JGA Anatomy - The Control Center

The Juxtaglomerular Apparatus (JGA) is a specialized structure at the vascular pole of the glomerulus, crucial for regulating blood pressure and filtration rate.
- Components:
- Macula Densa: Specialized cells in the Distal Convoluted Tubule (DCT). They act as chemoreceptors, sensing tubular fluid [NaCl] concentration. ↓NaCl stimulates renin release.
- Juxtaglomerular (JG) Cells: Modified smooth muscle cells in the afferent arteriole wall. They synthesize, store, and secrete renin. They also function as baroreceptors, sensing renal perfusion pressure.
- Extraglomerular Mesangial (Lacis) Cells: Transmit signals between the macula densa and JG cells.
⭐ High-Yield: JG cells are derived from smooth muscle cells of the afferent arteriole and are the primary site of renin production in the kidney.
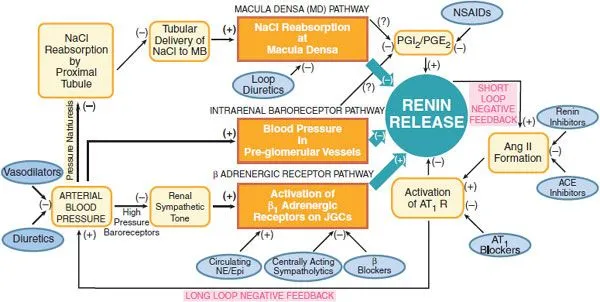
Renin Release - The Three Triggers
Renin secretion from juxtaglomerular (JG) cells is stimulated by three main pathways:
-
Macula Densa Pathway (Chemoreceptors)
- Senses ↓ NaCl concentration in the distal convoluted tubule (DCT).
- Triggers renin release via prostaglandins.
-
Afferent Arteriole Pathway (Baroreceptors)
- JG cells act as mechanoreceptors, sensing ↓ stretch due to low renal blood pressure.
- Directly stimulates renin release.
-
Sympathetic Nerve Pathway (β1 Receptors)
- Norepinephrine from renal sympathetic nerves stimulates β1-adrenergic receptors on JG cells.
⭐ Exam Favorite: NSAIDs (e.g., ibuprofen) can cause acute kidney injury by inhibiting prostaglandin synthesis. This blocks the macula densa pathway, reducing renin release and leading to ↓ GFR, especially in patients with already reduced renal perfusion.
Modulators - Brakes & Boosters
-
Boosters (↑ Renin Release)
- Juxtaglomerular (JG) cells act as intra-renal baroreceptors, sensing ↓ renal blood pressure.
- Macula densa cells in the DCT sense ↓ NaCl delivery, signaling JG cells to release renin.
- Sympathetic nervous system activation directly stimulates β1-adrenergic receptors on JG cells.
- Prostaglandins (PGE₂, PGI₂) also directly stimulate renin release.
-
Brakes (↓ Renin Release)
- Angiotensin II exerts direct negative feedback on JG cells (short-loop feedback).
- Atrial Natriuretic Peptide (ANP), released from stretched atria, inhibits renin secretion.
- Increased blood pressure and ↑ NaCl at macula densa provide direct inhibitory signals.
- Beta-blockers inhibit the sympathetic stimulation of JG cells.
⭐ NSAIDs block prostaglandin synthesis, thus ↓ renin secretion. This is critical in patients with low effective circulating volume (e.g., heart failure), as it can precipitate acute kidney injury by constricting the afferent arteriole.
High‑Yield Points - ⚡ Biggest Takeaways
- Renin is the rate-limiting enzyme in the RAAS, secreted by juxtaglomerular (JG) cells.
- Primary triggers for release are ↓ renal blood pressure, ↓ NaCl delivery to the macula densa, and ↑ sympathetic stimulation (β1-receptors).
- JG cells act as intra-renal baroreceptors sensing afferent arteriole stretch.
- Macula densa cells are chemoreceptors for distal tubular fluid's NaCl concentration.
- β-blockers and ANP inhibit renin secretion.
- Angiotensin II exerts negative feedback on renin release from JG cells.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

