Pulmonary Circulation - The Low-Pressure Player
- Hallmark: High-flow, low-pressure, low-resistance system.
- Pulmonary Artery Pressure: ~25/10 mmHg (Mean ~15 mmHg).
- Contrast with Systemic (Aortic) Pressure: ~120/80 mmHg.
- Vessels: Shorter, more numerous, and more compliant than systemic vessels, leading to ↓ resistance.
- Pulmonary Vascular Resistance (PVR): Calculated as $PVR = (P_{pulm. artery} - P_{left atrium}) / Cardiac Output$.
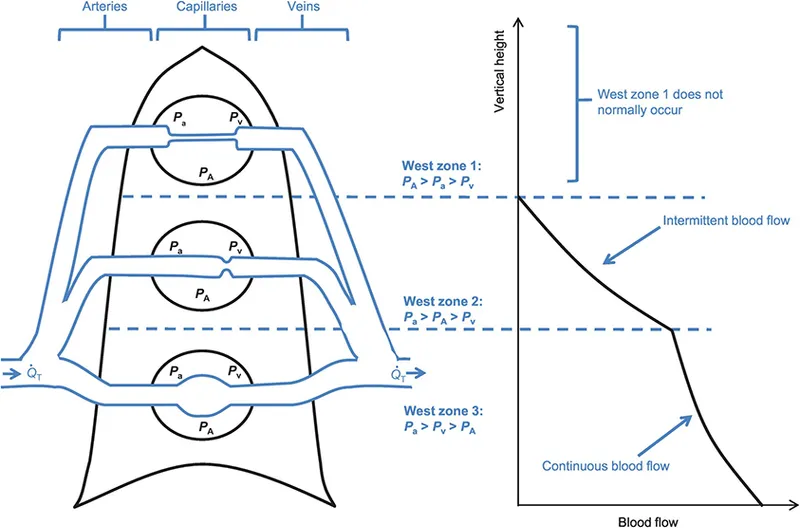
- Gravity Effects: Blood flow is unevenly distributed.
- Apex: Lower flow (Zone 1 & 2 physiology).
- Base: Higher flow (Zone 3 physiology).
⭐ Hypoxic Pulmonary Vasoconstriction (HPV): Unlike systemic circulation, hypoxia in the lungs causes vasoconstriction. This unique reflex diverts blood away from poorly ventilated alveoli, optimizing ventilation/perfusion (V/Q) matching.
Pulmonary Vascular Resistance - The Lung Squeeze
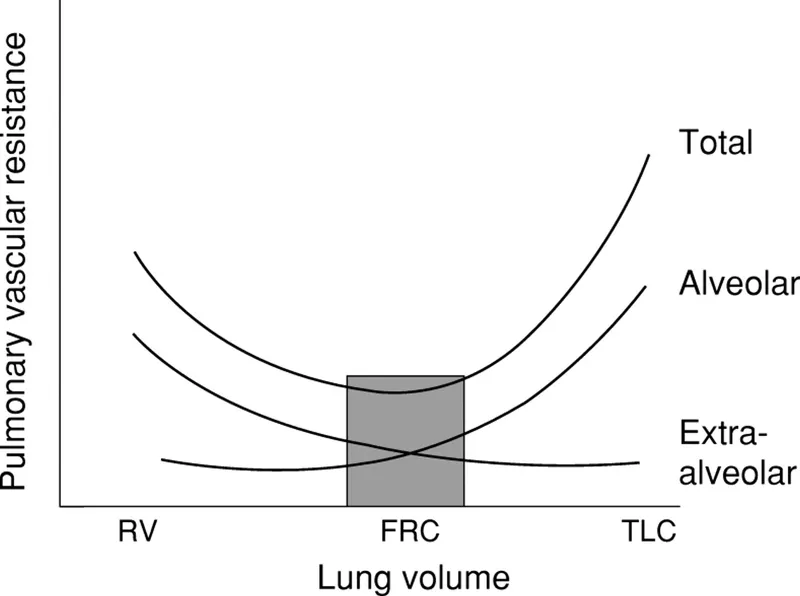
Pulmonary Vascular Resistance (PVR) is remarkably low (~1/10th of SVR). It varies with lung inflation in a distinct U-shaped relationship. The nadir, or lowest point of resistance, occurs at Functional Residual Capacity (FRC). Both high and low lung volumes increase PVR.
- Low Lung Volumes (approaching RV): Extra-alveolar vessels are compressed and become tortuous, increasing resistance.
- High Lung Volumes (approaching TLC): Alveolar capillaries are stretched thin and flattened by expanding alveoli, increasing resistance.
