Venous Pressure - The Low-Pressure Life
- Systemic veins are a high-capacitance, low-pressure reservoir, holding ~70% of blood volume at just 2-8 mmHg.
- This large compliance allows veins to accommodate significant volume changes with minimal pressure shifts.
Key factors aiding venous return to the heart:
- Skeletal Muscle Pump: Muscle contractions squeeze deep veins, propelling blood forward.
- Respiratory Pump: Inspiration decreases intrathoracic pressure, drawing blood into the chest.
- Sympathetic Venoconstriction: Reduces venous compliance, ↑ pressure and flow.
⭐ Central Venous Pressure (CVP) reflects right atrial pressure and is a crucial estimate of preload.

Venous Return Curve - Going With the Flow

- Venous return (VR) is the rate of blood flow back to the heart, driven by the pressure gradient between mean systemic filling pressure (Pmsf) and right atrial pressure (RAP).
- Formula: $VR = (P_{msf} - P_{ra}) / RVR$
- Pmsf (x-intercept): Pressure when flow stops. Reflects volume status & venomotor tone.
- ↑ Volume (infusion) or ↑ sympathetic tone → ↑ Pmsf (curve shifts right).
- ↓ Volume (hemorrhage) → ↓ Pmsf (curve shifts left).
- Slope: Determined by resistance to venous return (RVR).
- ↓ RVR (e.g., AV fistula) → ↑ slope (steeper).
⭐ The intersection of the venous return and cardiac function curves determines the steady-state cardiac output and right atrial pressure.
Factors Affecting Return - The Push and Pull
Venous return (VR) is driven by the pressure gradient between peripheral veins and the right atrium. $VR = (P_{msf} - P_{ra}) / RVR$
-
Push Factors (↑ VR)
- ↑ Mean Systemic Filling Pressure ($P_{msf}$): Caused by ↑ blood volume or ↑ venomotor tone.
- Skeletal muscle pump: Contraction compresses deep veins.
- Respiratory pump: Inspiration ↓ intrathoracic pressure, pulling blood into the chest.
-
Pull Factors (↑ VR)
- ↓ Right Atrial Pressure ($P_{ra}$): Improved cardiac function enhances suction.
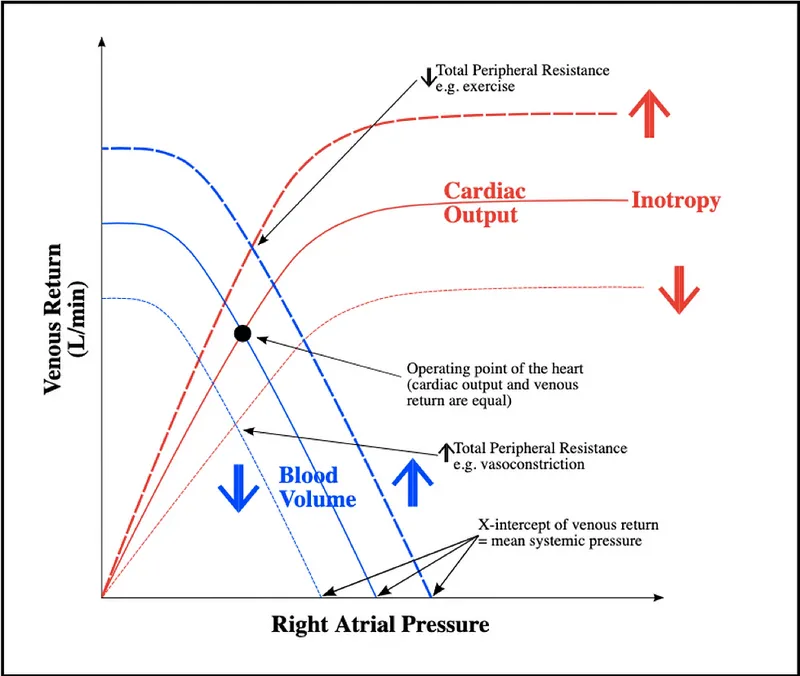
⭐ In heart failure, an elevated Right Atrial Pressure ($P_{ra}$) directly opposes and reduces venous return, contributing to systemic congestion.
Clinical Tie-ins - When Flow Goes Wrong
- Heart Failure (Right-sided):
- ↓ Cardiac contractility → blood backs up → ↑ Central Venous Pressure (CVP).
- Signs: Jugular Venous Distension (JVD), peripheral edema, ascites, hepatomegaly.
- Hemorrhage & Shock:
- ↓ Blood volume → ↓ Mean Systemic Filling Pressure (MSFP) → ↓ venous return.
- Leads to ↓ Cardiac Output (CO) and hypotension.
- Body compensates via venoconstriction to ↑ venous return.
- Fluid Administration:
- IV fluids or transfusions → ↑ blood volume → ↑ MSFP → ↑ venous return.
⭐ Central Venous Pressure (CVP) reflects right atrial pressure. A CVP > 8 mmHg is a key indicator of volume overload or right ventricular failure.

- Venous return (VR) must equal cardiac output (CO) for circulatory equilibrium.
- The primary driving force for VR is the pressure gradient between the mean systemic filling pressure (MSFP) and the right atrial pressure (RAP).
- MSFP reflects the total stressed volume in the vasculature and is increased by fluid infusion and sympathetic stimulation.
- RAP is the main force opposing venous return; it increases in right heart failure.
- Inspiration decreases intrathoracic pressure, which ↓RAP and ↑VR.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

