Definition of Lung Compliance - The Lung's Stretchiness
-
Lung Compliance (CL) is the measure of the lung's ability to stretch and expand in response to pressure changes. It quantifies the lung's "distensibility."
-
It's the inverse of elastance (stiffness).
- High Compliance: Lungs are easy to inflate (e.g., emphysema). Think of a well-used party balloon.
- Low Compliance: Lungs are stiff and difficult to inflate (e.g., fibrosis, ARDS). Think of a thick, new balloon.
-
Formula:
- $C_L = \frac{\Delta V_L}{\Delta P_{TP}}$
- $\Delta V_L$: Change in lung volume.
- $\Delta P_{TP}$: Change in transpulmonary pressure (Alveolar Pressure - Intrapleural Pressure).
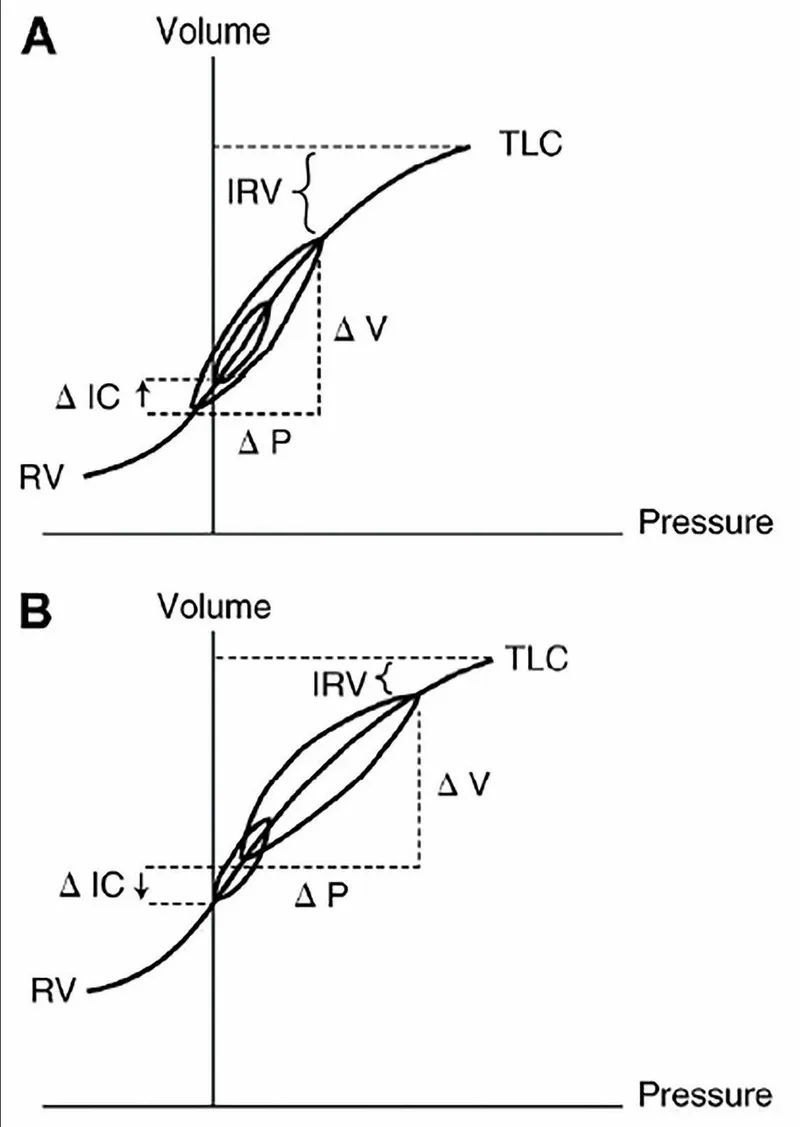 , normal, and low (fibrosis) lung compliance)
, normal, and low (fibrosis) lung compliance)
- Key Determinants:
- Elastic Properties: Intrinsic stretchiness from elastin and collagen fibers in the lung parenchyma.
- Surface Tension: Force at the air-liquid interface in alveoli, which is reduced by surfactant.
⭐ In a healthy adult, the compliance of the lungs and chest wall combined is approximately 100 mL/cm H₂O, which is about half the compliance of the lungs alone (200 mL/cm H₂O).
Factors Affecting Compliance - What Helps & Hinders
Lung compliance ($C = \Delta V / \Delta P$) is dictated by the lung's intrinsic elastic recoil and the surface tension at the alveolar air-fluid interface. Factors altering these properties will change compliance.
| Factors Increasing Compliance (↑C) | Factors Decreasing Compliance (↓C) - "Stiff Lung" |
|---|---|
| * Emphysema/COPD: Destruction of elastic fibers results in a "floppy," easily distended lung. | * Pulmonary Fibrosis: Excess collagen deposition makes the lung stiff and difficult to inflate. |
| * Normal Aging: Gradual loss of elastic recoil increases compliance. | * Pulmonary Edema/Pneumonia: Fluid or consolidation in alveolar spaces resists expansion. |
| * ARDS: Diffuse alveolar damage, edema, and loss of surfactant. | |
| * Neonatal RDS: Surfactant deficiency causes high surface tension. |
Clinical Significance - Floppy vs. Stiff Lungs
-
High Compliance (Floppy Lungs): Lungs are easier to distend but have poor elastic recoil.
- Causes: Emphysema (e.g., α1-antitrypsin deficiency), normal aging.
- Mechanism: Loss of elastic fibers makes lungs easy to inflate but difficult to exhale from.
- Clinical Result: Leads to air trapping, ↑ Functional Residual Capacity (FRC), and a "barrel chest." Expiration becomes an active process, increasing the work of breathing.
-
Low Compliance (Stiff Lungs): Lungs are harder to distend, requiring greater pressure.
- Causes: Pulmonary fibrosis, ARDS, pulmonary edema, Neonatal RDS.
- Mechanism: Increased fibrous tissue or alveolar fluid/inflammation stiffens the lung.
- Clinical Result: Requires ↑ inspiratory work to inflate the lungs.
⭐ In Neonatal Respiratory Distress Syndrome (NRDS), a deficiency of surfactant increases alveolar surface tension. This causes widespread atelectasis (alveolar collapse), severely ↓ lung compliance.
- Lung compliance is the change in lung volume per unit change in transpulmonary pressure ($C_L = \Delta V / \Delta P_{tp}$).
- It is the primary measure of the distensibility or "stretchiness" of the lungs.
- High compliance (e.g., emphysema, aging) means lungs are easy to inflate but have ↓ elastic recoil.
- Low compliance (e.g., fibrosis, ARDS, pneumonia) indicates "stiff" lungs that are difficult to inflate.
- Compliance is the inverse of elastance ($C = 1/E$).
- Surfactant increases lung compliance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

