Ventilatory Response - Gearing Up for Action
- Anticipatory Rise: Ventilation ↑ before exercise starts, driven by central command from the motor cortex.
- Initial Rapid Rise (Phase I/II):
- Immediate ↑ in ventilation at exercise onset.
- Mediated by afferent signals from mechanoreceptors in exercising limbs.
- Slower Sustained Rise (Phase III):
- Fine-tuned by peripheral chemoreceptors sensing ↑ $K^+$, ↑ body temp, and metabolic acidosis ($H^+$).
- Central chemoreceptors respond to ↑ $PCO_2$ in cerebrospinal fluid.
- Gas Exchange Dynamics:
- Minute ventilation ($V_E = RR \times TV$) increases linearly with metabolic rate.
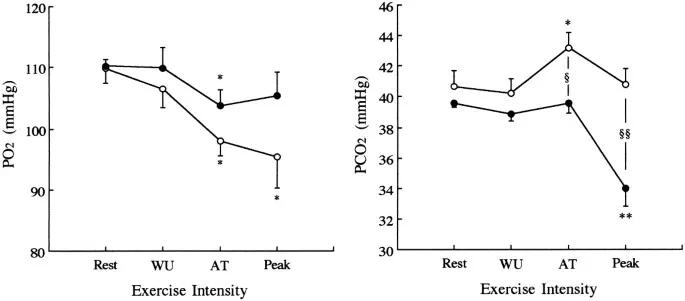
- Arterial $PaO_2$ and $PaCO_2$ remain remarkably stable during submaximal exercise.
⭐ During moderate exercise, the primary drivers for increased ventilation are central command and neurogenic reflexes from limbs, NOT changes in arterial $PaO_2$ or $PaCO_2$.
Gas Exchange & Transport - The Oxygen Shuffle
- During intense exercise, O2 consumption and CO₂ production by muscles skyrocket.
- This metabolic shift causes a rightward shift in the O₂-Hb dissociation curve, enhancing O₂ unloading to tissues.
- Mechanism: ↓ Hb affinity for O₂.
- Key drivers: ↑PCO₂, ↓pH (Bohr effect), and ↑ temperature.
- The Arterial-Venous (A-V) O₂ difference widens dramatically.
- Arterial O₂ content remains stable.
- Venous O₂ content plummets due to ↑ extraction.
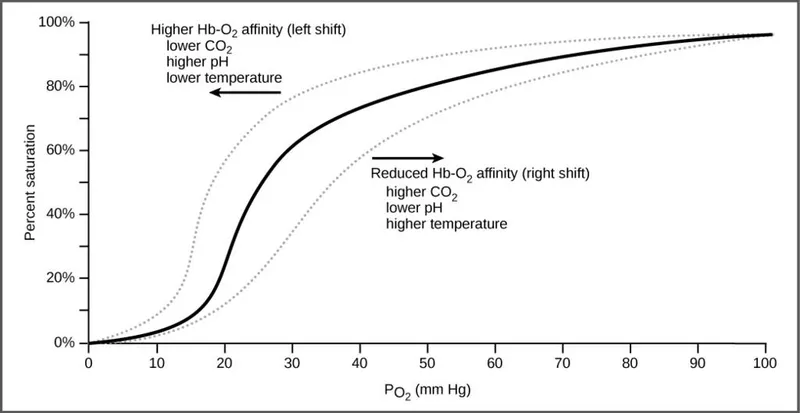
⭐ Myoglobin has a higher O₂ affinity than hemoglobin and a hyperbolic (non-sigmoidal) curve. It acts as an O₂ reserve in muscle, only releasing its O₂ at very low intramuscular PO₂ levels.
Limits & Thresholds - Hitting the Wall
-
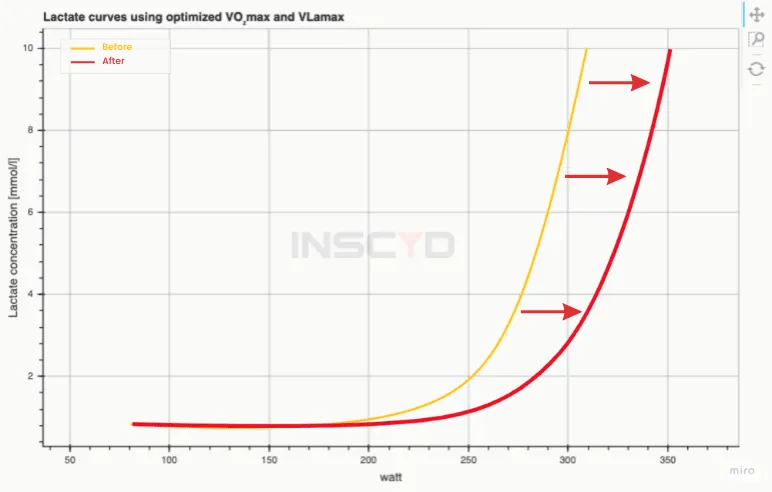
Anaerobic Threshold (AT): The exercise intensity at which blood lactate begins to systematically increase. Also called Lactate Threshold (LT).
- Represents a shift toward anaerobic metabolism as pyruvate is converted to lactate.
- Correlate: Ventilatory Threshold (VT), an inflection point where ventilation ($V_E$) increases disproportionately to oxygen consumption ($V_{O_2}$).
- Mechanism: Lactic acid buffering by bicarbonate ($HCO_3^-$) generates non-metabolic $CO_2$, driving ventilation.
-
Maximal Oxygen Uptake ($V_{O_2}$ max): The physiological ceiling for oxygen delivery and utilization during maximal exertion.
- Primary limiting factor in healthy individuals is cardiac output.
⭐ In severe COPD, the primary limit to exercise is ventilatory capacity (i.e., breathing limitation), not cardiac output.
Cardiopulmonary Adaptations - The Great Accommodator
- Ventilation (VE): ↑ linearly with O₂ consumption & CO₂ production.
- Initially met by ↑ Tidal Volume (TV), then ↑ Respiratory Rate (RR).
- V/Q ratio becomes more uniform, optimizing gas exchange.
- Gas Transport & Exchange:
- Pulmonary blood flow ↑ significantly.
- Venous O₂ content (PvO₂) ↓ due to ↑ tissue extraction, widening the A-vO₂ difference.
- Arterial Blood Gases:
- PaO₂ & PaCO₂: Maintained near resting levels until the anaerobic threshold.
- pH: Stable until anaerobic threshold, then ↓ from lactic acidosis.
⭐ The respiratory system is rarely the limiting factor in healthy individuals during exercise. PaO₂ and PaCO₂ are remarkably well-maintained despite huge metabolic demand.
High‑Yield Points - ⚡ Biggest Takeaways
- Exercise ↑ ventilation primarily via increased tidal volume; respiratory rate increases more significantly at high intensity.
- Arterial PaO2 and PaCO2 remain near-normal during moderate exercise due to tightly matched alveolar ventilation.
- Mixed venous PCO2 (PvCO2) increases because of ↑ CO2 production by metabolically active muscles.
- Arterial pH decreases only during strenuous exercise, secondary to lactic acidosis.
- The V/Q ratio becomes more uniform throughout the lungs, improving overall gas exchange efficiency.
- A rightward shift of the oxyhemoglobin curve (↑ temp, ↓ pH) enhances O2 unloading to tissues.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

