V/Q Basics - The Air-Blood Ratio
- Ventilation (V): The process of moving air into and out of the alveoli.
- Perfusion (Q): The flow of blood through the pulmonary capillary bed.
- The normal V/Q ratio for the entire lung is approximately 0.8, reflecting that perfusion is slightly greater than ventilation.
- V/Q Mismatches:
- Dead Space ($V/Q > 0.8$): Alveoli are ventilated but not perfused. Air is inhaled, but there's no blood to receive the oxygen.
- Shunt ($V/Q < 0.8$): Alveoli are perfused but not ventilated. Blood passes by, but there's no oxygen to pick up.
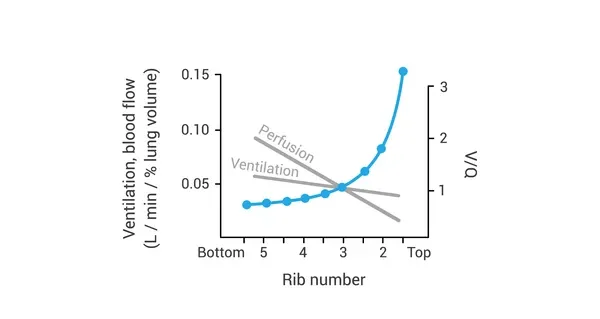
⭐ In an upright lung, gravity causes both ventilation and perfusion to be greatest at the base. However, perfusion's increase is more pronounced, leading to a lower V/Q at the base and a higher V/Q at the apex.
COPD Pathophysiology - Lungs Under Siege
- COPD encompasses two primary pathologies leading to V/Q mismatch:
- Chronic Bronchitis ("Blue Bloaters"): An airway disease.
- Mucus gland hypertrophy & hypersecretion → Airway plugging & inflammation.
- Results in a shunt-like state (V/Q ≈ 0) → Hypoxemia, hypercapnia.
- Emphysema ("Pink Puffers"): An alveolar disease.
- Destruction of alveolar walls (↑ elastase activity) → ↓ Surface area for gas exchange.
- Loss of elastic recoil → Air trapping (↑ RV, ↑ TLC).
- Creates dead space ventilation (V/Q → ∞).
- Chronic Bronchitis ("Blue Bloaters"): An airway disease.

⭐ Reid Index > 0.5 is a key histologic finding in Chronic Bronchitis, indicating mucus gland hypertrophy.
📌 Mnemonic: "Blue Bloaters" are blue (cyanosis) and bloated (edema), while "Pink Puffers" are pink (hyperventilation) and puff (pursed lips).
The Mismatch Mechanism - COPD's Bad Connection
COPD disrupts efficient gas exchange, primarily creating a low ventilation/perfusion (V/Q) state. This mismatch is the main driver of hypoxemia, as blood flows through lung areas that are poorly oxygenated.
- Low V/Q (Shunt): This is the predominant lesion. Bronchial inflammation and mucus block airways, reducing ventilation (V) to areas that still have blood flow (Q).
- High V/Q (Dead Space): In emphysematous areas, alveolar wall destruction eliminates capillaries, reducing perfusion (Q) in ventilated zones. This ventilation is wasted.

- Failed Compensation: Normally, hypoxic vasoconstriction diverts blood from poorly ventilated areas. In diffuse lung disease like COPD, this mechanism is inefficient and cannot correct the widespread mismatch.
⭐ The Alveolar-arterial (A-a) gradient is characteristically widened in COPD, reflecting the severity of the V/Q defect.
Clinical Correlation - Puffer vs. Bloater

-
Pink Puffer (Emphysema-Dominant)
- Marked by dyspnea, pursed-lip breathing ("puffing") to maintain alveolar pressure.
- Maintains near-normal gas exchange via hyperventilation.
- Classic findings: Barrel chest, muscle wasting, minimal cyanosis.
- V/Q is relatively matched until late disease.
-
Blue Bloater (Bronchitis-Dominant)
- Defined by chronic productive cough, leading to severe hypoxemia and hypercapnia.
- Results in cyanosis ("blue") and peripheral edema ("bloater") from cor pulmonale.
- Represents a profound V/Q mismatch (low V/Q).
⭐ Exam Pearl: Pure phenotypes are uncommon. Most COPD patients exhibit a mixture of emphysema and chronic bronchitis features.
High-Yield Points - ⚡ Biggest Takeaways
- COPD is an obstructive disease causing air trapping and creating areas of low V/Q ratio.
- Impaired ventilation (V) with relatively preserved perfusion (Q) leads to a physiological shunt.
- Chronic alveolar hypoxia triggers hypoxic pulmonary vasoconstriction (HPV).
- Widespread HPV increases pulmonary vascular resistance, causing pulmonary hypertension and cor pulmonale.
- This mismatch is the primary cause of hypoxemia and hypercapnia in "blue bloaters."
- High-flow O₂ can worsen hypercapnia by reversing HPV and increasing dead space.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

