V/Q Basics - The Lung's Balancing Act
- Ventilation (V): Air reaching the alveoli for gas exchange.
- Perfusion (Q): Blood flow through alveolar capillaries.
- Goal: Efficiently match airflow to blood flow. The ideal system-wide $V/Q$ ratio is ~0.8.
-
**Gravity's Influence (Upright Lung):
- Apex (Zone 1): Highest $V/Q$. Alveolar pressure can exceed blood pressure. Less perfusion. (Physiological dead space).
- Base (Zone 3): Lowest $V/Q$. Blood flow is highest due to gravity. (Physiological shunt).
-
Compensation Mechanism:
- Hypoxic Vasoconstriction: Pulmonary arterioles constrict in response to low alveolar O₂, shunting blood to better-ventilated lung regions.
⭐ Both ventilation and perfusion are greatest at the lung base; however, perfusion increases more significantly than ventilation from apex to base.
Physiologic V/Q Zones - Apex to Base Story
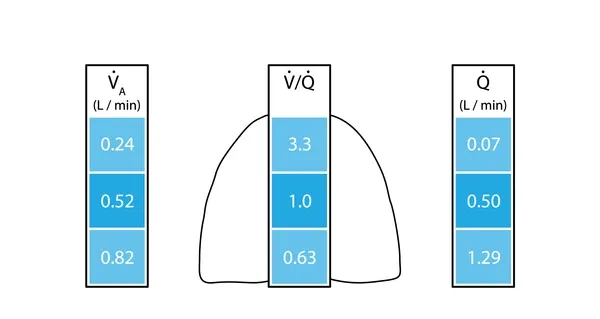
In the upright lung, gravity dictates ventilation (V) and perfusion (Q), creating three zones. Both V & Q are lowest at the apex and highest at the base, but perfusion's increase is more pronounced, altering the $V/Q$ ratio.
-
Zone 1 (Apex): V > Q → High $V/Q$ ratio.
- Pressure: $P_A > P_a > P_v$.
- Result: Physiologic dead space.
-
Zone 2 (Middle): V ≈ Q → Ideal $V/Q$ ratio (~1.0).
- Pressure: $P_a > P_A > P_v$.
- Result: Optimal gas exchange.
-
Zone 3 (Base): Q > V → Low $V/Q$ ratio.
- Pressure: $P_a > P_v > P_A$.
- Result: Physiologic shunt.
⭐ Both ventilation and perfusion are greatest at the lung base. However, perfusion (Q) increases more than ventilation (V) down the lung, causing the V/Q ratio to be lowest at the base.
V/Q Mismatch - Shunt vs. Dead Space
-
Ventilation/Perfusion ($V/Q$) Ratio: Aims to match alveolar ventilation to pulmonary blood flow. Normal $V/Q$ ≈ 0.8. Mismatch is the most common cause of hypoxemia.
-
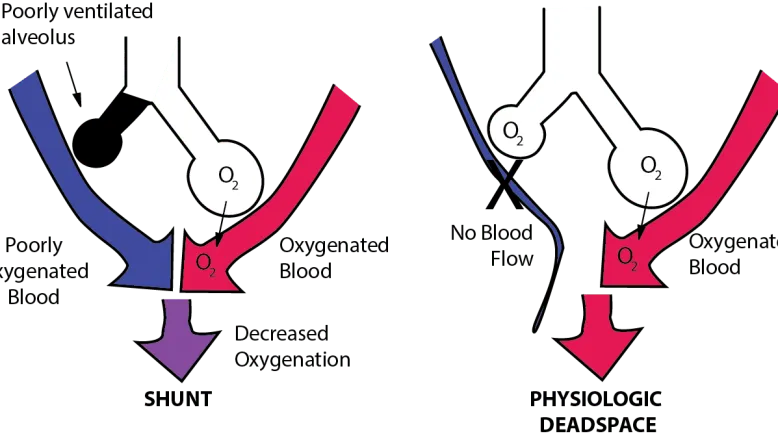
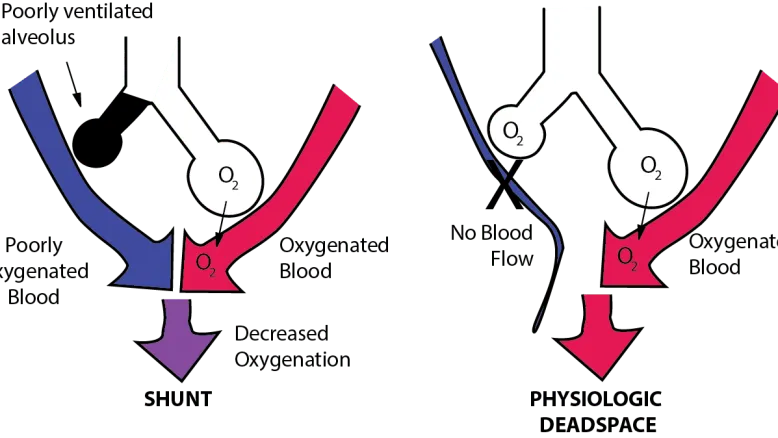
Shunt ($V/Q = 0$):
- Pathophysiology: Perfusion without ventilation ($V=0$). Blood bypasses non-ventilated alveoli.
