & Substance Use Disorders.
- Avoidant PD: Anxiety Disorders.
- Antisocial PD: Substance Use & Impulse Control Disorders.
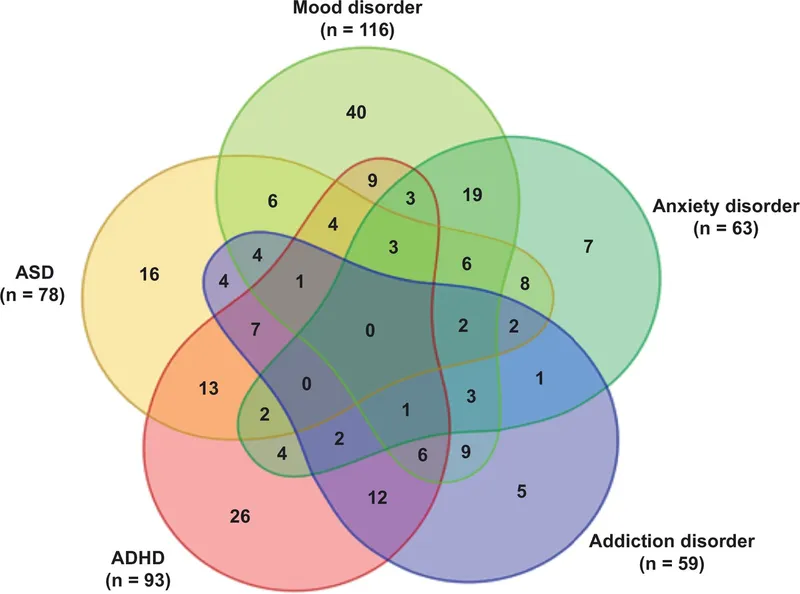
⭐ The presence of a PD significantly reduces the efficacy of standard treatments for the co-occurring Axis I disorder, requiring an integrated treatment approach.
Cluster A Comorbidities - The Weird & The Worrisome
- Paranoid PD: ↑ risk for Delusional Disorder (Persecutory Type) & Agoraphobia. Chronic stress can trigger brief psychotic episodes.
- Schizoid PD: Significant overlap with Major Depressive Disorder & Social Anxiety Disorder. Often lacks desire for relationships, distinguishing it from Avoidant PD.
- Schizotypal PD: Strongest link to Schizophrenia; considered a "schizophrenia-spectrum" disorder.
- High risk for developing Brief Psychotic Episodes, Schizophreniform Disorder, or Schizophrenia.
⭐ Up to 50% of patients with Schizotypal PD have had at least one episode of Major Depressive Disorder.
Cluster B Comorbidities - The Wild & The Woeful
- Antisocial (ASPD): High rates of Substance Use Disorders (SUDs), especially alcohol. Also strongly linked to Impulse Control Disorders (e.g., gambling).
- Borderline (BPD): The most comorbid personality disorder. Overlaps significantly with Mood Disorders (MDD, Bipolar), Anxiety Disorders, PTSD, SUDs, and Eating Disorders (especially Bulimia Nervosa).
- Histrionic (HPD): Frequently co-occurs with Somatic Symptom Disorder, Conversion Disorder, and Mood Disorders.
- Narcissistic (NPD): Associated with SUDs (cocaine), depressive episodes following "narcissistic injury," and anxiety. Anorexia Nervosa can also be a comorbidity.
⭐ Exam Favorite: Over 85% of patients with Borderline Personality Disorder have at least one other co-existing psychiatric diagnosis, most commonly a mood disorder.
Cluster C Comorbidities - The Anxious & The Apprehensive
- Avoidant PD: Marked overlap with Social Anxiety Disorder (often seen as a severe variant). High rates of comorbid Major Depressive Disorder (MDD) and other anxiety disorders like Panic Disorder due to persistent feelings of inadequacy.
- Dependent PD: Frequently diagnosed with MDD, Generalized Anxiety Disorder (GAD), and Panic Disorder. Highly susceptible to developing an Adjustment Disorder, especially when a core supportive relationship is lost.
- Obsessive-Compulsive PD (OCPD): Linked with Anxiety Disorders (esp. GAD) and Mood Disorders. Distinct from OCD, but they can co-exist. Shares traits of perfectionism and control with Anorexia Nervosa.
⭐ Patients with Avoidant PD deeply desire social connection but are paralyzed by fear of rejection, a key feature distinguishing them from the socially indifferent Schizoid PD.
Clinical Implications - Managing the Maelstrom
- Personality disorders (PDs) worsen Axis I prognosis: ↑ symptom severity, ↑ relapse rates, and ↓ treatment adherence.
- Management requires treating both disorders concurrently, not sequentially.
- Prioritize stabilizing acute Axis I crises (e.g., suicidality, psychosis) first.
- Psychotherapy (e.g., DBT, CBT) is the cornerstone for the PD, while pharmacotherapy targets Axis I symptoms.
⭐ Borderline Personality Disorder has the highest comorbidity with other psychiatric disorders, especially mood, anxiety, and substance use disorders, which significantly increases suicide risk.
High‑Yield Points - ⚡ Biggest Takeaways
- Cluster A disorders are linked to psychotic disorders; schizotypal PD has strong genetic ties to schizophrenia.
- Cluster B disorders are highly comorbid with mood disorders, substance use, and anxiety.
- Borderline PD frequently co-occurs with MDD, PTSD, and substance use disorders.
- Antisocial PD is strongly associated with substance use and impulse-control disorders.
- Cluster C disorders are most commonly seen with anxiety disorders (e.g., Avoidant PD and social anxiety).
- A co-occurring personality disorder often worsens the prognosis of the Axis I disorder.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

