Pathophysiology & Etiology - Plaque & Tangle Tussle
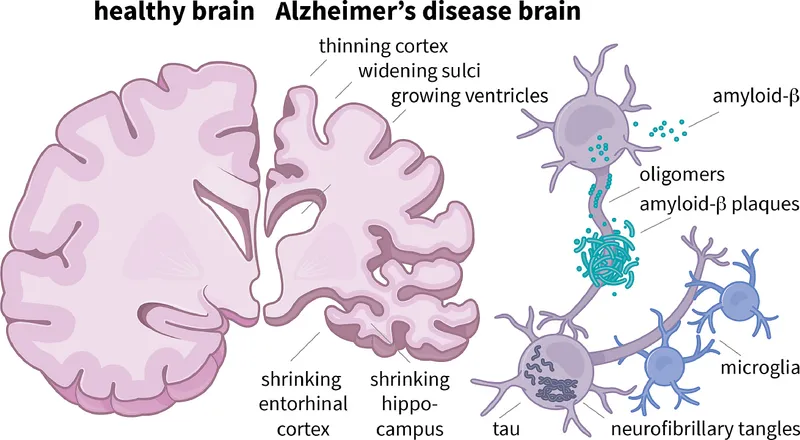
- Core Pathology: Two key players lead to synaptic dysfunction and neuronal loss:
- Extracellular: Amyloid-beta (Aβ) senile plaques.
- Intraneuronal: Tau neurofibrillary tangles (NFTs).
- Genetic Factors:
- Late-onset: Apolipoprotein E (ApoE ε4) allele is the strongest risk factor.
- Early-onset (Autosomal Dominant): Mutations in APP (Chr 21), PSEN1, PSEN2.
⭐ High-Yield: Down syndrome (Trisomy 21) significantly ↑ risk of early-onset Alzheimer's, as the APP gene is located on chromosome 21, leading to Aβ overproduction.
Clinical Presentation - The Slow Fade
- Insidious onset with gradual progression over 8-10 years.
- Short-term memory loss (anterograde amnesia) is the earliest and most prominent feature.
- Progressive Cognitive Decline:
- Executive dysfunction: Impaired planning, decision-making.
- Visuospatial deficits: Getting lost in familiar places.
- Language difficulties: Anomia (difficulty naming objects).
- Apraxia: Inability to perform learned motor tasks.
- Later stages involve personality and behavioral changes (e.g., apathy, agitation).
⭐ Memory for remote, well-learned facts and procedural memory (e.g., riding a bike) are typically preserved until late in the disease course.
Diagnostic Workup - Ruling It Out
Diagnosis is one of exclusion, focused on ruling out reversible causes of dementia.
-
Initial Screening: Cognitive tests.
- Mini-Mental State Examination (MMSE)
- Montreal Cognitive Assessment (MoCA)
-
Lab Tests: To exclude metabolic/deficiency states.
- CBC, CMP, TSH, Vitamin B12
-
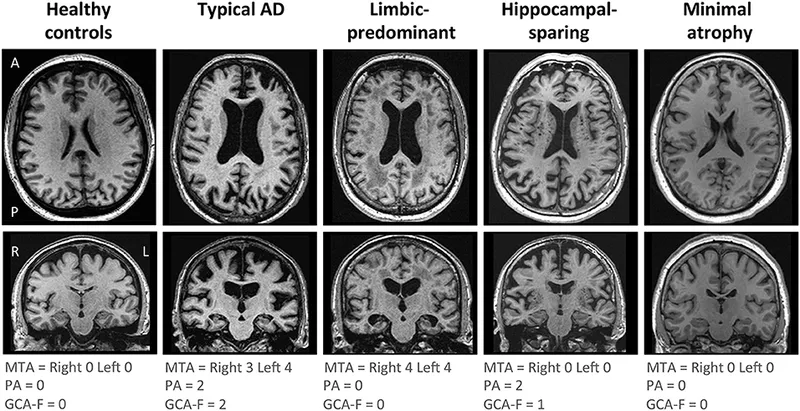
Imaging: CT or MRI to rule out structural causes (tumor, stroke).
- Medial temporal lobe (hippocampal) atrophy is a characteristic finding.
- CSF Analysis (less common in routine practice):
- ↓ Amyloid-beta 42 (Aβ-42)
- ↑ Total Tau & Phosphorylated Tau (p-Tau)
⭐ While imaging can show atrophy, a definitive diagnosis of Alzheimer's disease still requires histopathological confirmation on autopsy.
Management - Holding the Line
- Pharmacotherapy: Primarily symptomatic and supportive.
- Mild-to-moderate: Cholinesterase inhibitors (Donepezil, Rivastigmine, Galantamine).
- Moderate-to-severe: NMDA receptor antagonist (Memantine).
- 📌 Mnemonic: "Done with my gal, I need a river of memories" (Donepezil, Galantamine, Rivastigmine).
- Non-pharmacologic: Physical activity, cognitive stimulation, and management of behavioral symptoms like agitation.
⭐ Cholinesterase inhibitors can cause significant cholinergic side effects, including nausea, vomiting, diarrhea, and bradycardia.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common cause of dementia in the elderly, presenting with insidious short-term memory loss.
- Key pathology: extracellular amyloid-beta plaques and intracellular neurofibrillary tangles (hyperphosphorylated tau protein).
- Strongest genetic risk factor is the ApoE4 allele; early-onset linked to APP and presenilin mutations.
- Leads to diffuse cortical atrophy, most pronounced in the hippocampus and temporal lobes.
- Caused by a significant deficiency in acetylcholine.
- Treatment involves cholinesterase inhibitors and NMDA receptor antagonists.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