- Causes: Atelectasis, pneumonia, pulmonary edema, intracardiac shunts.
- Correction: Hypoxemia does not correct with 100% O₂.
-
Dead Space ($V/Q \to \infty$):
- Pathophysiology: Ventilation without perfusion ($Q=0$). Air ventilates unperfused alveoli.
- Causes: Pulmonary embolism, emphysema, cardiogenic shock.
- Correction: Hypoxemia does correct with 100% O₂.
⭐ In a true shunt (e.g., large atelectasis), the A-a gradient is significantly widened and is not corrected by supplemental oxygen, as the shunted blood never gets exposed to the high FiO₂.
Clinical V/Q - The Patient Picture
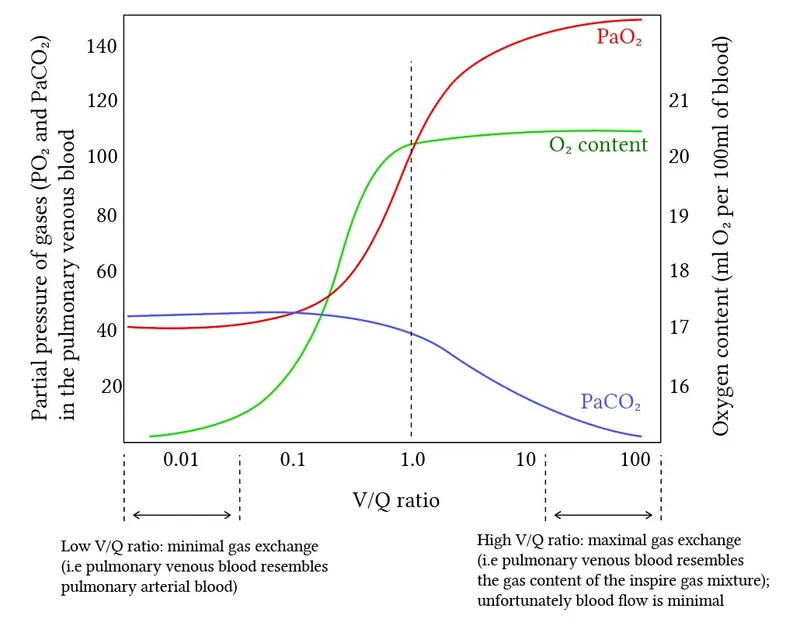
- V/Q mismatch is the most common cause of hypoxemia, reflected by an ↑ A-a gradient ($P_A O_2 - P_a O_2$).
-
Low V/Q (Shunt): V/Q → 0
- Perfusion without ventilation.
- Causes: Pneumonia, pulmonary edema, atelectasis.
- Hypoxemia does not correct with 100% O₂.
-
High V/Q (Dead Space): V/Q → ∞
- Ventilation without perfusion.
- Causes: Pulmonary embolism, emphysema, cardiogenic shock.
- Hypoxemia corrects with 100% O₂.
⭐ A key distinction: Shunt-induced hypoxemia is refractory to supplemental O₂, whereas dead space-induced hypoxemia is not. This is because O₂ can't reach blood in a true shunt.
High‑Yield Points - ⚡ Biggest Takeaways
- The ideal V/Q ratio is ~0.8 for optimal gas exchange.
- Lung apex: High V/Q (physiologic dead space) due to lower perfusion.
- Lung base: Low V/Q (physiologic shunt) due to higher perfusion.
- Hypoxic vasoconstriction diverts blood from poorly ventilated to well-ventilated areas, improving V/Q matching.
- V/Q mismatch is a major cause of hypoxemia.
- Pulmonary embolism causes dead space (↑ V/Q); pneumonia causes a shunt (↓ V/Q).
- Hypoxemia from mismatch is correctable with 100% O2.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

