RAAS Triggers - The Pressure Alarm
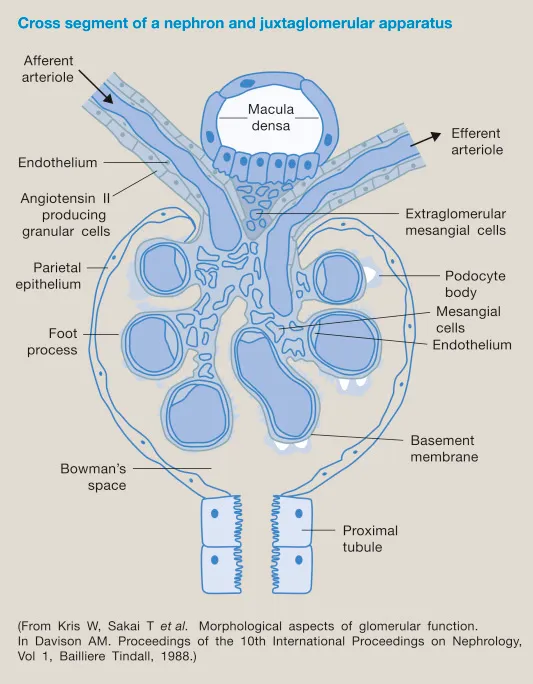
Renin release from juxtaglomerular (JG) cells is stimulated by three main triggers:
- ↓ Renal Blood Flow: JG cells act as intra-renal baroreceptors, sensing low perfusion.
- ↓ NaCl to Distal Tubule: Macula densa cells sense decreased sodium chloride delivery.
- ↑ Sympathetic Tone: β1-adrenergic receptors on JG cells are activated by norepinephrine.
⭐ The macula densa senses low NaCl delivery to the distal tubule, signaling JG cells to release renin.
RAAS Cascade - A Chain Reaction
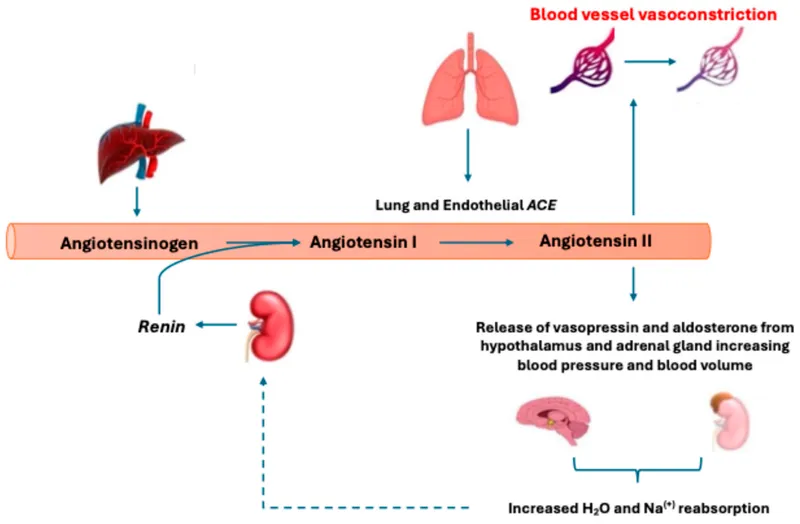
The liver produces angiotensinogen. Kidneys release renin, which converts it to angiotensin I. Angiotensin-Converting Enzyme (ACE) from the lungs then transforms it into the potent vasoconstrictor, angiotensin II, which acts on various tissues to raise blood pressure.
$Angiotensinogen \xrightarrow{Renin} Angiotensin\ I \xrightarrow{ACE} Angiotensin\ II$
⭐ ACE, found primarily in pulmonary and renal endothelium, also breaks down bradykinin, a vasodilator. This dual action further elevates blood pressure.
Angiotensin II Effects - The Master Squeezer
Acts via Gq-coupled AT1 receptors to orchestrate a systemic "squeeze" on blood vessels and fluid volume, raising blood pressure.
- Vascular System: Potent vasoconstriction of arterioles → ↑ Systemic Vascular Resistance (SVR).
- Adrenal Gland: Stimulates aldosterone release from the zona glomerulosa → ↑ Na⁺ and H₂O reabsorption.
- Brain:
- ↑ ADH (vasopressin) secretion from the posterior pituitary.
- Stimulates the hypothalamic thirst center.
- Kidneys:
- Constricts the efferent arteriole.
⭐ Angiotensin II preferentially constricts the efferent arteriole, which helps maintain GFR during low renal blood flow states.
Aldosterone's Role - The Salt Saver
- Source: Released from the adrenal cortex (zona glomerulosa).
- Target: Acts on principal cells within the kidney's collecting ducts.
- Mechanism:
- Upregulates epithelial Na+ channels (ENaC) on the apical side.
- Boosts Na+/K+ ATPase pumps on the basolateral side.
- Net Effect:
- Promotes robust Na+ (salt) and water retention.
- Increases K+ excretion into the urine.
- Ultimately raises blood volume and blood pressure.

⭐ Aldosterone works on the principal cells of the collecting duct to increase Na+ reabsorption and K+ secretion.
RAAS Pharmacology - Hacking the System
📌 'A-pril' fools the ACE; '-sartan' blocks the 'czar' Angiotensin II.
Targets key pathway steps to lower blood pressure. Major classes:
- ACE Inhibitors (-pril): Block conversion of Angiotensin I to II.
- ARBs (-sartan): Block Angiotensin II receptors directly.
- Aldosterone Antagonists (Spironolactone): Block aldosterone effects.
- Direct Renin Inhibitors (Aliskiren): Inhibit renin's activity.
⭐ ACE inhibitors' characteristic dry cough is due to the accumulation of bradykinin; ARBs do not have this side effect.
Key Risks: Hyperkalemia, hypotension, and Angioedema (especially with ACEi).
High‑Yield Points - ⚡ Biggest Takeaways
- Renin release from the kidney's juxtaglomerular apparatus is the rate-limiting step, triggered by ↓ renal perfusion.
- Angiotensin II is the primary effector, causing potent vasoconstriction (↑ SVR) and stimulating aldosterone release from the adrenal cortex.
- Aldosterone acts on the distal convoluted tubule & collecting duct to ↑ Na+ and H₂O reabsorption, expanding blood volume.
- ACE from the lungs converts Ang I to Ang II and also breaks down bradykinin (implicated in ACE inhibitor cough).
- The system defends against hypotension, making it a key target for antihypertensive drugs (e.g., ACE inhibitors, ARBs).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

