Initial Workup - Spotting the Storm
-
Assess Episode Type: Is it Mania or Hypomania?
- Mania: Symptoms ≥ 1 week, causing marked functional impairment, hospitalization, or psychosis.
- Hypomania: Symptoms ≥ 4 days, observable change in function, but no marked impairment/hospitalization/psychosis.
-
Evaluate Symptoms: Use the 📌 DIGFAST mnemonic:
- Distractibility
- Indiscretion (risky behaviors)
- Grandiosity
- Flight of ideas
- Activity increase
- Sleep deficit
- Talkativeness
-
Rule Out Other Causes:
- Substances: Cocaine, amphetamines, high-dose steroids. Order a UDS.
- Medical: Hyperthyroidism, neurologic conditions. Order a TSH.
⭐ Always screen for substance use (UDS) and thyroid dysfunction (TSH) in a patient with new-onset manic symptoms.
Acute Mania - Taming the Tempest
- Immediate Goal: Rapid stabilization & ensure safety. Prioritize de-escalation.
- Severe Mania / Agitation: Hospitalization is paramount.
- For acute agitation, use intramuscular (IM) medication:
- Olanzapine
- Ziprasidone
- For acute agitation, use intramuscular (IM) medication:
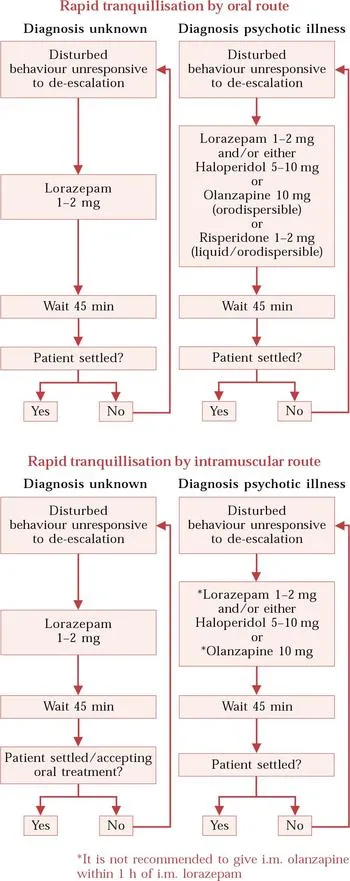
- Pharmacotherapy First-Line:
- Mood Stabilizers: Lithium (acute target: 0.8-1.2 mEq/L) or Valproate.
- Second-Gen Antipsychotics (SGAs): Risperidone, Olanzapine, Quetiapine. Can be used as monotherapy or adjunctively with mood stabilizers for quicker symptom control.
⭐ For an acutely agitated manic patient, a combination of an antipsychotic (e.g., olanzapine) and a benzodiazepine (e.g., lorazepam) is often used for rapid tranquilization.
Bipolar Depression - The Other First Face
- Often the initial presentation of Bipolar I or II. Misdiagnosis as unipolar depression is common and dangerous.
- Primary Goal: Treat depression without inducing mania.
- First-Line Pharmacotherapy:
- Monotherapy with Second-Generation Antipsychotics (SGAs): Quetiapine, Lurasidone.
- Combination therapy: Olanzapine-fluoxetine.
- Maintenance, Not Acute:
- Lamotrigine is effective for maintenance to prevent future depressive episodes.
- ⚠️ Requires slow titration due to the risk of Stevens-Johnson Syndrome (SJS).
⭐ Antidepressant monotherapy (e.g., SSRIs) is contraindicated. It can precipitate a manic or hypomanic episode in a patient with unrecognized bipolar disorder.
High‑Yield Points - ⚡ Biggest Takeaways
- Differentiating from unipolar depression is critical; a history of mania or hypomania is definitional.
- For acute mania, first-line agents are mood stabilizers (Lithium, Valproate) or second-generation antipsychotics (SGAs).
- Severe mania often requires combination therapy: a mood stabilizer PLUS an SGA.
- Antidepressant monotherapy is contraindicated due to the risk of precipitating a manic episode.
- If mania emerges while on an antidepressant, taper and discontinue the antidepressant immediately.
- Treat bipolar depression with mood stabilizers or specific SGAs (e.g., quetiapine, lurasidone), not antidepressants alone.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

