Pathophysiology - Brain Blood Flow Blues
- Core Insult: Cerebrovascular disease (CVD) disrupts cerebral blood flow (CBF), leading to neuronal death and cognitive deficits.
- Primary Mechanisms:
- Multi-infarct Dementia: Accumulation of multiple cortical or subcortical infarcts over time.
- Strategic Infarct Dementia: A single, crucial infarct in an area like the thalamus or hippocampus.
- Subcortical Ischemic Dementia: Chronic ischemia damages small vessels, causing diffuse white matter lesions (leukoaraiosis) and lacunar infarcts (e.g., Binswanger's disease).
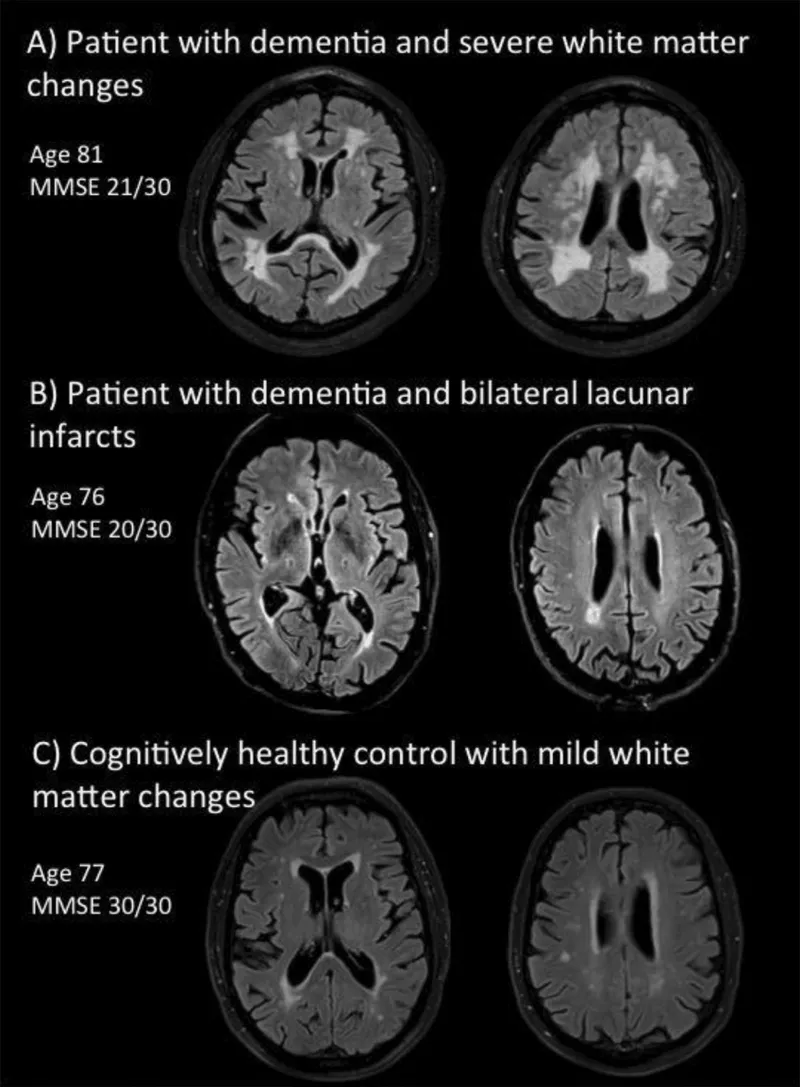
⭐ The classic presentation is a stepwise deterioration in cognitive function, where abrupt declines are interspersed with periods of stability, reflecting subsequent ischemic events.
Clinical Features - The Stepwise Slide
- Hallmark: Abrupt, stepwise deterioration in cognitive function, often temporally related to a cerebrovascular event (e.g., stroke).
- Course: Fluctuating progression. Function declines in discrete steps with periods of stability.
- Early & Prominent Deficits:
- Executive dysfunction (planning, decision-making).
- Slowed processing speed.
- Associated Features:
- Focal neurological signs (e.g., hemiparesis, visual defects).
- Pseudobulbar affect (emotional lability).
- Gait disturbance, unsteadiness, and frequent falls.
⭐ The "stepwise" decline is classic but not universal. A gradual, progressive course can occur with subcortical small vessel disease, often presenting with early and prominent executive dysfunction compared to the memory loss seen in Alzheimer's.
Diagnosis - Spotting the Strokes
- Clinical Picture: Hallmark is a stepwise decline in cognition, often with a clear temporal link to a stroke. Look for focal neurological deficits.
- Hemiparesis, pronator drift
- Visual field defects
- Pseudobulbar affect (emotional lability)
- Neuroimaging: MRI is the preferred modality.
- Reveals cortical/subcortical infarcts, lacunar strokes, or extensive white matter lesions (leukoaraiosis).

⭐ A "stepwise" cognitive decline, where function abruptly worsens after a vascular event and then stabilizes, is the classic historical feature distinguishing it from Alzheimer's gradual decline.
Management - Damage Control
- Primary Goal: Aggressively manage cardiovascular (CV) risk factors to prevent further ischemic insults.
- HTN: Strict BP control (target <130/80 mmHg).
- Diabetes: Glycemic control (target HbA1c ~7%).
- Hyperlipidemia: High-intensity statins.
- Antiplatelet therapy: Aspirin or clopidogrel for secondary stroke prevention.
- Cognitive Symptoms:
⭐ Cholinesterase inhibitors (donepezil, rivastigmine) and memantine can be considered, but have limited evidence of benefit compared to their use in Alzheimer's disease.
High-Yield Points - ⚡ Biggest Takeaways
- Stepwise cognitive decline with periods of stability, unlike the gradual decline in Alzheimer's disease.
- Caused by cerebrovascular disease, such as multiple cortical or subcortical infarcts.
- Strongly associated with vascular risk factors like hypertension, diabetes, and smoking.
- Often presents with focal neurological deficits (e.g., unilateral weakness, pronator drift).
- Neuroimaging is key, revealing evidence of prior strokes or significant white matter changes.
- Management focuses on aggressive risk factor control to prevent further ischemic events.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

