Overview & Epidemiology - The Winter Blues
- A subtype of Major Depressive Disorder (MDD) with a recurring seasonal pattern, typically starting in fall/winter and remitting in spring.
- Linked to reduced sunlight exposure, which impacts circadian rhythms, serotonin, and melatonin levels.
- Epidemiology:
- Affects ~5% of the U.S. population; more common in northern latitudes.
- Higher prevalence in women (F:M ratio ≈ 4:1).
- Typical age of onset is between 20-30 years.
⭐ For diagnosis, the seasonal depressive episodes must have occurred for at least 2 consecutive years, with seasonal episodes substantially outnumbering non-seasonal episodes over a lifetime.
Pathophysiology - Brain's Hibernation
- Circadian Rhythm Disruption: Reduced sunlight exposure in autumn/winter disrupts the suprachiasmatic nucleus (SCN) of the hypothalamus.
- Neurotransmitter Imbalance:
- ↑ Melatonin: Leads to lethargy and hypersomnia. The brain misinterprets dim light as a signal for prolonged nighttime.
- ↓ Serotonin (5-HT): Contributes to mood changes and carbohydrate cravings.
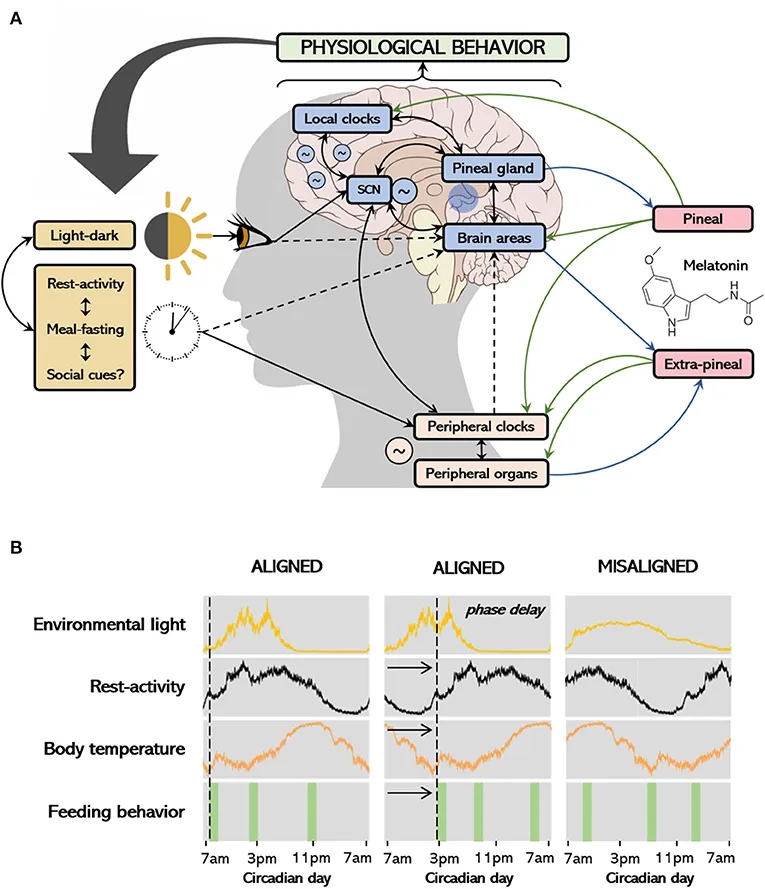
⭐ Phase-Delay Hypothesis: A key theory suggests that in SAD, the circadian rhythm is delayed relative to the external clock, causing a mismatch between sleep-wake cycles and other bodily rhythms.
Diagnosis & Features - Spotting the Slump
- Meets full criteria for Major Depressive Disorder (MDD) with a recurring seasonal pattern.
- Key diagnostic timing:
- Onset and remission occur at characteristic times of the year for at least 2 consecutive years.
- Seasonal episodes must substantially outnumber any non-seasonal episodes.
- Predominantly atypical depressive features:
- ↓ Energy (anergia) & leaden paralysis
- Hypersomnia (oversleeping)
- ↑ Appetite with carbohydrate craving
- Weight gain
📌 WINTER Mnemonic: Weight gain, Irritability, No energy, Tiredness, Eating carbs, Rejection sensitivity.
⭐ To diagnose, the seasonal pattern must be observed for at least 2 years, with seasonal episodes being far more common than non-seasonal ones throughout the patient's life.
Management - Let There Be Light
-
First-Line Therapies:
- Light Therapy: Core treatment.
- 10,000-lux broad-spectrum white light.
- Daily morning exposure for 30-45 minutes.
- Mechanism: ↓ melatonin, realigns circadian rhythm.
- Side effects: Headaches, eye strain, nausea.
- Cognitive Behavioral Therapy for SAD (CBT-SAD):
- Efficacy matches light therapy; longer-lasting effects.
- Targets negative thoughts & behavioral inactivation.
- Light Therapy: Core treatment.
-
Second-Line / Adjunctive:
- SSRIs (e.g., Fluoxetine, Sertraline) or Bupropion.
- Consider starting prophylactically in early autumn.
⭐ High-Yield: Screen for bipolar disorder before initiating light therapy, as it can precipitate hypomania/mania.

High‑Yield Points - ⚡ Biggest Takeaways
- Seasonal Affective Disorder (SAD) is a subtype of major depressive disorder with a recurring seasonal pattern.
- Episodes typically begin in the fall or winter and remit in the spring, occurring for at least 2 consecutive years.
- Key features include atypical depressive symptoms like hypersomnia, increased appetite or weight gain, and carbohydrate craving.
- Pathophysiology is linked to circadian rhythm disruption and altered melatonin metabolism.
- First-line treatment is bright light therapy (phototherapy).
- SSRIs and bupropion are effective pharmacotherapies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

