Diagnosis & Criteria - Defining the Dread
- Hallmark: Recurrent, unexpected panic attacks.
- Followed by ≥1 month of one or both:
- Persistent concern about future attacks or their consequences (e.g., "going crazy").
- Significant maladaptive behavior change related to attacks (e.g., avoiding exercise).
- Panic Attack: Abrupt fear surge peaking within minutes with ≥4 of 13 official symptoms.
- 📌 Common symptoms: Palpitations, sweating, trembling, shortness of breath, chest pain, dizziness, paresthesias, derealization, fear of dying or losing control.
⭐ Key differentiator: The panic attacks are uncued ("out of the blue"). If attacks are consistently triggered by a specific situation, consider another diagnosis like a specific phobia or social anxiety disorder.
Pathophysiology - Brain on Fire
- Neurotransmitter Dysregulation: Imbalance in key systems.
- Norepinephrine (NE): ↑ activity, especially from the locus coeruleus (the brain's "panic button").
- Serotonin (5-HT): ↓ levels, leading to poor mood and anxiety regulation.
- GABA: ↓ inhibitory function, causing unchecked neuronal firing.
- Fear Circuitry: Hyperactive amygdala (fear center) with poor top-down control from the prefrontal cortex (PFC).
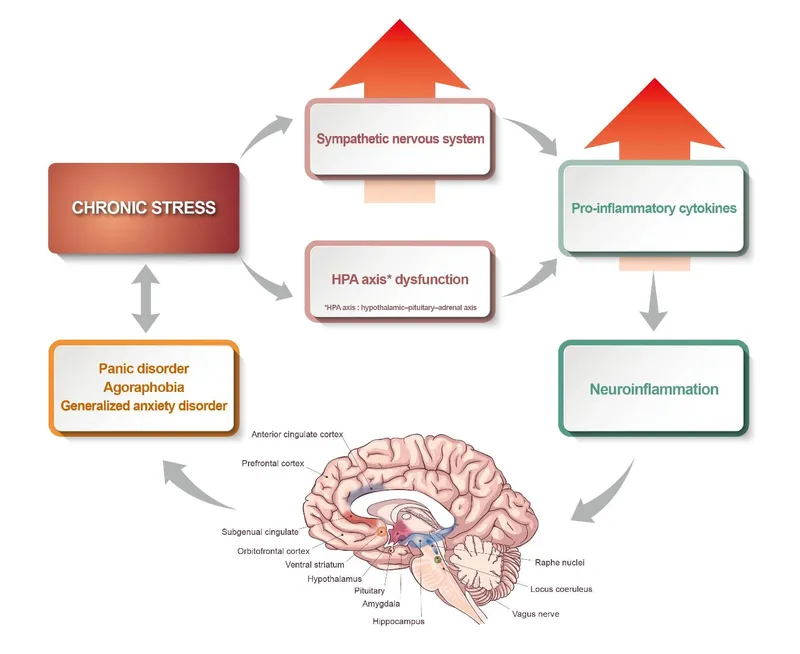
⭐ Patients with panic disorder often exhibit hypersensitivity to carbon dioxide ($CO_2$) inhalation, which can trigger panic attacks in a laboratory setting.
Clinical Features & Differentials - The Sudden Storm
- Abrupt surge of intense fear peaking within minutes. Requires ≥4 of 13 DSM-5 symptoms:
- Palpitations, sweating, trembling, shortness of breath (SOB).
- Chest pain, dizziness, nausea, paresthesias.
- Derealization/depersonalization, fear of losing control or dying.
- Crucial Differentials (Rule Out First):
- Medical: Myocardial infarction, pulmonary embolism, hyperthyroidism, pheochromocytoma, hypoglycemia.
- Substance-Induced: Caffeine, stimulants (cocaine, amphetamines), alcohol/sedative withdrawal.
⭐ Panic disorder patients often present to the ED fearing a heart attack; an EKG is essential to rule out cardiac ischemia.
Management - Taming the Terror
- Long-Term (First-Line): SSRIs/SNRIs and CBT are cornerstones. SSRIs require 4-6 weeks for full effect. CBT focuses on exposure and cognitive restructuring.
- Acute Management: Benzodiazepines provide rapid relief but should be used short-term (<4 weeks) as a bridge due to dependence risk.
- Treatment Duration: Continue successful pharmacotherapy for at least 6-12 months after remission to prevent relapse.
⭐ Initial SSRI treatment can paradoxically worsen anxiety. Counsel patients on this risk and use a "start low, go slow" titration strategy.
Comorbidities & Prognosis - The Ripple Effect
Error generating content for this concept group: Invalid JSON response
High‑Yield Points - ⚡ Biggest Takeaways
- Recurrent, unexpected panic attacks followed by ≥1 month of persistent worry about future attacks or maladaptive behavior changes.
- Strongly associated with agoraphobia, the fear of situations where escape might be difficult.
- First-line treatment is a combination of SSRIs (e.g., sertraline) and Cognitive Behavioral Therapy (CBT).
- Benzodiazepines are effective for acute management but are not preferred for long-term use due to dependence risk.
- Always rule out underlying medical causes like hyperthyroidism, pheochromocytoma, and cardiac arrhythmias.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

