Mechanism of Action - T-Cell Takedown
- Polyclonal (e.g., Antithymocyte Globulin) and monoclonal (e.g., Alemtuzumab) antibodies bind to a variety of antigens on the T-cell surface.
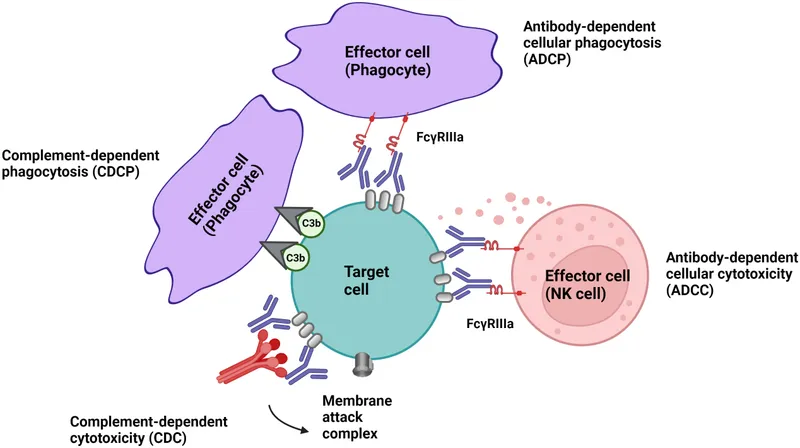
- This tagging marks the T-cell for destruction through:
- Complement-Dependent Cytotoxicity (CDC): The antibody activates the complement system, leading to cell lysis.
- Antibody-Dependent Cell-Mediated Cytotoxicity (ADCC): NK cells and phagocytes recognize the antibody and destroy the T-cell.
- Alemtuzumab specifically targets the CD52 antigen.
⭐ First-dose reactions, like Cytokine Release Syndrome (CRS), can be severe. This is due to the initial massive activation and lysis of T-cells, releasing a flood of inflammatory cytokines.
Polyclonal Antibodies - The Broadside
- Agents: Anti-thymocyte Globulin (ATG) derived from horse or rabbit serum.
- Mechanism: A "broadside" attack. Binds to a wide array of T-cell surface antigens (CD2, CD3, CD4, etc.), triggering complement-dependent lysis and clearance by phagocytes. Causes profound T-cell depletion.
- Clinical Use:
- Induction therapy for preventing rejection in solid organ transplants (especially kidney).
- Treatment of severe, steroid-resistant acute rejection.
- Adverse Effects:
- ⚠️ Cytokine Release Syndrome (CRS): Systemic inflammation (fever, rigors, hypotension) after the first dose due to massive cytokine release from lysed T-cells.
- Serum Sickness: Type III hypersensitivity (fever, rash, arthralgia) days to weeks later.
- Leukopenia, thrombocytopenia.
- Increased risk of infection (CMV) & PTLD.
⭐ High-Yield: To manage expected Cytokine Release Syndrome, pre-medicate patients with corticosteroids, acetaminophen, and antihistamines before the first ATG infusion.
Monoclonal Antibodies - The CD52 Sniper
-
Alemtuzumab: A humanized monoclonal antibody that targets the CD52 antigen.
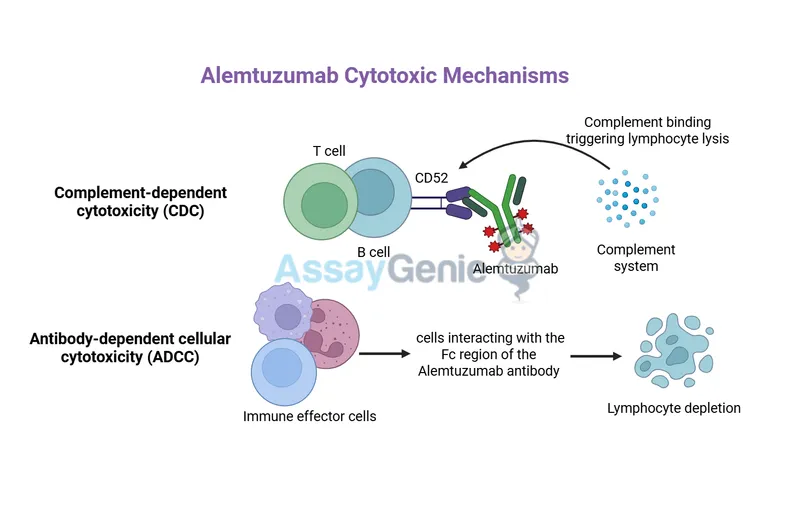
- Mechanism: Binds to CD52 on T-cells, B-cells, NK cells, monocytes, and macrophages. This triggers complement-dependent cytotoxicity (CDC) and antibody-dependent cell-mediated cytotoxicity (ADCC).
- Effect: Causes rapid, profound, and long-lasting depletion of lymphocytes.
-
Primary Uses:
- Relapsing-Remitting Multiple Sclerosis (MS).
- Chronic Lymphocytic Leukemia (CLL).
- Formerly used in transplant rejection.
-
Major Adverse Effects:
- Pancytopenia: Especially severe lymphopenia, requiring prophylaxis against opportunistic infections (e.g., PJP, Herpesviruses).
- Infusion Reactions: Pre-medication is necessary.
- Secondary Autoimmunity: Thyroid disease, ITP, nephropathies.
⭐ High-Yield: A major long-term complication is the development of secondary autoimmune diseases (e.g., Graves' disease, ITP), which can occur in up to 50% of patients months to years after treatment.
📌 Mnemonic: Alemtuzumab causes elemination of CD52 cells.
Adverse Effects - The Aftermath
- Cytokine Release Syndrome (CRS):
- Systemic inflammation from rapid T-cell lysis.
- Presents with fever, chills, rigors, headache, hypotension.
- ⚠️ Most severe with the first dose.
- Increased Infection Risk:
- High risk for opportunistic infections.
- Key pathogens: CMV, PJP, BK virus.
- Requires prophylactic antimicrobial therapy.
- Malignancy:
- Increased risk of Post-Transplant Lymphoproliferative Disorder (PTLD), usually EBV-driven.
- Skin cancers.
- Drug-Specific:
- Alemtuzumab: Pancytopenia, autoimmune thyroiditis.
⭐ Muromonab-CD3 (OKT3) is notorious for causing a severe, potentially fatal CRS after the first dose, often called the "first-dose reaction."
High‑Yield Points - ⚡ Biggest Takeaways
- Alemtuzumab targets CD52 on most lymphocytes, used for MS and CLL; causes profound, prolonged lymphopenia.
- Muromonab-CD3 (OKT3) is a murine antibody against the T-cell CD3 receptor, causing rapid T-cell depletion.
- First dose of Muromonab often causes a severe cytokine release syndrome.
- Basiliximab and daclizumab are monoclonal antibodies targeting the IL-2 receptor (CD25).
- Primarily used for prophylaxis of acute rejection in renal transplantation.
- Major risks for all include increased susceptibility to infection and malignancy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

