Core Challenges - Diagnostic Headaches
-
Ego-syntonic Nature: Patients perceive their behaviors and traits as normal and appropriate ("it's just who I am"). This leads to poor insight and makes them unlikely to seek help voluntarily.
-
Longitudinal History: Diagnosis requires establishing a pervasive, inflexible pattern of behavior over years, not from a single clinical interview. Diagnosis is deferred until after age 18.
-
Collateral Information: Crucial for an objective assessment. Patient self-reporting can be unreliable; input from family, friends, or past medical records is often necessary to confirm long-standing patterns.
⭐ Overlapping diagnostic criteria between different personality disorders are common, complicating a single, clear diagnosis and often leading to "not otherwise specified" (NOS) classifications.
Differential Diagnosis - Separating the Syndromes
High comorbidity and symptom overlap make differentiation critical. The core challenge is separating chronic, pervasive personality patterns from episodic syndromes or more circumscribed anxiety.
| Disorder | Key Differentiator | vs. | Counterpart | Key Differentiator |
|---|---|---|---|---|
| Borderline PD | Mood shifts are rapid, transient, and reactive to interpersonal stressors. Chronic emptiness; identity disturbance. | vs. | Bipolar Disorder | Mood episodes (mania, depression) are sustained (days to weeks) and more autonomous. |
| Schizotypal PD | Magical thinking, perceptual distortions, and eccentricity without frank, persistent psychosis. | vs. | Schizophrenia | Frank, persistent psychosis (delusions, hallucinations) and more severe functional decline. |
| Avoidant PD | Pervasive, lifelong social inhibition due to feelings of inadequacy. Desires relationships but fears rejection. | vs. | Social Anxiety | Fear is often specific to performance or social situations, not necessarily pervasive across all life domains. |
Assessment Toolkit - Instruments and Influences
- Structured Clinical Interviews: Gold standard for diagnostic accuracy.
- Structured Clinical Interview for DSM-5 (SCID-5-PD): Semi-structured, investigator-based. Ensures systematic coverage of criteria.
- Self-Report Inventories: Provide valuable collateral information but are susceptible to patient bias.
- Minnesota Multiphasic Personality Inventory (MMPI): Assesses personality traits and psychopathology.
- Clinician-Related Factors:
- Countertransference: Clinician's emotional reaction to the patient can distort judgment. Awareness is key.
- Cultural Sensitivity: Norms of behavior vary across cultures; what seems "disordered" may be culturally syntonic.
- ⚠️ Iatrogenic Harm: Mislabeling can lead to stigma and inappropriate treatment.
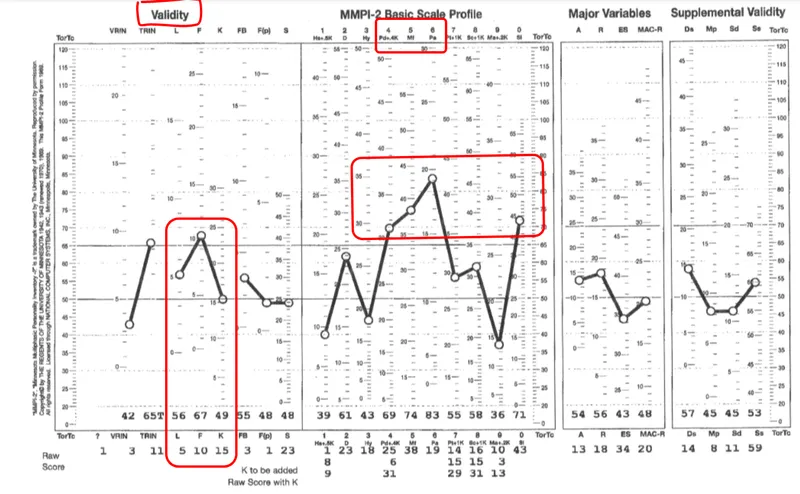
⭐ High-Yield Fact: The MMPI contains validity scales (e.g., L, F, K) to detect dishonest or random responding, crucial in personality disorders where impression management is common.
High-Yield Points - ⚡ Biggest Takeaways
- Overlapping criteria across different personality disorders frequently complicate a single, clear diagnosis.
- Patients often exhibit poor insight (ego-syntonic symptoms), viewing their behavior as normal.
- Co-occurring psychiatric disorders, like depression or substance use, can obscure the underlying personality structure.
- Diagnosis requires a longitudinal history to assess enduring patterns, not just a cross-sectional view.
- Clinician's countertransference can be a major diagnostic obstacle, clouding objective assessment.
- Cultural and social norms must be considered to avoid misinterpreting culturally syntonic behaviors.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