⭐ Alveolar hypoxia, unlike in systemic vessels, causes localized vasoconstriction. This "Hypoxic Pulmonary Vasoconstriction" is vital for V/Q matching, diverting blood from poorly ventilated lung regions to better-oxygenated ones.
Flow Regulation - The Oxygen Sensor
- Hypoxic Pulmonary Vasoconstriction (HPV): A unique, local response where low alveolar oxygen ($P_{A}O_2$) triggers vasoconstriction. This is the opposite of systemic circulation.
- Primary Goal: To optimize ventilation/perfusion (V/Q) matching by diverting blood from poorly ventilated lung segments to well-ventilated segments, thus maximizing gas exchange.
⭐ In conditions of global hypoxia, such as at high altitudes or in advanced COPD, widespread HPV can pathologically elevate pulmonary vascular resistance, leading to pulmonary hypertension.
- Modulators:
- Vasoconstrictors: Endothelin-1, Thromboxane A₂.
- Vasodilators: Nitric Oxide (NO), Prostacyclin.
Clinical Tie-ins - Pressure Problems
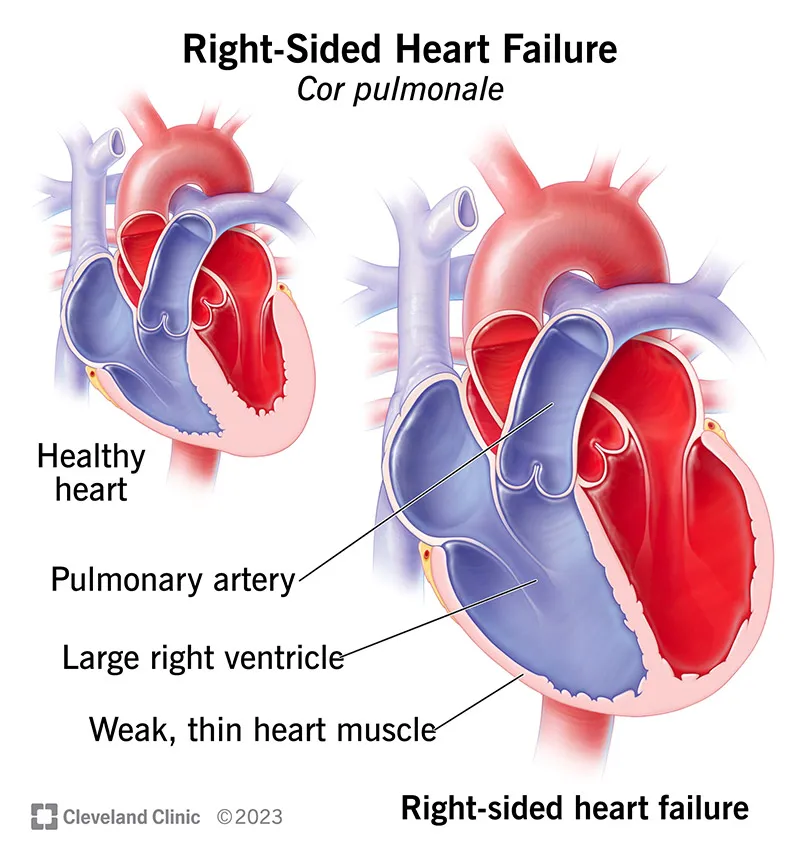
- Pulmonary Hypertension (PHTN): Defined by mean pulmonary arterial pressure (mPAP) > 20 mmHg at rest. Leads to right ventricular hypertrophy (RVH) and eventual cor pulmonale.
- Mechanisms:
- ↑ Pulmonary vascular resistance (PVR): Idiopathic, heritable (BMPR2), or from chronic hypoxia (lung disease).
- ↑ Left atrial pressure: Back-pressure from left heart failure (most common cause).
- Chronic thromboembolism (CTEPH).
- Mechanisms:
- Pulmonary Edema:
- Cardiogenic: ↑ PCWP > 18 mmHg from ↑ LA pressure.
- Non-cardiogenic (ARDS): Normal PCWP; due to ↑ capillary permeability.
⭐ PCWP approximates left atrial pressure. It's normal in PHTN from lung disease/hypoxia but elevated in PHTN from left heart failure.
High‑Yield Points - ⚡ Biggest Takeaways
- Pulmonary circulation is a low-pressure, low-resistance system, contrasting sharply with systemic circulation.
- Pulmonary Vascular Resistance (PVR) is uniquely lowest at functional residual capacity (FRC).
- Hypoxic pulmonary vasoconstriction is a critical mechanism to divert blood from poorly ventilated areas, optimizing V/Q matching.
- Normal pulmonary artery pressure is ~25/10 mmHg; mean PAP >20 mmHg at rest defines pulmonary hypertension.
- Perfusion is gravity-dependent, being highest at the lung bases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

