LSDs Overview - Tiny Trash Troubles
- Definition: Group of ~70 inherited metabolic disorders. Caused by defects in lysosomal enzymes or essential proteins, leading to lysosomal dysfunction.
- Pathophysiology: Specific enzyme deficiency → progressive accumulation of undigested macromolecules (e.g., sphingolipids, mucopolysaccharides, glycogen) within lysosomes → cellular engorgement, organomegaly, and widespread systemic damage.
- Inheritance: Mostly Autosomal Recessive (AR).
⭐ Most LSDs are Autosomal Recessive. Notable X-linked Recessive exceptions include Fabry Disease and Hunter Syndrome (MPS II).
MPS Disorders - Sugar Storage Saga
| MPS Type | Enzyme Def. | Accum. GAG(s) | Features | Inh. |
|---|---|---|---|---|
| IH | α-L-iduronidase | H, D $SO_4$ | Coarse facies, cornea, dysostosis, CNS↓ | AR |
| II | Iduronate sulfatase | H, D $SO_4$ | Coarse facies, NO cornea, dysostosis, aggression | XR |
| III | Heparan N-sulfatase | H $SO_4$ | Severe CNS↓, mild somatic | AR |
| IV | Gal-6-sulfatase | K, C-6 $SO_4$ | Skeletal (short trunk), normal IQ, cornea | AR |
| VI | Arylsulfatase B | D $SO_4$ | Coarse facies, cornea, dysostosis, normal IQ | AR |
| VII | β-glucuronidase | H, D, C $SO_4$ | Variable: hydrops, HSM, dysostosis | AR |
⭐ Hunter (MPS II): X-linked, NO corneal clouding (vs Hurler).
Sphingolipidoses - Fatty Brain Breakdown
| Disease | Enzyme Deficient | Accumulated Substrate | Key Features | Inheritance |
|---|---|---|---|---|
| Tay-Sachs | Hexosaminidase A | GM2 ganglioside | Cherry-red spot, neurodegeneration, onion-skin lysosomes. 📌 Tay-SaX lacks heXosaminidase A. | AR |
| Niemann-Pick (Type A/B) | Sphingomyelinase | Sphingomyelin | Cherry-red spot (Type A), HSM, foam cells. | AR |
| Gaucher | Glucocerebrosidase | Glucocerebroside | HSM, pancytopenia, bone crises, Gaucher cells (crumpled tissue paper). 📌 Gaucher - Glucocerebrosidase. | AR |
| Fabry | α-galactosidase A | Ceramide trihexoside | Peripheral neuropathy, angiokeratomas, renal failure. | XLR |
| Krabbe | Galactocerebrosidase | Galactocerebroside, psychosine | Peripheral neuropathy, optic atrophy, globoid cells. | AR |
| Metachromatic Leukodystrophy | Arylsulfatase A | Sulfatides | Demyelination (central & peripheral), ataxia, dementia. | AR |
⭐ Cherry-red spot on macula is seen in Tay-Sachs disease and Niemann-Pick disease type A.
Other Notable LSDs - Rare & Remembered
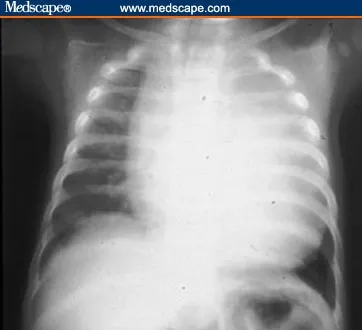
- Pompe Disease (GSD Type II)
- Enzyme: Acid $\alpha$-glucosidase
- Substrate: Glycogen (lysosomal)
- Key: Massive cardiomegaly, profound hypotonia, hepatomegaly. "Floppy infant".
- I-cell Disease (Mucolipidosis II)
- Enzyme: N-acetylglucosamine-1-phosphotransferase
- Substrate: Lysosomal enzymes mis-targeted (↑ in plasma)
- Key: Coarse facies, skeletal dysplasia, gingival hyperplasia, developmental delay.
-
⭐ I-cell disease: Deficiency of N-acetylglucosamine-1-phosphotransferase leads to mis-targeting of lysosomal enzymes.

- Wolman Disease
- Enzyme: Acid lipase
- Substrate: Cholesterol esters, triglycerides
- Key: Bilateral adrenal calcification, hepatosplenomegaly, FTT, early death.
- Cholesterol Ester Storage Disease (CESD)
- Enzyme: Acid lipase (milder)
- Substrate: Cholesterol esters, triglycerides
- Key: Hepatomegaly, hyperlipidemia, cirrhosis; later onset_
LSDs Dx & Rx - Spot & Support
- Dx: Clinical suspicion → Enzyme assays / Genetic tests (confirmatory, PND). Newborn screening (some LSDs).
- Rx: ERT, SRT, HSCT, Chaperones. Supportive care crucial. Gene therapy investigational.
⭐ ERT is available for several LSDs (e.g., Gaucher, Fabry, Pompe, MPS I, II, VI) but often has limited efficacy for CNS manifestations due to the blood-brain barrier.
High‑Yield Points - ⚡ Biggest Takeaways
- LSDs: Enzyme defects lead to lysosomal substrate accumulation.
- Gaucher disease: Most common; glucocerebrosidase deficiency; crumpled tissue paper cells, hepatosplenomegaly.
- Tay-Sachs disease: Hexosaminidase A defect; cherry-red spot, neurodegeneration, no hepatosplenomegaly.
- Niemann-Pick disease: Sphingomyelinase deficiency; foam cells, cherry-red spot, marked hepatosplenomegaly.
- Fabry disease: X-linked recessive; α-galactosidase A defect; angiokeratomas, peripheral neuropathy, renal failure.
- Mucopolysaccharidoses (MPS): Defective glycosaminoglycan (GAG) breakdown; e.g., Hurler syndrome (corneal clouding), Hunter syndrome (X-linked, no corneal clouding).
- Pompe disease: Acid α-glucosidase (acid maltase) defect; cardiomegaly, profound hypotonia, muscle weakness.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

