RAAS Overview - The Pressure Patrol
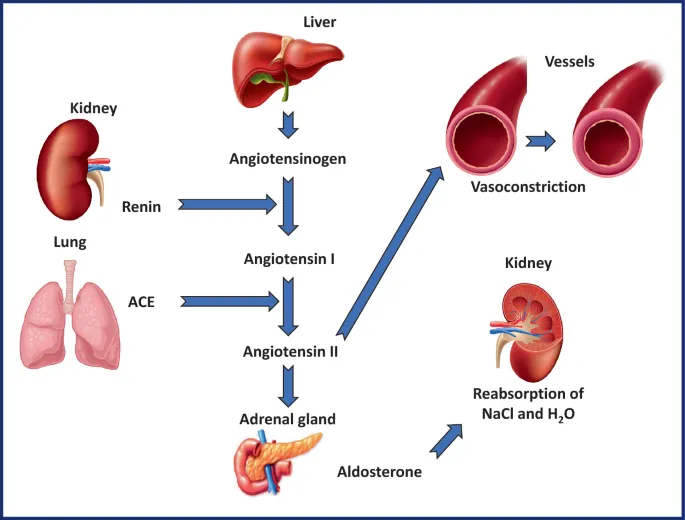
The Renin-Angiotensin-Aldosterone System (RAAS) is a critical hormonal cascade that regulates blood pressure, fluid, and electrolyte balance. Its primary trigger is a decrease in renal perfusion or blood pressure.
- Primary Effector: Angiotensin II.
- Potent vasoconstrictor (↑ SVR).
- Stimulates aldosterone release from the adrenal cortex.
- Promotes ADH release & thirst.
⭐ Angiotensin II is the most potent vasoconstrictor in the human body, directly increasing systemic vascular resistance to rapidly elevate blood pressure.
Aldosterone Synthesis - Adrenal Factory
- Location: Zona Glomerulosa of the adrenal cortex.
- 📌 Mnemonic (superficial to deep): Goes Faster with Red Bull (Glomerulosa, Fasciculata, Reticularis).
- Synthesis Pathway: A multi-step enzymatic process converting cholesterol into aldosterone.
- Cholesterol → Pregnenolone
- Pregnenolone → Progesterone
- Progesterone → 11-Deoxycorticosterone (via 21-hydroxylase)
- 11-Deoxycorticosterone → Corticosterone
- Corticosterone → Aldosterone (via Aldosterone Synthase)

- Primary Regulators of Release:
- ↑ Angiotensin II
- ↑ Plasma [$K^+$] (Hyperkalemia) is a potent direct stimulus.
⭐ Exam Favorite: While Angiotensin II is the main trigger, ACTH has a transient, minor role in aldosterone release. Chronic ACTH stimulation does not lead to sustained high aldosterone levels (Aldosterone Escape).
Release Regulation - The Control Knobs
- Primary Stimulators:
- Angiotensin II: The most potent stimulus from the RAAS pathway. Binds AT1 receptors, activating the IP3/DAG pathway to ↑ intracellular Ca²⁺.
- Hyperkalemia (↑ Plasma K⁺): The most potent direct stimulus. Depolarizes glomerulosa cells, opening voltage-gated Ca²⁺ channels.
- A plasma K⁺ rise of just 0.1 mEq/L can trigger aldosterone secretion.
- Minor Stimulator:
- ACTH: Provides a weak and transient stimulus for aldosterone release.
- Primary Inhibitor:
- Atrial Natriuretic Peptide (ANP): Released from stretched atria (hypervolemia); directly inhibits aldosterone secretion.
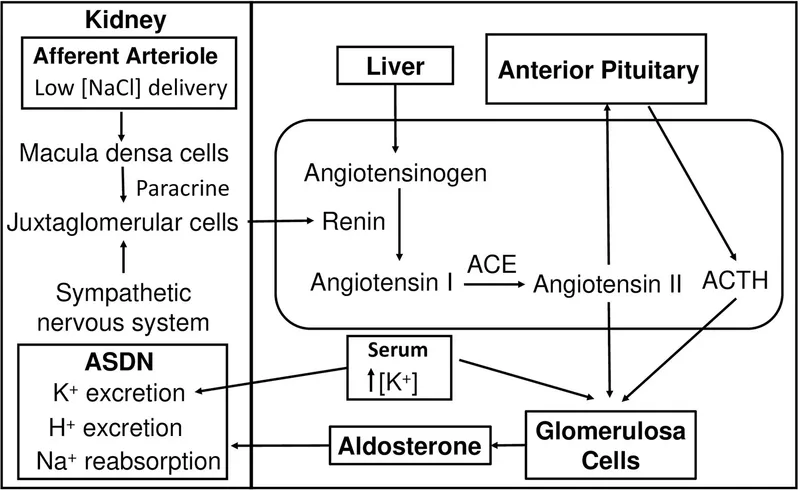
⭐ Hyperkalemia is the most sensitive and potent direct stimulus for aldosterone secretion. This direct feedback loop is critical for preventing life-threatening arrhythmias from high potassium.
Mechanism of Action - Salty Secrets
- Lipophilic Nature: As a steroid hormone, aldosterone freely diffuses across the cell membrane of principal cells in the distal convoluted tubule (DCT) and collecting ducts.
- Receptor Binding: Binds to its intracellular mineralocorticoid receptor (MR) in the cytoplasm.
- Gene Transcription: The hormone-receptor complex translocates to the nucleus, functioning as a transcription factor to upregulate specific genes.
- ENaC: Increases synthesis of apical epithelial Na⁺ channels (ENaC) → ↑ Na⁺ reabsorption from lumen.
- Na⁺/K⁺ Pump: Increases synthesis of basolateral Na⁺/K⁺-ATPase pumps → ↑ K⁺ secretion into lumen.
⭐ Aldosterone also stimulates H⁺ secretion via H⁺-ATPase in α-intercalated cells, contributing to metabolic alkalosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Angiotensin II is the primary stimulator for aldosterone synthesis from the zona glomerulosa of the adrenal cortex.
- Hyperkalemia is a potent, direct stimulator of aldosterone release, independent of the RAAS pathway.
- The rate-limiting enzyme for synthesis is aldosterone synthase (CYP11B2).
- Angiotensin II signaling occurs via a Gq protein-coupled receptor, utilizing the IP3/DAG second messenger system.
- ACTH provides a minor, transient stimulus for aldosterone secretion.
- ANP and BNP inhibit aldosterone release from the adrenal gland.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

