Acute Ventilatory Response - The Initial Huff & Puff
- Phase I (Immediate): Abrupt ↑ in ventilation at exercise onset.
- Neural-driven: Not chemical. Central command from the motor cortex and feedback from muscle/joint proprioceptors stimulate medullary respiratory centers.
- Phase II (Slower): Gradual increase to match metabolic demand.
- Humoral-driven: Fine-tuning via chemoreceptors sensing ↑ $P_{CO_2}$ and $[H^+]$.
⭐ During moderate exercise, arterial $P_{aO_2}$ and $P_{aCO_2}$ remain remarkably constant, as alveolar ventilation increases in proportion to metabolic output.
Gas Exchange Dynamics - The O₂-CO₂ Swap Meet
-
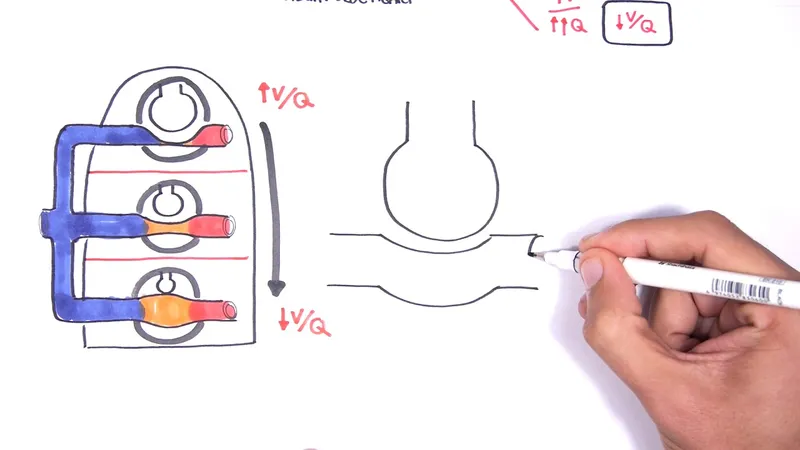
Pulmonary Blood Flow & V/Q Matching:
- Cardiac output ↑, leading to ↑ pulmonary blood flow.
- Recruits and distends apical capillaries, improving ventilation/perfusion (V/Q) matching throughout the lung.
- The V/Q ratio becomes more uniform, optimizing gas exchange efficiency.
-
Oxygen Diffusion & Transport:
- O₂ diffusing capacity ↑ up to 3x due to ↑ surface area and steeper pressure gradients.
- Arterial-venous O₂ difference (a-vO₂ diff) widens significantly as muscles extract more O₂.
⭐ During moderate exercise, PaO₂ and PaCO₂ remain remarkably stable due to tight coupling between ventilation and metabolic demand. They only change significantly near the lactate threshold.
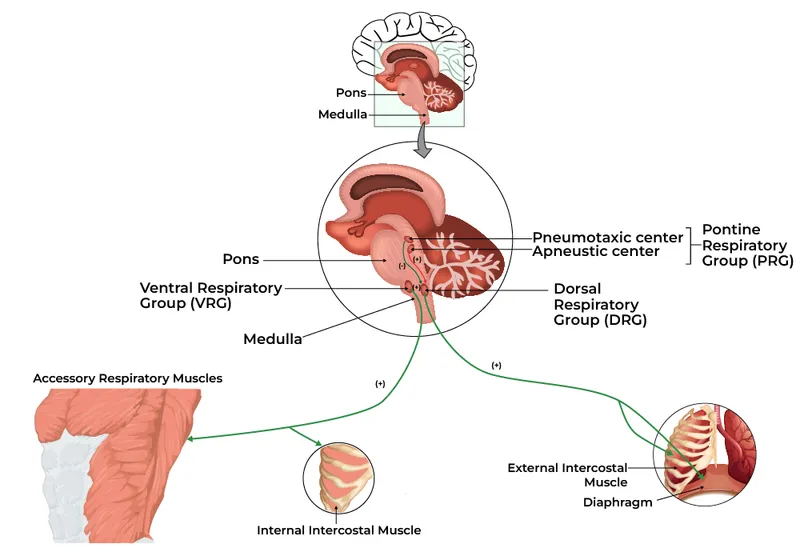
Ventilatory Control - The Brain's Breath Boss
-
Central Command: The primary driver. The motor cortex, upon initiating muscle contraction, sends feed-forward signals to the medullary respiratory centers. This anticipates metabolic needs.
-
Peripheral Feedback Loop:
- Proprioceptors: Mechanoreceptors in muscles and joints signal movement, providing rapid feedback.
- Chemoreceptors: Fine-tune ventilation. Carotid/aortic bodies respond to ↑ arterial $PCO_2$ and ↑ $H^+$. Hypoxia ($PO_2$ < 60 mmHg) becomes a potent stimulus.
⭐ The initial, abrupt ↑ in ventilation at exercise onset is due to central command and muscle mechanoreceptor feedback, before arterial $PCO_2$ or $PO_2$ change significantly.
Chronic Adaptations - The Efficient Engine
- ↑ $V̇O_{2}$ max: Primarily from enhanced pulmonary diffusion capacity.
- ↑ Respiratory Muscle Strength: Diaphragm and intercostals become stronger, resisting fatigue.
- ↓ Ventilatory Equivalents ($V_E/V̇O_2$, $V_E/V̇CO_2$): Improved efficiency at submaximal intensities.
⭐ At a given submaximal workload, a trained athlete has a lower respiratory rate and minute ventilation than an untrained individual.
High‑Yield Points - ⚡ Biggest Takeaways
- Minute ventilation (VE) ↑ proportionally to metabolic demand, driven first by tidal volume, then respiratory rate.
- Arterial PaO₂ and PaCO₂ remain remarkably stable during moderate exercise due to tight homeostatic control.
- Venous PCO₂ (PvCO₂) ↑ due to increased CO₂ production by exercising muscles.
- The arterial-venous (A-v) O₂ difference widens significantly, reflecting increased O₂ extraction by tissues.
- Ventilation-perfusion (V/Q) matching improves, becoming more uniform across the lungs.
- Pulmonary vascular resistance ↓ as vessels recruit and distend to handle increased cardiac output.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

