Sensory Input - Pressure & Gas Detectors
-
Baroreceptors (Pressure): High-pressure sensors detecting arterial stretch.
- Carotid Sinus: Monitors BP to the brain; afferents via Glossopharyngeal n. (CN IX).
- Aortic Arch: Monitors systemic BP; afferents via Vagus n. (CN X).
-
Chemoreceptors (Gas/pH): Detect changes in arterial $P_{O_2}$, $P_{CO_2}$, and pH.
- Carotid Bodies: Primary peripheral sensors for hypoxemia (↓$P_{O_2}$); afferents via CN IX.
- Aortic Bodies: Afferents via CN X.
⭐ The carotid sinus baroreceptor is most critical for minute-to-minute regulation of arterial blood pressure.
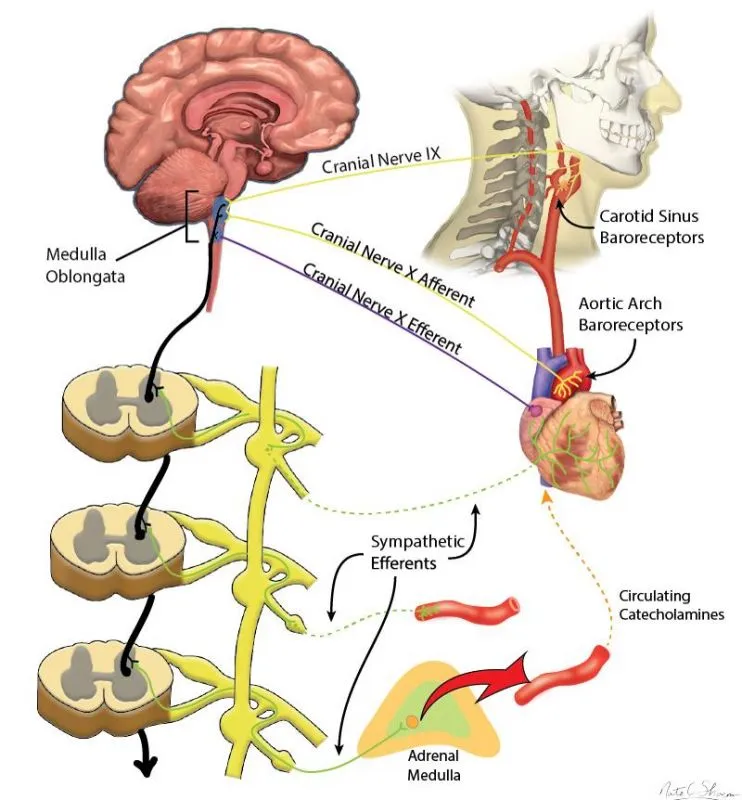
ANS Output - The Push-Pull System
The ANS fine-tunes cardiac function via a constant push-pull between its two branches. Sympathetic stimulation generally acts as an accelerator, while parasympathetic acts as a brake.

| Action | Sympathetic (NE) | Parasympathetic (ACh) |
|---|---|---|
| Heart Rate | ↑ via $\beta_1$ receptors | ↓ via M$_2$ receptors |
| Contractility | ↑ via $\beta_1$ receptors | ↓ (atria only) via M$_2$ |
| Vascular Tone | ↑ Constriction via $\alpha_1$ | Minimal direct effect |
- **$\beta_1$:** Located in the heart. Think **1** heart.
- **$\beta_2$:** Lungs & skeletal muscle vessels. Think **2** lungs. Causes vasodilation.
- **$\alpha_1$:** Smooth muscle of most arterioles, causing vasoconstriction.
- **M$_2$:** Heart (SA/AV nodes, atria).
⭐ High-Yield: During exercise, sympathetic outflow triggers generalized $\alpha_1$-mediated vasoconstriction to divert blood from non-essential organs. However, local metabolites and circulating epinephrine (acting on $\beta_2$ receptors) cause vasodilation in skeletal and coronary vessels.
Central Command - The Brain's HQ
The medulla is the primary integration center, modulated by higher cortical areas.
- Medulla Oblongata:
- NTS (Nucleus Tractus Solitarius): Integrates baro/chemoreceptor signals.
- RVLM (Rostral Ventrolateral Medulla): Governs sympathetic outflow.
- Nucleus Ambiguus: Provides parasympathetic (vagal) outflow to the heart.
- Hypothalamus & Cortex: Adjust cardiovascular function for exercise, temperature, and emotional responses.
⭐ Central command from the cortex initiates ↑ heart rate and contractility during exercise before feedback from working muscles arrives.
Key Reflexes - Clinical Tie-Ins
-
Valsalva Maneuver: Forced expiration against a closed glottis; evaluates autonomic function.
-
Cushing Reflex: Triad from ↑ intracranial pressure.
- Hypertension (↑ SBP)
- Bradycardia (↓ HR)
- Irregular Respirations
-
Bainbridge (Atrial) Reflex: ↑ atrial volume → atrial stretch → reflex ↑ HR. Prevents blood backup.
⭐ The Valsalva maneuver (specifically phase 4) increases vagal tone and is used clinically to terminate paroxysmal supraventricular tachycardias (PSVTs).
High‑Yield Points - ⚡ Biggest Takeaways
- Baroreceptors in the carotid sinus (CN IX) and aortic arch (CN X) are crucial for short-term BP regulation.
- The Bainbridge reflex increases heart rate in response to ↑ atrial stretch, mediated by vagal afferents.
- Peripheral chemoreceptors respond to ↓ PaO₂, ↑ PaCO₂, and ↓ pH, leading to systemic vasoconstriction.
- The Cushing reflex-hypertension, bradycardia, irregular respiration-is a sign of ↑ intracranial pressure.
- Vasovagal syncope results from a paradoxical activation of the vagus nerve, causing sudden hypotension and bradycardia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

